Stem cell therapy is rapidly gaining attention as a transformative approach to treating chronic illnesses, and diabetes stands out as one of the most intensively studied conditions in this field. In Thailand, advancements in stem cell research and clinical applications are progressing steadily, particularly in relation to both Type 1 and Type 2 diabetes. Although stem cell–based interventions have not yet become part of routine medical care, ongoing research and early-stage clinical trials suggest a future where diabetes management could be significantly improved—or even fundamentally changed—through regenerative medicine.
Stem Cell-Based Strategies for Type 1 Diabetes
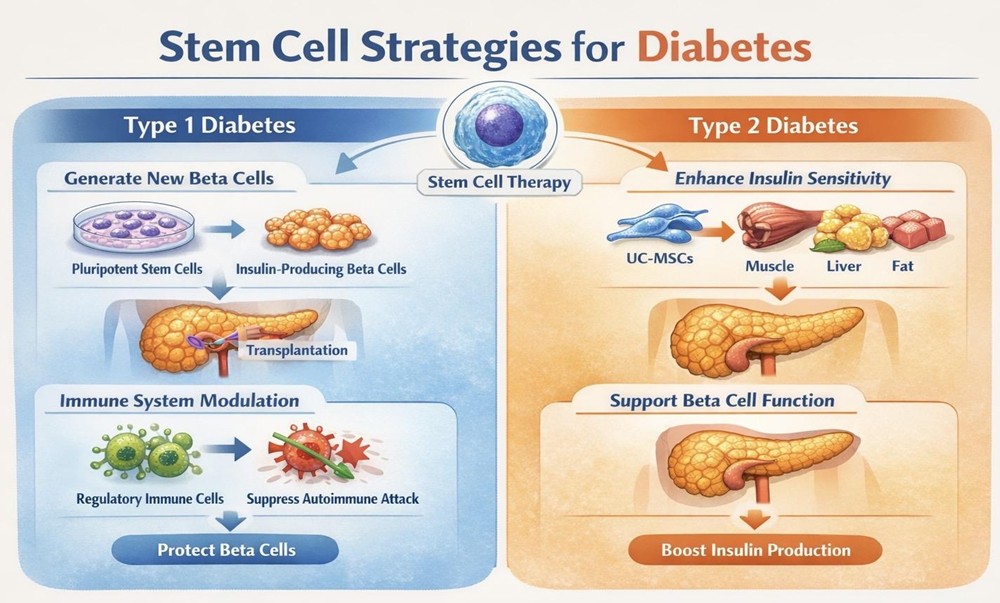
For individuals with Type 1 diabetes, the destruction of beta cells presents a significant challenge. Stem cell research is focused on two key objectives: restoring the lost insulin-producing cells and preventing the immune system from attacking them again.
One promising approach involves generating new beta cells from pluripotent stem cells. These versatile cells have the capacity to develop into nearly any cell type in the body. Scientists can guide them in laboratory settings to become insulin-producing cells, which may then be transplanted into patients. Early experimental studies have shown that such cells can survive and function in preclinical models, offering hope for restoring natural insulin production.
Another area of research aims to address the autoimmune nature of T1D. Scientists are exploring ways to modify or “retrain” the immune system using stem cells. By producing immune cells that are more tolerant, or by suppressing harmful immune responses, it may be possible to protect both existing and newly introduced beta cells from destruction. This dual strategy—cell replacement combined with immune regulation—could be essential for achieving long-term success.
Stem Cell Applications for Type 2 Diabetes
While Type 2 diabetes is primarily associated with insulin resistance, it often evolves into a condition where insulin production is also impaired. This makes it a complex disorder requiring multifaceted treatment strategies.
Stem cell therapy offers potential benefits by improving how the body responds to insulin. Mesenchymal stem cells (MSCs), particularly those derived from umbilical cord tissue (UC-MSCs), have demonstrated anti-inflammatory properties that may enhance insulin sensitivity. By reducing chronic inflammation—a key factor in insulin resistance—these cells can help metabolic tissues such as muscle, liver, and fat function more effectively in glucose regulation.
In addition to enhancing insulin responsiveness, stem cell research is also focused on preserving or regenerating pancreatic beta cells in individuals with T2D. Supporting the survival and function of these cells could slow disease progression and reduce the need for medications or insulin therapy. This combined effect—improving both insulin action and production—represents a promising avenue for more comprehensive disease management.
Advancements and Research in Thailand
Thailand has become an increasingly important center for regenerative medicine and medical tourism. The country’s healthcare system, combined with growing investment in biotechnology, has created a supportive environment for stem cell research.
Several research institutions and medical centers in Thailand are actively studying the use of stem cells for diabetes treatment. In clinical practice, procedures such as islet cell transplantation have already been introduced. This technique involves transferring clusters of insulin-producing cells from a donor pancreas into a diabetic patient. While it can improve glucose control, particularly in individuals with Type 1 diabetes, it also requires the use of immunosuppressive drugs to prevent rejection.
In parallel, researchers are investigating the potential of UC-MSC stem cells and other stem cell types in both laboratory and early clinical settings. These efforts are contributing to a deeper understanding of how regenerative therapies can be safely and effectively applied to diabetes care.
Future Directions and Emerging Technologies
The outlook for stem cell therapy in diabetes treatment is increasingly optimistic, especially as new technologies continue to evolve.
One of the most exciting developments is the integration of gene-editing techniques, such as CRISPR-Cas9, with stem cell therapy. This approach allows scientists to modify stem cells at the genetic level, potentially enhancing their performance or making them less visible to the immune system. For instance, engineered stem cells could be designed to avoid immune rejection, reducing or eliminating the need for long-term immunosuppressive medications.
Another important advancement is the move toward personalized medicine. By using a patient’s own cells, researchers can create customized stem cell therapies tailored to an individual’s unique biological and immune profile. This approach not only minimizes the risk of rejection but also increases the likelihood of long-term success. Personalized stem cell treatments could play a key role in delivering more precise and effective care for people with diabetes.
Conclusion
Stem cell therapy represents a promising and rapidly evolving field in the treatment of diabetes, offering new hope for individuals affected by both Type 1 diabetes and Type 2 diabetes forms of the disease. By focusing on regenerating insulin-producing cells, improving insulin sensitivity, and addressing immune system dysfunction, researchers are making significant strides toward more effective and potentially curative therapies.
In Thailand, continued investment in research, combined with a strong medical infrastructure, is positioning the country as a leader in this innovative area of healthcare. While challenges remain and more clinical validation is needed, the progress being made suggests that stem cell–based treatments could play a transformative role in the future of diabetes management.

