Using UC-MSCs at a stem cell clinic for Tissue Regeneration after Severe bone fractures
Bone fractures are a major worldwide health issue resulting in high levels of disability, even affecting all ages and walks of life. These injuries are a primary result of traumatic events, and also occur due to degenerative processes in the body. Injuries of this severity result in prolonged recovery periods which greatly impact a person’s mobility and function on the job. In certain cases, conventional methods of treatment are suboptimal and result in prolonged recovery times. Therefore, there is a continuing need among medical professionals for innovative approaches to treatment. Recently, one leading stem cell clinic began offering clients an alternative to traditional medicine called regenerative medicine. For a complex injury, the use of UC-MSCs is a novel approach to assist in the gradual process of biological tissue repair. This departure to new, untried and innovative methods fulfills the immediate demand for active treatments.
- Pathophysiology Impact on the Body
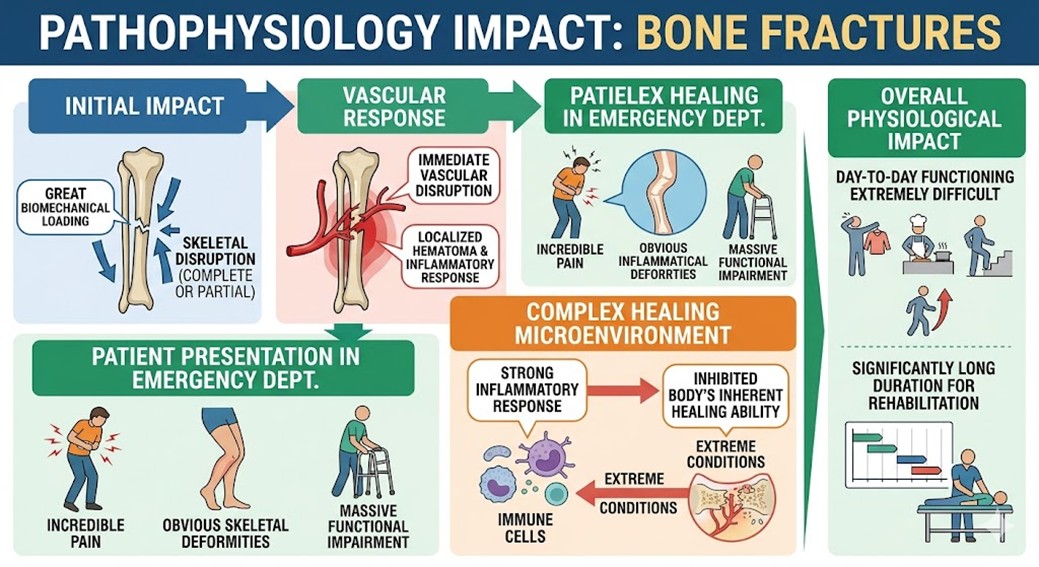
Bone fractures occur as a result of great biomechanical loading applied to the skeletal system resulting in the complete or partial disruption of bone (osseous) tissue. This traumatic event, in turn, causes an immediate and catastrophic disruption of the body’s vascular network in the affected area, creating an inflammatory response and localized hematoma. When patients present to the emergency department, they suffer from an incredible amount of pain and obvious skeletal deformities and a massive impairment of their functional capabilities. In extreme conditions, the body’s inherent ability to heal itself is inhibited due to the complexity of the microenvironment created by the strong inflammatory response. The level of physiological disruption makes the day-to-day functioning of the individual extremely difficult, and it can take a significantly long duration before rehabilitation is completed. The focus of contemporary reparative therapies is on addressing these intricately cellular issues. The inflammatory microenvironment remains a hurdle that a modern stem cell clinic is seeking to optimize via UC-MSCs, to facilitate the osteogenic healing process.
- Present Clinical Limitations and Physical Modalities
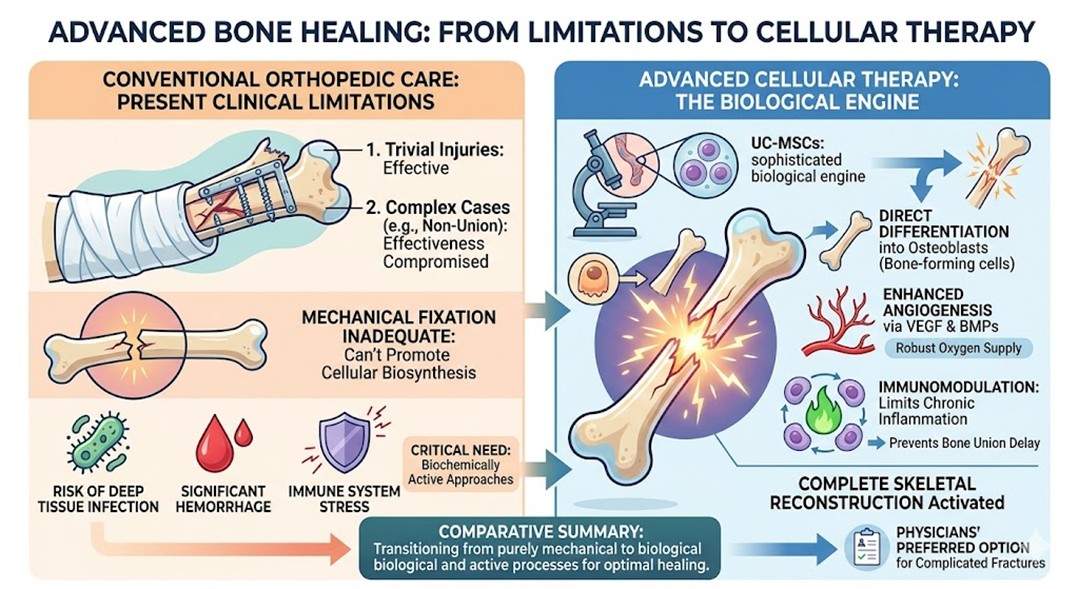
In cases of severe orthopedic trauma, the conventional approach is to combine the mechanical stabilization and anatomical reduction techniques. Post-operative care primarily involves the use of plaster casts, metal plating, or intramedullary nailing to ensure that the affected anatomical structures heal through the process of natural healing. While these strategies are effective for trivial injuries, their effectiveness is considerably compromised for the more complex cases of non-union injuries, which are often encountered. Mechanical fixation, in and of itself, is inadequate to promote the biosynthesis of the requisite cellular constituents, and in addition, the bio-surgical techniques carry the inherent dangers of deep tissue infections, significant hemorrhage, and proto-surgical stress to the immune system. Most, if not all, of these considerations emphasize the critical need for biochemically active approaches. In response to these specific challenges, a particular stem cell clinic has developed a system for assessing adjunct bio-therapies utilizing UC-MSCs. The result of integrating specialized cellular populations is an acceleration of healing processes that would occur in conjunction with the use of traditional immobilization techniques on advanced bone fractures.
- The Biological Engine Behind Advanced Cellular Therapy
UC-MSCs, as utilized in a targeted stem cell clinic, provide a sophisticated biological engine and a critical active process that addresses the full range of deficiencies in traditional fracture management. These amazing cells can differentiate into osteoblasts, or cells that form bones, when they are in the vicinity of the injury. These cells, in addition to direct differentiation, are strong in paracrine signaling. They produce and secrete important bioactive molecules such as bone morphogenetic proteins and vascular endothelial growth factor, both of which are the key to robust angiogenesis, which is critical for the Oxygen supply to the healing bone tissue. Furthermore, UC-MSCs also modulate the local immune response by limiting the milieu of pro-inflammatory cytokines and promoting the polarization of anti-inflammatory macrophages. This form of immunomodulation is what prevents chronic inflammation, which delays the process and pulls the pace of the bone union to a crawl. A state-of-the-art facility uses these mechanisms to activate the process of complete skeletal reconstruction. This dual mechanism is the reason why this modern treatment is becoming the preferred option for physicians for complicated bone fractures.
- Thailand as a Leading Center for Medical Innovation
The clinical pathway for applying regenerative medicine on bone fractures is very promising in the entire Southeast Asia, however, Thailand is the best choice. Thailand is the best option for advanced medical tourism because of the legal and cellular research friendly regulatory framework and high-end healthcare facilities. The country is also home to advanced laboratories and leading medical institutions for accurate cell culture in stem cell research. One leading stem cell clinic in the region has very good UC-MSCs at very competitive prices within the market of Western countries. It is where high-end technology for stem cell therapy is combined with the best holistic care of the patients. Thai medicine will benefit greatly from the upcoming new biological innovations as a result of this integrated approach.

