Ovarian health is central to a woman’s reproductive potential and overall physiological balance. Beyond producing eggs, the ovaries regulate essential hormones—primarily estrogen and progesterone—that influence numerous bodily systems. These hormones play key roles in maintaining menstrual cycles, preserving bone density, supporting cardiovascular health, and stabilizing mood. When ovarian function begins to decline, it can disrupt this delicate hormonal balance, leading to fertility challenges and broader health concerns.
There are multiple causes of reduced ovarian function. Premature ovarian insufficiency (POI), natural aging and menopause, autoimmune conditions, and the effects of medical treatments can all impair ovarian activity. Regardless of the underlying cause, diminished ovarian function often results in hormonal imbalances, irregular or absent menstruation, infertility, and symptoms that impact both physical and emotional well-being.
In recent years, regenerative medicine has introduced new possibilities for addressing these issues. Among the most promising innovations is stem cell therapy, which focuses on repairing and revitalizing damaged tissues rather than simply managing symptoms. In Thailand, a recognized center for advanced medical care, umbilical cord-derived mesenchymal stem cell (UC-MSC) therapy is gaining attention as a potential approach to restoring ovarian function. This therapy aims to support natural hormone production, improve fertility outcomes, and enhance overall quality of life.
Mechanisms of Ovarian Restoration
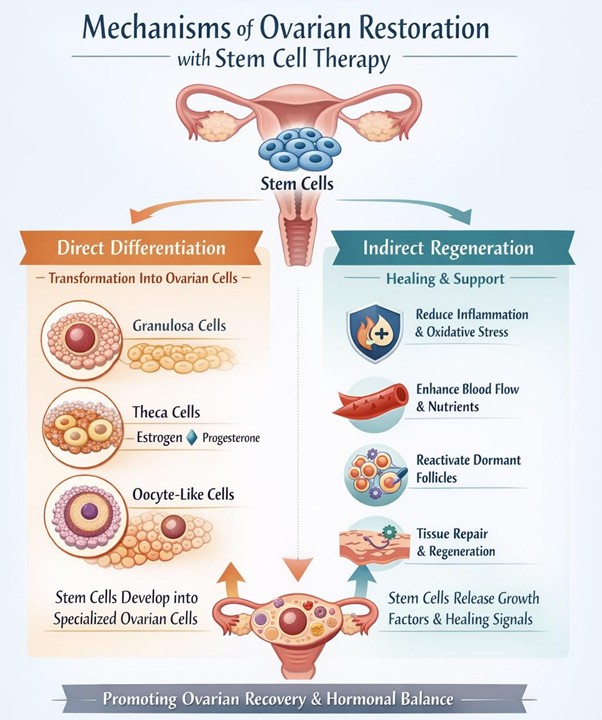
Stem cell therapy may improve ovarian function through both direct and indirect mechanisms.
The first approach involves differentiation into ovarian-specific cells. Certain types of stem cells, particularly pluripotent stem cells, have the capacity to develop into specialized ovarian cells under controlled laboratory conditions. These may include granulosa cells, which support egg development; theca cells, which produce key reproductive hormones; and in some experimental settings, even oocyte-like cells. By replenishing these essential components, stem cells may help rebuild the ovarian environment and support follicle development.
The second and more commonly observed mechanism in clinical settings is indirect regeneration. Stem cells typically do not replace ovarian cells directly. Instead, they release a variety of growth factors, cytokines, and anti-inflammatory molecules that enhance the body’s natural healing processes. These secretions help reduce inflammation and oxidative stress, both of which contribute to ovarian aging. They also promote angiogenesis, improving blood flow and nutrient delivery to ovarian tissue. Additionally, these signaling molecules can activate dormant follicles and support the survival and function of existing cells.
Through these combined effects, stem cell therapy may create a more favorable environment for ovarian recovery, potentially restoring hormone production and menstrual function.
Clinical Observations and Emerging Outcomes
Early clinical observations have shown encouraging results. Some women undergoing stem cell therapy have experienced the return of menstrual cycles after prolonged absence. Improvements in hormone levels, including increased estrogen and anti-Müllerian hormone (AMH), have also been reported. Imaging studies have occasionally revealed the reappearance of ovarian follicles, suggesting renewed activity within the ovaries.
In rare but notable cases, natural conception and successful pregnancies have occurred following treatment. While these outcomes are not guaranteed, they highlight the potential of stem cell therapy as a supportive option for women facing infertility due to ovarian dysfunction.
Key Areas of Application
One important area where this therapy is being explored is premature ovarian insufficiency. Women with POI experience a loss of ovarian function before the age of 40, often leading to infertility and early menopause symptoms. Stem cell therapy may help reactivate dormant follicles and restore hormone production, offering a possible alternative to conventional treatments.
Another focus is age-related ovarian decline. As women age, the number and quality of eggs decrease, eventually leading to menopause. Regenerative approaches such as stem cell therapy aim to rejuvenate ovarian tissue, potentially easing menopausal symptoms and supporting hormonal balance during this transition.
Stem cell therapy is also being investigated for women who have undergone cancer treatment. Chemotherapy and radiation can severely damage ovarian tissue, sometimes resulting in permanent infertility. By promoting tissue repair and regeneration, stem cell therapy may help restore ovarian function and improve reproductive prospects for cancer survivors.
Thailand as a Hub for Regenerative Therapies
Thailand has emerged as a leading destination for regenerative medicine, supported by modern healthcare infrastructure, skilled medical professionals, and a growing focus on innovative treatments. Clinics and research centers across the country are actively exploring the use of stem cell therapy for ovarian rejuvenation.
The treatment process typically begins with a thorough evaluation, including hormone testing, imaging studies, and a detailed medical history. Once a patient is deemed suitable, stem cells may be administered through intravenous infusion or targeted injection into the ovaries. Follow-up monitoring is essential, as improvements in hormone levels and ovarian activity often develop gradually over several months.
Early findings from clinical practices in Thailand suggest that many patients experience positive changes, including improved hormonal balance, more regular menstrual cycles, and enhanced overall well-being. While results can vary, these outcomes contribute to growing interest in this therapeutic approach.
Conclusion
Stem cell therapy represents a promising advancement in the field of women’s health. By addressing the underlying causes of ovarian dysfunction through tissue regeneration, immune modulation, and hormonal support, this therapy offers a comprehensive approach to restoring ovarian activity.
For women facing challenges such as premature ovarian insufficiency, menopause, or treatment-related ovarian damage, stem cell therapy may provide new hope. Beyond fertility, the potential benefits extend to improved energy levels, emotional stability, and long-term health.
As research continues to evolve, Thailand remains at the forefront of bringing these innovations into clinical practice. With ongoing advancements, stem cell therapy is poised to play an increasingly important role in shaping the future of reproductive and hormonal care.