Chronic ulcer wounds remain one of the most challenging conditions in modern healthcare. Traditional wound management focuses on controlling symptoms and preventing complications. Regenerative medicine has emerged as a promising new direction for treating these difficult wounds. In particular, therapy using umbilical cord–derived mesenchymal stem cells (UC-MSCs) is gaining increasing attention in Thailand as a potential breakthrough in chronic wound care.
Stem cell therapy offers a fundamentally different approach to managing chronic ulcers. Rather than focusing solely on the surface of the wound, regenerative treatments aim to correct the biological conditions that prevent normal healing.
Biological Mechanisms Supporting Wound Repair
Stem cells assist in wound healing through a variety of biological mechanisms that address the complex factors responsible for chronic ulcers.
One of the most important functions of stem cells is their role in tissue regeneration. These cells have the capacity to develop into several types of specialized cells involved in skin repair, including epithelial cells, vascular cells, and connective tissue components. By contributing to the formation of new tissue, stem cells help rebuild damaged structures and restore the integrity of the wound area.
Another critical function involves stimulating blood vessel formation, also known as angiogenesis. Chronic wounds often suffer from inadequate blood circulation, which limits oxygen delivery and nutrient supply. Stem cells release signaling molecules such as vascular endothelial growth factor (VEGF), which encourage the formation of new capillaries within the damaged tissue. Improved circulation supports the survival of surrounding cells and promotes long-term healing.
Stem cells also play an important role in controlling inflammation. Many chronic ulcers remain trapped in a prolonged inflammatory phase that interferes with normal tissue repair. Mesenchymal stem cells produce anti-inflammatory cytokines that help calm excessive immune responses. By reducing inflammation, the wound environment can shift toward the regenerative phase of healing.
Another beneficial mechanism involves immune system regulation. Stem cells interact with immune cells such as macrophages, encouraging them to transition from a destructive inflammatory state into a regenerative form that supports tissue rebuilding. This shift helps limit further damage to surrounding tissues while promoting recovery.
In addition to direct cell replacement, stem cells exert powerful paracrine effects. This means they release signaling molecules, growth factors, and extracellular vesicles that influence nearby cells. These signals stimulate the activity of fibroblasts, keratinocytes, and other skin cells responsible for producing collagen, migrating across the wound surface, and closing the injury. Even when stem cells do not directly become new tissue, their signaling functions can activate the body’s natural repair processes.
Researchers have also observed antimicrobial properties associated with stem cells. Certain peptides released by these cells may inhibit the growth of harmful bacteria, which helps reduce infection risk and maintain a healthier wound environment.
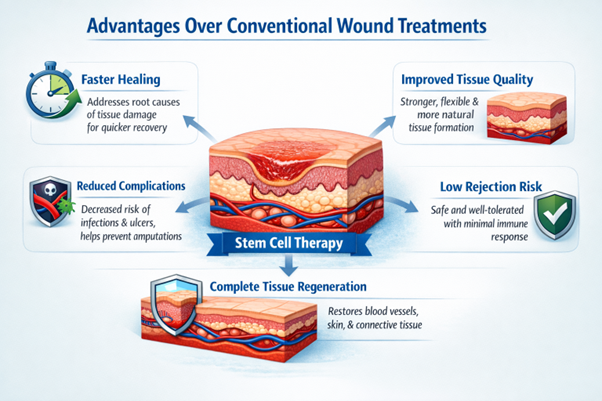
Advantages Over Conventional Wound Treatments
Stem cell therapy provides several potential advantages compared with traditional wound care methods. One of the most notable benefits is the ability to promote faster healing by addressing the root causes of tissue damage rather than simply managing surface symptoms.
The regenerated tissue formed during stem cell–assisted healing often demonstrates improved strength and flexibility compared with scar tissue produced during conventional healing. Because stem cells stimulate the repair of skin, connective tissue, and blood vessels simultaneously, the resulting tissue may more closely resemble normal skin.
Another important advantage involves the reduction of serious complications. By improving blood circulation, regulating inflammation, and supporting immune defenses, stem cell therapy may help prevent ulcer progression and decrease the likelihood of infections that could lead to amputation.
Safety is also a key consideration. Clinical studies and therapeutic experiences worldwide suggest that mesenchymal stem cell treatments are generally well tolerated by patients. Because these cells possess immune-modulating properties, the risk of rejection is relatively low. In most cases, stem cell therapy is applied locally to the wound area, minimizing systemic effects.
Most importantly, regenerative therapy aims to achieve complete tissue restoration, rather than temporary closure of the wound surface. By rebuilding deeper structures such as blood vessels and connective tissue, stem cell therapy seeks to provide a more durable and stable healing outcome.
Thailand’s Role in Regenerative Wound Care
Thailand has become an emerging center for regenerative medicine in Southeast Asia. The country’s healthcare system combines advanced medical infrastructure with experienced clinicians and supportive regulatory oversight. This environment has enabled significant progress in the development and application of stem cell–based therapies.
Several hospitals and research institutions across Thailand are actively studying the use of stem cells for treating diabetic ulcers and other chronic wounds. Laboratories that produce therapeutic stem cells often follow Good Manufacturing Practice (GMP) standards to ensure strict quality control, sterility, and safety throughout the preparation process.
These developments have made Thailand an increasingly recognized destination for patients seeking innovative regenerative treatments. As clinical experience grows and research continues to expand, the use of stem cell therapy in wound care is expected to play an increasingly important role in the country’s medical landscape.
Conclusion
Chronic ulcer wounds remain a major medical challenge, particularly among aging populations and individuals with diabetes or circulatory disorders. Traditional treatments are valuable for managing symptoms and preventing complications, but they often fail to resolve the underlying biological conditions that prevent healing.
Stem cell therapy offers a new regenerative strategy that targets the root causes of chronic wounds. By promoting blood vessel growth, regulating inflammation, stimulating tissue regeneration, and supporting immune balance, mesenchymal stem cells create a more favorable environment for long-term recovery.
In Thailand, the growing use of stem cell therapy reflects the expanding role of regenerative medicine in modern healthcare. As scientific research continues and clinical applications evolve, stem cell–based treatments may provide a powerful pathway toward lasting wound healing and improved quality of life for patients suffering from chronic ulcers.

