Strategic Breakthroughs in Managing Diabetes Mellitus with UC-MSCs stem cell therapy in Thailand
The global healthcare landscape is currently facing a monumental challenge in the form of Diabetes Mellitus, a chronic metabolic disorder characterized by persistent hyperglycemia. For decades, this condition has been viewed as a progressive burden, leading to severe systemic complications such as neuropathy, retinopathy, and end-stage renal disease. The sheer scale of the epidemic has forced medical researchers to look beyond conventional symptom management. Patients often find themselves trapped in a cycle of constant glucose monitoring and exogenous insulin dependence, which, while life-saving, does not address the underlying cellular dysfunction. Consequently, there is a pressing need for regenerative interventions. This is where stem cell therapy offers a transformative path forward. Specifically, the utilization of UC-MSCs (Umbilical Cord-derived Mesenchymal Stem Cells) has emerged as a frontline candidate for restoring metabolic balance, aiming to transition from temporary management to genuine biological repair.
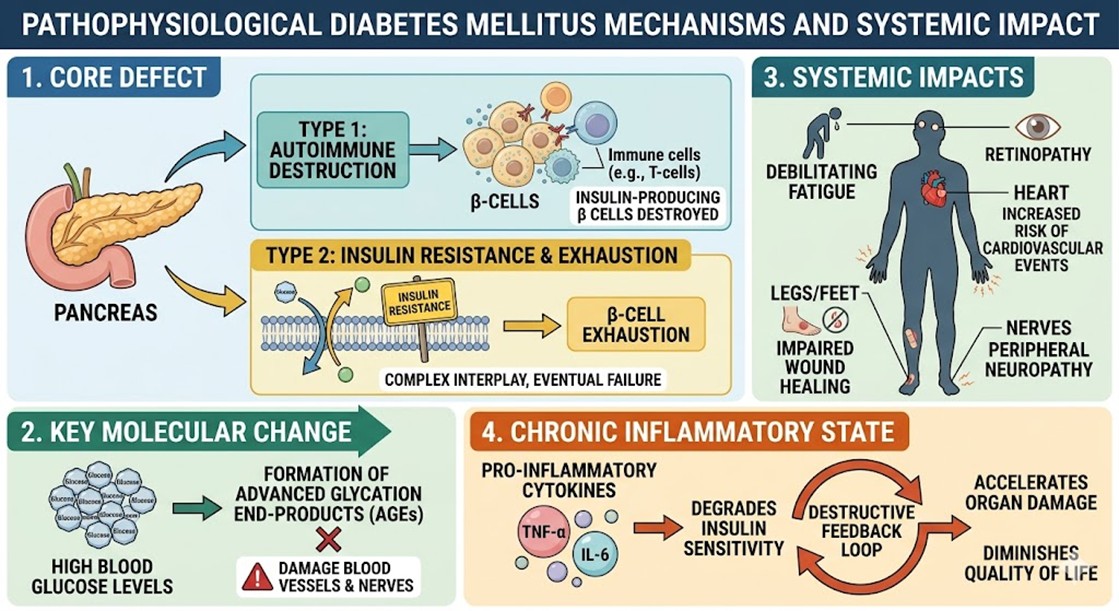
- Pathophysiological Diabetes Mellitus Mechanisms and Systemic Impact
At its core, Diabetes Mellitus represents a profound failure of the body’s glucose regulatory system. In Type 1 cases, an autoimmune assault destroys insulin-producing β cells in the pancreas, whereas Type 2 involves a complex interplay of insulin resistance and eventual β-cell exhaustion. The resulting high blood glucose levels trigger the formation of advanced glycation end-products, which damage blood vessels and nerves over time.
Patients suffer from debilitating fatigue, impaired wound healing, and a significantly increased risk of cardiovascular events. The cellular environment becomes increasingly pro-inflammatory, characterized by an overabundance of cytokines like TNF-α and IL-6. This chronic inflammatory state further degrades insulin sensitivity, creating a destructive feedback loop that accelerates organ damage and diminishes the quality of life for millions.
- Limitations of Conventional Therapeutic Diabetes Mellitus Approaches
Standard medical protocols for managing blood sugar levels primarily rely on lifestyle modifications, oral hypoglycemic agents, and various insulin analogs. While these Diabetes Mellitus treatments are effective at preventing immediate ketoacidosis or severe hyperglycemic spikes, they possess inherent limitations. They are reactive rather than proactive, focusing on the symptoms of insulin deficiency rather than the regeneration of the pancreatic microenvironment. Furthermore, long-term use of certain medications can lead to weight gain, gastrointestinal distress, or the dreaded risk of hypoglycemia. Many patients eventually reach a plateau where pharmacological intervention no longer prevents the progression of secondary complications, highlighting the therapeutic ceiling of modern traditional medicine.
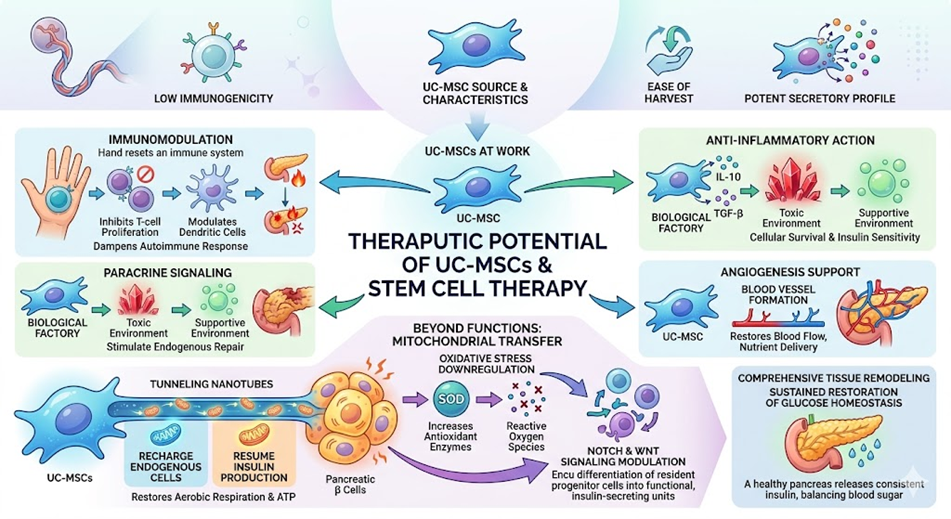
3.Therapeutic Potential of UC-MSCs and Stem Cell Therapy
The shift toward stem cell therapy represents a paradigm change in endocrinology. Among various cell types, UC-MSCs are preferred due to their low immunogenicity, ease of harvest, and potent secretory profile. These cells function through several sophisticated biological pathways.
- Immunomodulation These cells can reset the immune system by inhibiting the proliferation of T-cells and modulating the activity of dendritic cells, effectively dampening the autoimmune response that targets the pancreas.
- Paracrine Signaling Rather than just replacing cells, they act as biological factories, releasing growth factors and exosomes that stimulate the repair of endogenous pancreatic tissue.
- Anti-Inflammatory Action By secreting IL-10 and TGF-β, they transform the toxic, high-glucose environment into one that supports cellular survival and insulin sensitivity.
- Angiogenesis Support They promote the formation of new blood vessels, which is critical for restoring blood flow to damaged tissues and improving the delivery of nutrients.
Beyond these functions, the efficacy of stem cell therapy involves mitochondrial transfer. UC-MSCs possess the unique ability to donate healthy mitochondria to stressed or dying pancreatic β cells via tunneling nanotubes. This direct energy transfer restores aerobic respiration and cellular ATP levels, effectively recharging the endogenous cells to resume natural insulin production. Furthermore, these cells actively downregulate oxidative stress by increasing the expression of antioxidant enzymes like superoxide dismutase. This reduces the accumulation of reactive oxygen species that typically exacerbate insulin resistance. By modulating the Notch and Wnt signaling pathways, these cells also encourage the differentiation of resident progenitor cells into functional, insulin-secreting units. This dual action of protecting existing cells while fostering the birth of new ones creates a robust regenerative environment. Such deep biological integration ensures that the therapeutic impact is not merely transient but contributes to a sustained restoration of glucose homeostasis through comprehensive tissue remodeling.
- The Future of Regenerative Medicine in Thailand
Thailand has positioned itself as a premier destination for advanced clinical applications involving UC-MSCs. The country’s medical infrastructure combines rigorous international standards with a specialized focus on regenerative biology. Patients are increasingly looking toward Thailand because of its concentration of world-class research facilities and experienced clinicians who specialize in metabolic health. The future outlook involves integrating genomic screening with cellular infusions to provide highly personalized protocols. By fostering an environment where biotechnology and clinical care overlap seamlessly, Thailand serves as a hub for those seeking cutting-edge alternatives to daily injections. The regulatory framework in the region is also evolving to support the safe and ethical application of cellular products, making it a stable and attractive location for long-term health journeys.
In summary, the transition from traditional maintenance to the regenerative capabilities of stem cell therapy marks a new era for individuals living with Diabetes Mellitus. By leveraging the unique immunomodulatory and reparative properties of UC-MSCs, it is possible to target the inflammatory roots of the disease. While conventional methods remain necessary for immediate control, the biological potential offered by cord-derived cells provides a beacon of hope for sustained health. As Thailand continues to lead the way in clinical excellence and specialized research, the dream of achieving metabolic homeostasis through cellular restoration becomes increasingly attainable for a global population.

