Chronic ulcerative wounds remain one of the most difficult conditions to manage in modern healthcare. These include diabetic foot ulcers, venous leg ulcers, pressure sores, and wounds caused by poor blood circulation. Conventional approaches are primarily designed to manage symptoms rather than fully restore damaged tissue. As a result, patients may experience ongoing pain, infection, limited mobility, and in severe cases, the risk of limb amputation.
In recent years, regenerative medicine has introduced a new and promising direction for treating chronic ulcers. Among the most advanced approaches is umbilical cord–derived mesenchymal stem cell (UC-MSC) therapy. This innovative treatment focuses on repairing and regenerating damaged tissue at a biological level, offering hope for more complete and lasting healing.
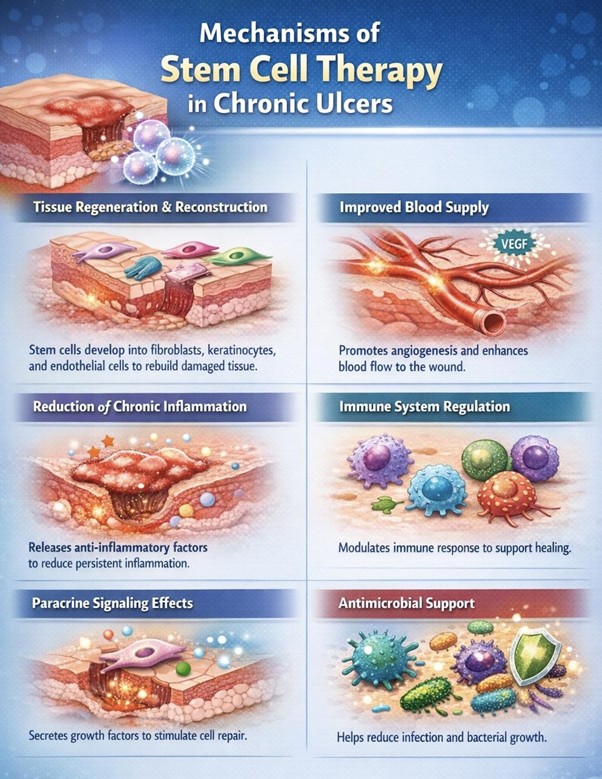
Mechanisms of Stem Cell Therapy in Chronic Ulcers
- Tissue Regeneration and Reconstruction: Mesenchymal stem cells can develop into key structural cells needed for wound repair. These include fibroblasts, which produce connective tissue; keratinocytes, which form the outer skin layer; and endothelial cells, which create blood vessels. By contributing to the formation of these cell types, stem cells help rebuild damaged tissue from the inside out.
- Improved Blood Supply: One of the major challenges in chronic wounds is poor circulation. Stem cells release growth factors such as vascular endothelial growth factor (VEGF), which stimulate the formation of new blood vessels—a process known as angiogenesis. Improved blood flow enhances oxygen and nutrient delivery, both of which are essential for healing.
- Reduction of Chronic Inflammation: Persistent inflammation is a key factor that prevents chronic wounds from healing. UC-MSC stem cells produce anti-inflammatory molecules that help shift the wound environment from a state of ongoing damage to one that supports repair. This transition is critical for allowing tissue regeneration to occur.
- Immune System Regulation: Stem cells interact with immune cells, including macrophages and T cells, to create a balanced immune response. This helps the body fight infection more effectively while avoiding excessive inflammation that could further damage tissue.
- Paracrine Signaling Effects: A significant portion of stem cell activity comes from the release of signaling molecules. These factors encourage nearby cells to multiply, migrate, and participate in tissue repair. Even when stem cells do not directly become new tissue, they play a vital role in orchestrating the healing process.
- Antimicrobial Support: Emerging research suggests that mesenchymal stem cells may produce antimicrobial peptides. These substances can help limit bacterial growth within the wound, reducing the risk of infection and supporting faster recovery.
Methods of Delivering Stem Cell Therapy for Chronic Ulcers
- Topical Application: Stem cells are incorporated into gels or dressings that are applied directly to the wound This method is suitable for shallow or easily accessible ulcers.
- Localized Injection: Stem cells are injected into and around the wound site, allowing them to act in deeper layers of tissue. This approach is often used for diabetic foot ulcers and pressure sores.
- Biomaterial Scaffolds: Stem cells are combined with supportive materials such as collagen or fibrin to create a structured environment for tissue growth. These scaffolds protect the cells and guide organized healing.
- Intravenous Infusion: In some cases, stem cells are delivered through the bloodstream. They can travel to damaged areas and contribute to repair, particularly when multiple wounds are present.
Benefits of Stem Cell Therapy for Chronic Ulcers
Regenerative treatment using stem cells offers several advantages over traditional wound care methods. One of the most significant benefits is its ability to promote full-thickness healing. Instead of addressing only the surface, stem cell therapy works to rebuild all layers of the skin and underlying structures.
Another advantage is the reduction of scarring. By guiding tissue regeneration in a more organized manner, stem cells help minimize fibrosis and improve the final appearance of healed skin. Faster wound closure also lowers the risk of infection and other complications.
Additionally, the newly formed tissue tends to be stronger and more resilient, reducing the likelihood of the wound reopening. In severe cases, early use of stem cell therapy may decrease the need for amputation by preserving tissue and restoring function.
Clinical Evidence and Research Progress
Clinical studies on stem cell therapy for chronic ulcers have shown encouraging results. Patients with diabetic foot ulcers and venous leg ulcers have demonstrated faster healing rates, reduced wound size, and improved tissue quality.
Stem cell treatments may lead to better healing outcomes compared to standard care alone, without significant safety concerns when used appropriately. Research on pressure ulcers has also shown improved blood vessel formation and accelerated recovery. The existing evidence supports the growing role of stem cell therapy in wound management.
Conclusion
Stem cell therapy marks a significant breakthrough in managing chronic ulcers. By addressing the underlying causes of impaired healing—such as poor circulation, inflammation, and cellular dysfunction—this approach goes beyond symptom management to achieve true tissue regeneration.
As research continues and new technologies emerge, stem cell therapy is expected to play an increasingly important role in wound care. In Thailand, where regenerative medicine is rapidly advancing, this innovative treatment offers new hope for patients facing the challenges of chronic ulcers. With its potential to accelerate healing, reduce complications, and preserve limbs, stem cell therapy is shaping the future of modern wound management.

