Experts In this age of revolution in medicine, there is a significant shift taking place in the neurological landscape from symptomatic management to biological restoration. Parkinson’s disease is one of the most challenging neurodegenerative disorders of our time in this context. It is characterized by the loss of dopaminergic neurons in the substantia nigra pars compacta. The loss of these cells triggers a catastrophic chain reaction of motor deficits, such as tremor, stiffness and balance problems.
Then, of course, there is the emotional aspect of Parkinson’s Disease. The disease weighs extremely heavy on mental health and cognitive function, ultimately taking away autonomy. With an ageing global population, the socioeconomic burden of this condition increases and requires a shift in strategy from temporary reliefs to such permanent cellular and Regenerative Medicine interventions.
1.Understanding the Pathophysiology of Neuronal Decay
The root of many cases of Parkinson’s Disease involves the abnormal misfolding of alpha-synuclein proteins that will bunch together to form harmful bundles called Lewy bodies. This aberrant assembly modifies cellular balance and gives rise to mitochondrial dysfunction and oxidative stress. When dopaminergic neurons die, the fine control of basal ganglia is lost and classical motor symptoms occur.
The amount of neuronal loss determines the severity of the disease, only to become clinically overt once approximately 60-80% loss has occurred. That late stage diagnosis means that by the time a patient comes to a clinician, their brain is already had massive structural changes and has also made traditional pharmaceutical interventions increasingly less effective.
2.Current Standard of Care and Limitations
Current pharmacological Parkinson’s Disease approaches primarily rely on Levodopa or dopamine agonists to replenish the brain’s dwindling dopamine levels. While these treatments offer a honeymoon period of symptom relief, they do not halt the underlying neurodegeneration. Over years of use, many patients develop motor fluctuations and dyskinesia—involuntary, jerky movements caused by the medication itself.
Furthermore, deep brain stimulation, while effective for certain motor symptoms, involves invasive surgery and does not address the non-motor aspects of the disease like depression or cognitive decline. These limitations highlight a desperate need for Regenerative Medicine strategies that can actually replace the lost hardware of the brain rather than just tweaking the software.
3.The Role of Regenerative UC-MSCs Medicine in Therapeutic Innovation
Umbilical cord-derived mesenchymal stem cells, or UC-MSCs, have emerged as a frontrunner in the field of Stem Cell therapy as Regenerative Medicine due to their unique immunomodulatory and neuroprotective properties. Unlike traditional treatments, UC-MSCs function through several complex biological pathways. First, they secrete growth factors and cytokines, such as brain-derived neurotrophic factor, which support the survival of existing neurons. Second, their immunomodulatory capacity allows them to dampen the chronic neuroinflammation that accelerates cell death in Parkinson’s Disease.
The mechanism of action is multifaceted. These cells migrate to the sites of injury—a process called homing—where they release extracellular vesicles containing microRNAs that can reprogram the local microenvironment. This shift from a pro-inflammatory state to a pro-healing state is crucial. By reducing the activation of microglia and astrocytes, UC-MSCs create a bio-shield that protects surviving dopaminergic cells from further oxidative damage. This dual action of protection and potential replacement is why researchers believe that Stem Cell integration is the only way to achieve long-term remission.
4.Future Prospects for Cellular Therapy in Thailand
The trajectory of Regenerative Medicine in Thailand is exceptionally promising, positioned at the intersection of advanced biotechnology and specialized medical tourism. Thailand has established itself as a regional hub for cellular research, backed by a regulatory framework that encourages clinical innovation while maintaining high safety standards. The country’s medical infrastructure provides a unique advantage for international patients seeking cutting-edge treatments that might be bogged down by bureaucracy elsewhere.
Why Thailand? Beyond the world-class hospital facilities, the nation has invested heavily in laboratory excellence and specialized training for neurologists and cellular biologists. The future involves moving toward personalized protocols where MSCs are tailored to the specific genetic profile of the patient. This evolution will likely see Thailand leading the way in integrating Stem Cell Regenerative Medicine protocols into routine clinical practice for neurodegenerative disorders likes Parkinson’s Disease, offering a blend of high-tech intervention and compassionate care that is difficult to replicate in other regions.
5.Advanced Clinical Integration and Safety Standards
As Thailand solidifies its position, the focus has shifted toward the standardization of UC-MSC Regenerative Medicine protocols. This involves rigorous screening of donor tissue and advanced expansion techniques in Grade A cleanrooms. For patients with Parkinson’s Disease, this ensures that the biological material is of the highest potency and free from contaminants. The integration of Regenerative Medicine into the broader healthcare system in Thailand is also supported by a growing body of local clinical data, which helps refine dosage and delivery methods for optimal neuronal support.
Furthermore, the collaboration between Thai research institutes and international biotechnology firms has accelerated the development of targeted delivery systems. These systems aim to enhance the homing capabilities of UC-MSCs, ensuring that a higher concentration of secretomes reaches the affected areas of the brain. This precision-based approach is a hallmark of the medical excellence found in Thailand today.
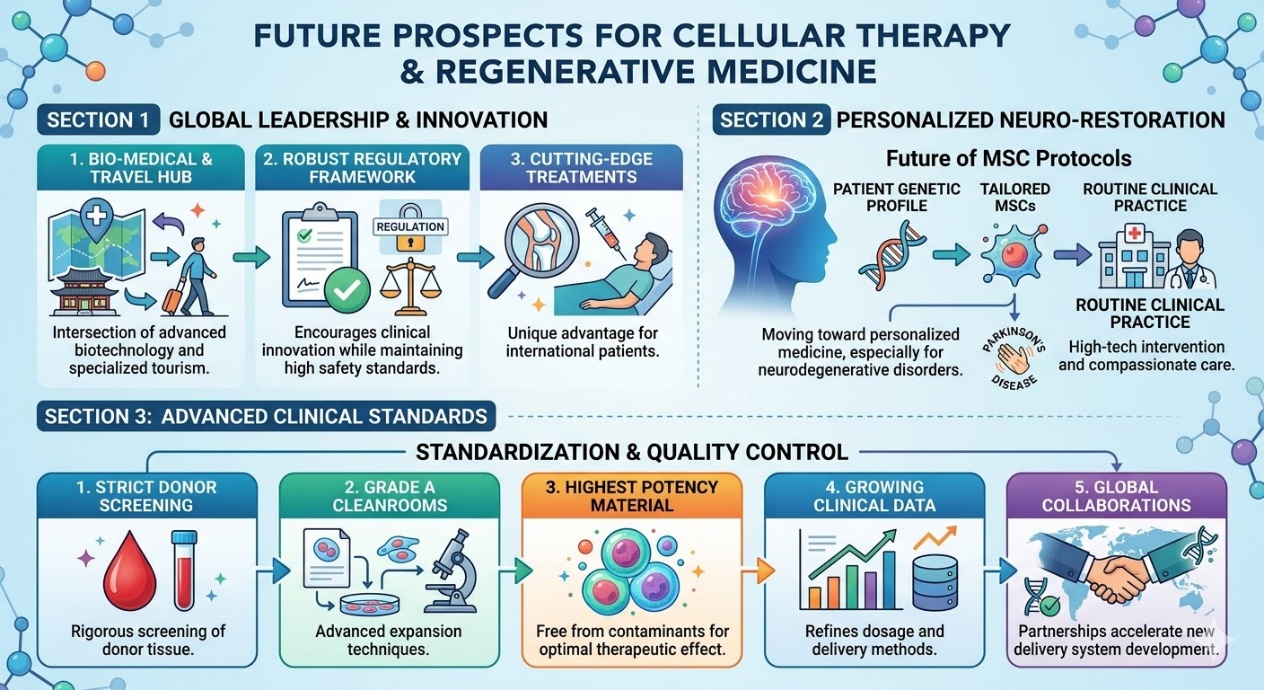
Figure 1: Future Prospects for Parkinson’s Disease Cellular Therapy and Regenerative Medicine
in Thailand
To conclude, the shift from palliative care to restorative therapy is the most important step in managing Parkinson’s Disease. Conventional medications can restore relieve symptoms but could never rectify the underlying process of neuronal death. With Regenerative Medicine in mind, a future where UC-MSCs are expanding the arsenal to fight neurodegeneration by modulating inflammation, releasing essential growth factors, and protecting structural integrity of brain can now be envisioned. With the advance of research, Thailand stay in the front of this medical uprising giving a sign of hope for those searching to reclaim their living again on improvement into this sickness. Stem Cell Science is poised to become an inevitable part of the clinical landscape, one welcomed as a development in science, far more importantly that such presence will be essential for health at the global level.