Chronic ulcerative wounds—such as diabetic foot ulcers, venous leg ulcers, pressure sores, and ulcers caused by poor circulation—pose serious and long-lasting health challenges. These wounds often persist for months despite conventional treatments like wound cleaning (debridement), specialized dressings, antibiotics, and pressure relief techniques. When healing is delayed, patients may experience ongoing pain, infection, reduced mobility, and, in severe cases, the risk of limb amputation. In response to these challenges, regenerative medicine—particularly stem cell therapy—has emerged as a promising solution that focuses on restoring damaged tissue rather than simply managing symptoms.
Umbilical cord–derived mesenchymal stem cells (UC-MSCs) are particularly valuable due to their strong regenerative and anti-inflammatory properties. Their ability to influence multiple aspects of healing makes them an effective tool in treating complex wounds like chronic ulcers.
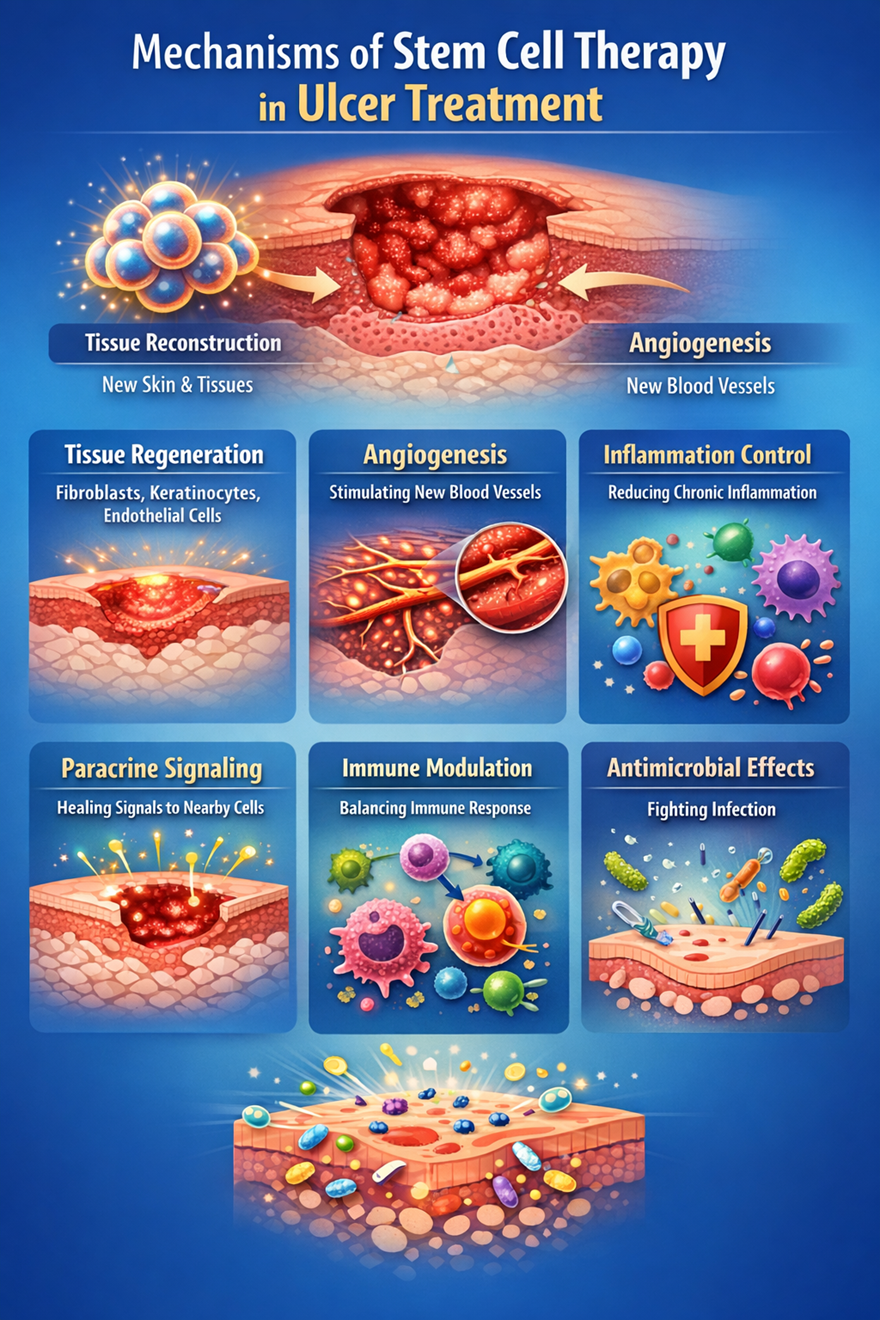
Mechanisms of Stem Cell Therapy in Ulcer Treatment
Stem cell therapy supports wound healing through several interconnected biological processes.
One of the primary mechanisms is tissue reconstruction. Stem cells can differentiate into fibroblasts, keratinocytes, and endothelial cells, which are critical for rebuilding skin, connective tissue, and blood vessels. This allows for repair that extends beyond the surface, restoring deeper layers of damaged tissue.
Another important effect is the promotion of angiogenesis, or the formation of new blood vessels. Chronic ulcers often suffer from poor blood supply, which limits healing. Stem cells release factors such as vascular endothelial growth factor (VEGF), encouraging the development of new capillaries. This improves the delivery of oxygen and nutrients, creating a more favorable environment for tissue repair.
Stem cells also help control inflammation, which is a major barrier to healing in chronic wounds. They produce anti-inflammatory molecules like interleukin-10 (IL-10) and transforming growth factor-beta (TGF-β), which help shift the wound environment from a state of persistent inflammation to one that supports regeneration.
In addition, stem cells play a role in regulating the immune system. They interact with immune cells such as macrophages and T cells, enhancing the body’s ability to fight infection while preventing excessive inflammatory responses that could damage tissue.
Their paracrine activity is another key factor. Even when stem cells do not directly transform into new tissue, they release biochemical signals that encourage nearby cells to multiply, migrate, and participate in healing. This coordinated response accelerates tissue repair and improves overall outcomes.
Some studies also suggest that stem cells may have antimicrobial properties, producing peptides that help inhibit the growth of harmful microorganisms. This can further support wound healing by reducing infection risk.
Benefits of Stem Cell-Based Treatment for Chronic Ulcers
Stem cell therapy offers several advantages over traditional wound care methods. One of the most significant benefits is its ability to promote full-thickness healing, meaning it repairs all layers of the skin rather than just addressing surface damage.
It also tends to result in less scarring, as the regenerated tissue is more organized and similar to normal skin. This can improve both function and appearance.
Faster healing reduces the likelihood of infection and other complications, while the strengthened tissue is more durable and less prone to reopening. For patients with severe ulcers, early use of stem cell therapy may decrease the risk of amputation by preserving affected limbs.
Evidence from Clinical Research
Clinical studies have provided encouraging results regarding the use of stem cells for chronic ulcers. Early-phase trials in patients with diabetic foot ulcers and venous leg ulcers have shown faster wound closure, reduced wound size, and improved tissue quality compared to standard treatments.
Systematic reviews and meta-analyses suggest that a higher proportion of ulcers heal when stem cell therapy is included in treatment plans. Importantly, these studies have not identified major safety concerns when stem cells are used at appropriate doses.
Research on pressure ulcers has also demonstrated improved blood vessel formation and accelerated recovery, further supporting the potential of this therapy.
Future Innovations in Wound Care
The field of regenerative medicine continues to evolve, bringing new possibilities for treating chronic ulcers. Emerging technologies include 3D-printed skin grafts that incorporate stem cells and growth factors, allowing for customized treatment based on the size and shape of the wound.
Smart dressings are also being developed. These advanced materials can respond to changes in the wound environment, such as temperature or pH, and release therapeutic agents accordingly.
Genetically modified stem cells are another area of exploration. These cells may be engineered to produce higher levels of healing factors or to survive better in challenging conditions, such as low oxygen environments.
Exosome therapy is gaining attention as well. By using the bioactive molecules released by stem cells rather than the cells themselves, this approach may offer a safer and more convenient alternative while still delivering regenerative benefits.
Conclusion
Stem cell therapy is an important advancement in the treatment of chronic ulcers. Instead of focusing solely on symptom control, it addresses the underlying causes of impaired healing by promoting tissue regeneration, improving blood flow, reducing inflammation, and supporting immune balance.
As research continues and new technologies are developed, this innovative approach is likely to become an essential component of modern wound care. In Thailand, the growing focus on regenerative medicine positions the country at the forefront of these advancements, offering new hope for patients seeking more effective and lasting solutions to chronic wounds.

