Breakthroughs in Diabetic Wound Healing with Regenerative Medicine Thailand
The clinical challenge of chronic non-Healing ulcers represents one of the most debilitating complications for patients living with diabetes. These Wounds often persist for months or even years, significantly reducing quality of life and imposing a massive economic burden on healthcare systems globally. Conventional treatments frequently fail because the underlying physiological environment of a Diabetic patient is fundamentally altered, characterized by persistent inflammation, impaired vascularization, and a lack of essential growth factors. When a simple lesion refuses to close, the risk of systemic infection and lower-limb amputation increases exponentially. This critical situation has fueled the urgent search for advanced therapeutic interventions. We are now entering a transformative era where standard care is no longer the ceiling, as innovative biological therapies offer a chance to reset the Healing process at a cellular level.
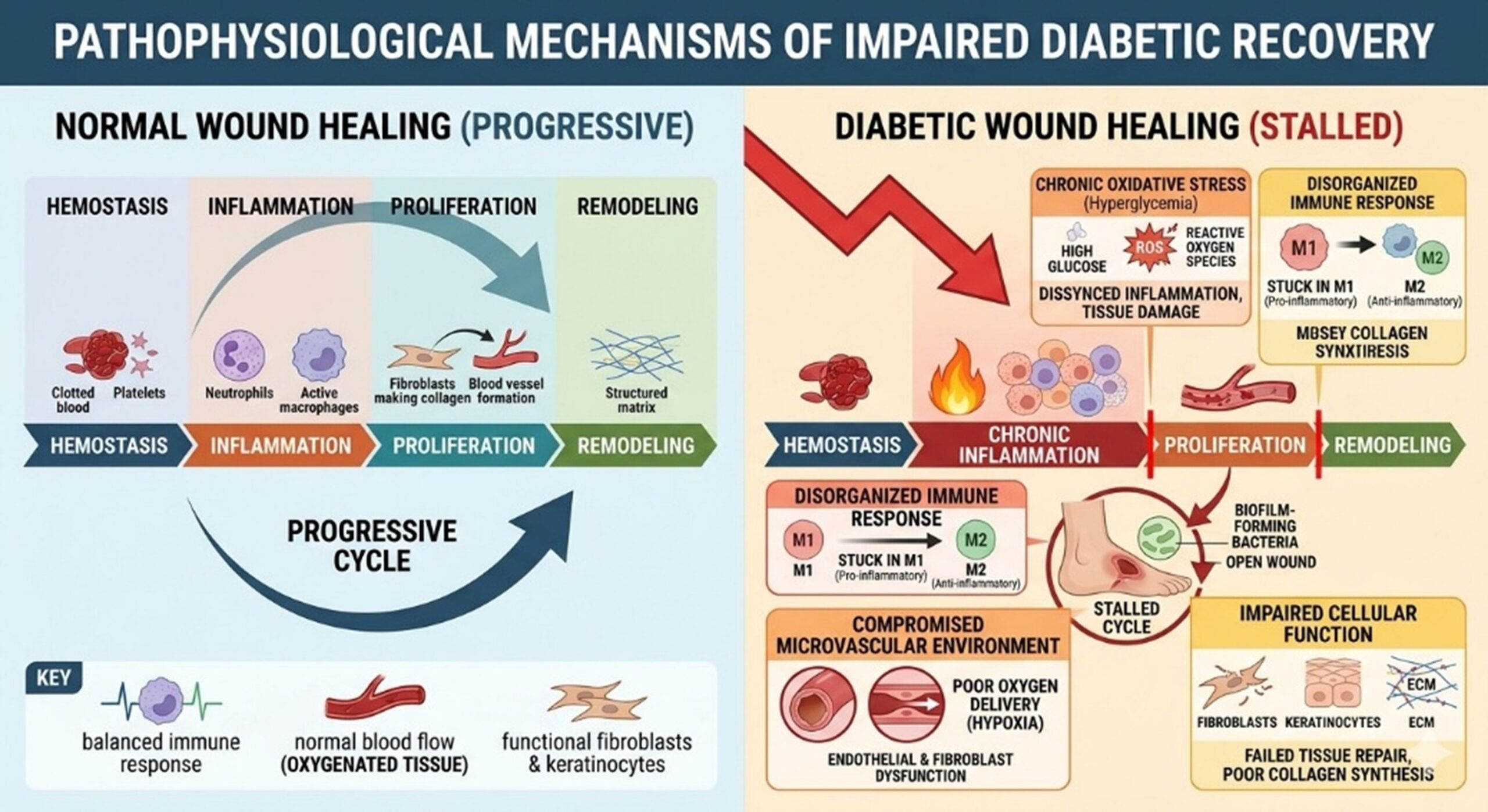
1.Pathophysiological Mechanisms of Impaired Diabetic Recovery
Diabetic Wounds are not merely slow-Healing cuts but are complex biological puzzles characterized by a stalled Healing cycle. In a healthy individual, Wound Healing progresses through four distinct phases: hemostasis, inflammation, proliferation, and remodeling. However, in Diabetic patients, high glucose levels create a state of chronic oxidative stress that traps the Wound in a permanent inflammatory phase. The excessive production of reactive oxygen species damages cellular DNA and proteins, leading to the dysfunction of fibroblasts and keratinocytes.
Furthermore, the microvascular environment is severely compromised. Hyperglycemia causes thickening of the capillary basement membrane and impairs the function of endothelial cells, resulting in poor oxygen delivery or hypoxia. Without adequate blood flow, the tissue lacks the nutrients required for repair. Additionally, the recruitment of immune cells is disorganized; macrophages, which should transition from a pro-inflammatory M1 phenotype to an anti-inflammatory M2 phenotype to promote repair, remain stuck in the aggressive M1 state. This biochemical imbalance prevents the formation of new extracellular matrix, leaving the Wound open and vulnerable to biofilm-forming bacteria.
2.Conventional Treatment Modalities and Their Clinical Limitations
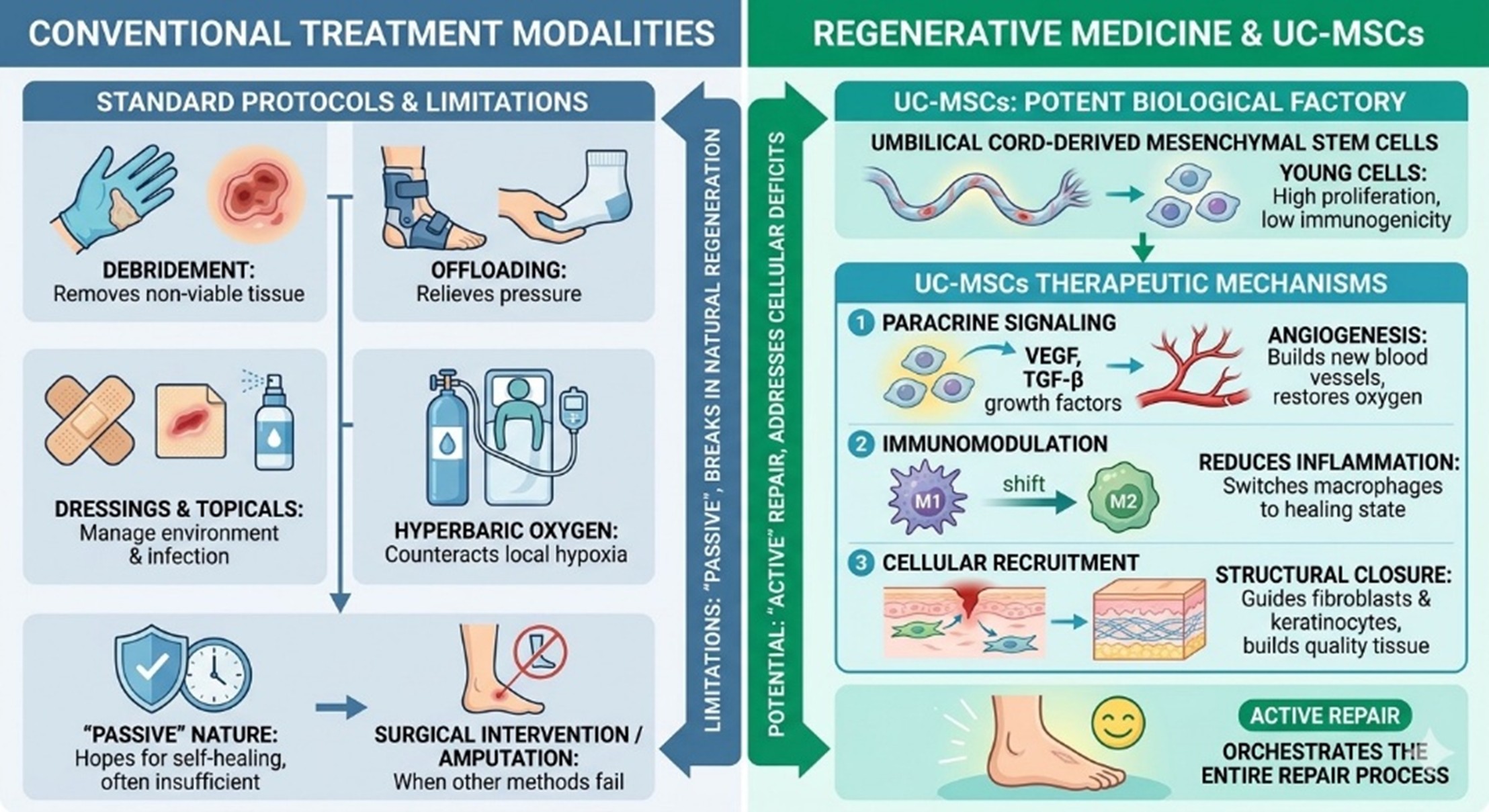
Current standard protocols for managing Diabetic ulcers primarily focus on Wound bed preparation. This typically involves aggressive debridement to remove necrotic tissue, offloading pressure from the affected site, and maintaining a moist environment through various dressings. While these steps are necessary, they are often insufficient for chronic cases because they do not address the systemic cellular deficits inherent in diabetes. Topical antibiotics and specialized silver-impregnated dressings are frequently used to manage bacterial load, yet they cannot stimulate the regeneration of lost tissue. Hyperbaric oxygen therapy has been employed to counteract local hypoxia, but its efficacy varies and requires expensive equipment and frequent hospital visits. The most significant limitation of traditional care is its passive nature; it attempts to protect the Wound while hoping the body heals itself. Unfortunately, in a Diabetic state, the body’s natural Regenerative toolkit is broken. When these methods fail, the final resort is often surgical intervention or amputation, which fails to solve the underlying biological dysfunction and leads to high mortality rates post-surgery.
3.The Therapeutic Potential of UC-MSCs in Regenerative Medicine Thailand
The limitations of traditional care have paved the way for Regenerative Medicine Thailand to integrate Umbilical Cord-Derived Mesenchymal Stem Cells (UC-MSCs) into clinical practice. UC-MSCs are particularly potent because they are young cells with higher proliferative capacity and lower immunogenicity compared to adult bone marrow cells. Their mechanism of action in Diabetic Wound Healing is multifaceted, acting as a biological factory that orchestrates the entire repair process.
One primary mechanism is the paracrine signaling effect. UC-MSCs secrete a diverse array of cytokines and growth factors, such as Vascular Endothelial Growth Factor (VEGF) and Transforming Growth Factor-beta (TGF-β), which directly stimulate angiogenesis. By building new blood vessels, these cells restore the oxygen supply to the starved tissue. Moreover, MSCs possess unique immunomodulatory properties. They can actively signal the local environment to shift macrophages from the destructive M1 state to the Healing M2 state, effectively turning off chronic inflammation. They also facilitate the migration of fibroblasts and keratinocytes to the Wound site, ensuring the structural closure of the skin barrier through the deposition of high-quality collagen rather than disorganized scar tissue.
4.Future Perspectives of MSC Therapy in Thailand for Diabetic Wound Healing
Thailand has positioned itself as a sophisticated hub for biotechnology, making the future of Diabetic Wound Healing via stem cells promising. The nation combines robust medical infrastructure with regulatory frameworks supporting clinical translation. This push toward Regenerative Medicine Thailand stems from high regional diabetes prevalence, creating significant demand for specialized care. Local laboratory investments ensure high-quality MSC expansion under strict protocols, providing patients access to viable treatments. Integrating MSC therapy with local innovations, like bio-engineered scaffolds or hydrogels, offers a synergistic approach. As clinical data demonstrates superior outcomes, Thailand is becoming a primary destination for patients seeking a biological reset for previously untreatable chronic conditions.
5.Comprehensive Summary of Advanced Healing Strategies
The journey from a chronic Diabetic ulcer to successful closure requires a shift from passive protection to active biological intervention. While traditional methods like debridement and offloading remain the foundational steps, they cannot overcome the deep-seated cellular exhaustion found in Diabetic tissues. The introduction of UC-MSCs represents a paradigm shift in how we approach Diabetic Wound Healing, providing the necessary signals to dampen inflammation and rebuild the vascular network. By utilizing the strengths of Regenerative Medicine Thailand, healthcare providers can offer a more holistic and effective path to recovery. This approach not only focuses on closing the Wound but also on restoring the functional integrity of the skin and preventing the catastrophic outcome of amputation. As research matures, the synergy between advanced cell biology and clinical expertise in Thailand will likely redefine the standard of care for Diabetic patients worldwide.

