Neuroprotective Mechanisms of UC-MSCs in Advanced Stem Cell Therapy for Parkinson’s Disease
The landscape of neurological healthcare is currently facing a formidable challenge with the rising prevalence of neurodegenerative conditions. Among these, Parkinson’s Disease represents one of the most debilitating diagnoses for the aging population. Characterized by a progressive loss of motor function, this condition stems from the selective destruction of dopaminergic neurons within the substantia nigra pars compacta. Beyond the physical tremors and rigidity, the disease imposes a heavy emotional and economic burden on patients and their families. As the pathology advances, individuals often lose their independence, facing significant cognitive decline and a diminished quality of life that traditional medicine struggles to fully restore.
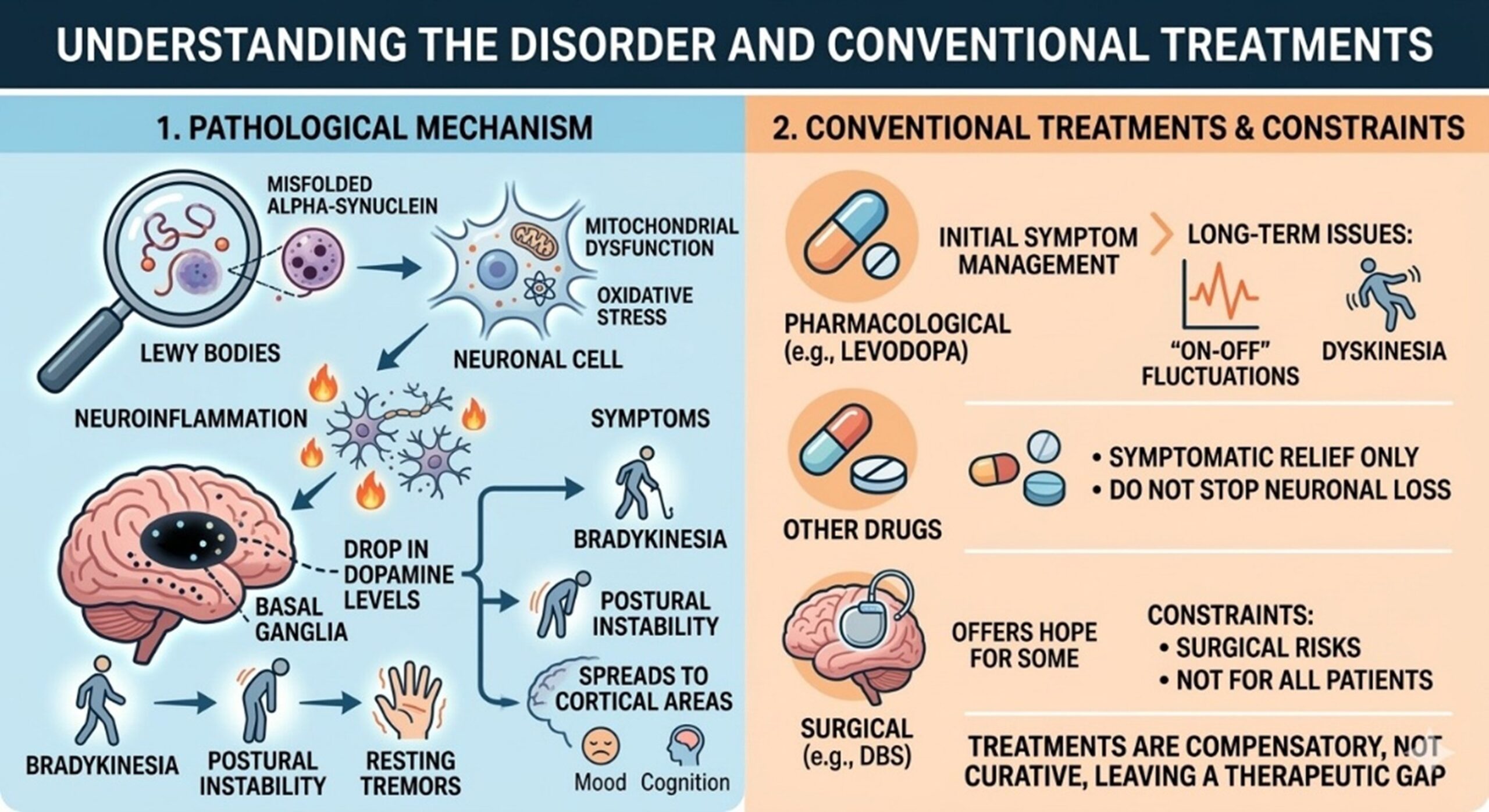
1.Understanding the Pathological Parkinson’s Disease
At its core, the progression of this disorder is driven by the accumulation of misfolded alpha-synuclein proteins, which form toxic aggregates known as Lewy bodies. These aggregates disrupt cellular homeostasis, leading to severe mitochondrial dysfunction and increased oxidative stress. The resulting neuroinflammation creates a hostile microenvironment that accelerates neuronal death. As the dopamine levels drop, the basal ganglia—the brain’s command center for movement—fails to transmit signals effectively. This failure manifests as the classic symptoms of bradykinesia, postural instability, and resting tremors. The systemic impact is profound, as the degeneration is not localized solely to motor pathways but eventually spreads to cortical areas, affecting mood and cognition.
2.Current Conventional Parkinson’s Disease Treatments
For decades, the pharmacological gold standard has been the administration of Levodopa, a precursor to dopamine. While initially effective in managing motor symptoms, long-term reliance on Levodopa often leads to on-off fluctuations and the development of dyskinesia—involuntary, jerky movements that can be as distressing as the disease itself. Other options, such as dopamine agonists or MAO-B inhibitors, provide symptomatic relief but do not address the underlying cause of neuronal loss. Furthermore, invasive procedures like Deep Brain Stimulation (DBS) offer hope for some, yet they carry surgical risks and are not suitable for all patients. These conventional approaches are ultimately compensatory rather than curative, leaving a therapeutic gap that necessitates more innovative strategies.
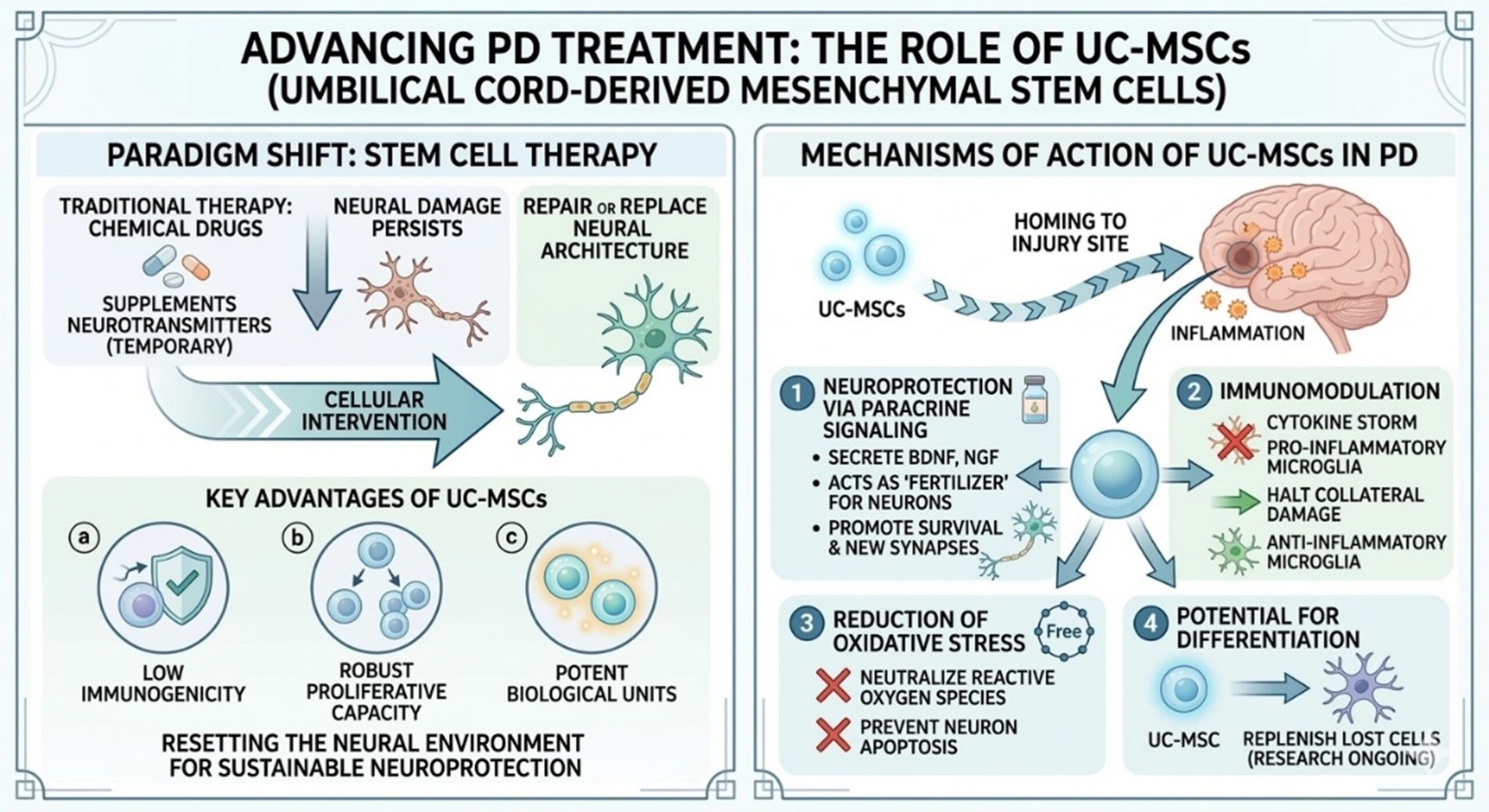
3.The Paradigm Shift to Stem Cell Therapy
This is where Stem Cell Therapy emerges as a transformative alternative. Unlike chemical drugs that merely supplement neurotransmitters, cellular intervention aims to repair or replace the damaged neural architecture. Among the various sources of cells, UC-MSCs (Umbilical Cord-derived Mesenchymal Stem Cells) have gained significant attention. These cells are prized for their low immunogenicity, meaning the body is less likely to reject them, and their robust proliferative capacity. By introducing these potent biological units into the system, clinicians aim to reset the neural environment and provide a sustainable source of neuroprotection that oral medications simply cannot replicate.
4.Detailed Therapeutic Mechanisms of UC-MSCs
The efficacy of UC-MSCs in treating Parkinson’s Disease is rooted in a sophisticated multi-pronged mechanism. First, these cells exhibit a remarkable homing ability, migrating toward areas of injury or inflammation in the brain. Once they reach the site of degeneration, they perform several critical functions:
- Neuroprotection via Paracrine Signaling: The cells secrete a cocktail of neurotrophic
factors, such as Brain-Derived Neurotrophic Factor (BDNF) and Nerve Growth Factor (NGF). These substances act as fertilizer for struggling neurons, promoting survival and stimulating the growth of new synaptic connections.
- Immunomodulation: One of the most vital roles of UC-MSCs is their ability to reduce the
cytokine secretion within the central nervous system. They shift the polarization of microglia from a pro-inflammatory state to an anti-inflammatory state, effectively halting the collateral damage caused by chronic inflammation.
- Reduction of Oxidative Stress: These mesenchymal cells enhance the antioxidant defenses
of the brain, neutralizing reactive oxygen species that would otherwise trigger programmed cell death (apoptosis) in dopaminergic cells.
- Potential for Differentiation: While most benefits are paracrine, research continues to
explore the capacity of these cells to differentiate into neuron-like cells under specific microenvironmental cues, potentially replenishing the lost cellular population over time.
5.The Future of Medical Innovation in Thailand
The outlook for utilizing UC-MSCs within the Thai medical sector is exceptionally bright. Thailand has positioned itself as a global hub for advanced biotechnology, supported by rigorous regulatory frameworks and world-class laboratory facilities. The decision to pursue Stem Cell Therapy in Thailand is driven by the country’s unique combination of medical expertise and a compassionate approach to patient care. Researchers in the region are currently spearheading clinical trials that focus on the long-term safety and efficacy of umbilical cord derivatives, ensuring that the transition from laboratory to bedside is both ethical and scientifically sound. Thailand’s strategic investment in regenerative medicine makes it a primary destination for patients seeking cutting-edge alternatives to conventional neurology.
In summary, the transition from managing symptoms to treating the root biological causes of neurodegeneration represents a pivotal moment in modern medicine. While traditional treatments for Parkinson’s Disease remain useful for early-stage management, their inherent limitations emphasize the need for the regenerative potential offered by Stem Cell Therapy. Through the complex immunomodulatory and neuroprotective actions of UC-MSCs, there is now a tangible path toward not just slowing the disease, but potentially restoring lost function. As Thailand continues to lead the way in this scientific frontier, the hope for a future where neurodegenerative conditions are manageable—or even reversible—becomes increasingly realistic for patients worldwide.

