The liver is one of the hardest-working organs in our human system, but it usually remains silent until much doom occurs. Early Liver Disease → The majority of those afflicted with early symptoms may only experience mild tiredness, lessened appetite, and abdominal discomfort, or none at all. When things like swelling, jaundice, easy bruising, fluid retention, or confusion appear, the disease could be more advanced already.
This is one of the reasons patients are starting to look for a stem cell clinic that views liver health from a broad biological window. They are seeking more than just medication or symptom control. There are those who want a more holistic approach to stem cell healthcare, looking at inflammation, fibrosis, immune imbalance, and liver repair signaling through nutrition-mediated metabolic health long-term monitoring.
Still, this topic needs honesty. Stem Cell therapy for Liver Disease is not a cure-out-of-the-box and thus should not be presented as an alternative to current hepatology care, antiviral treatment strategies, lifestyle modification, including nutritional correction, or liver transplant evaluation and standard medical management. From a mechanistic point of view, recent studies are encouraging, particularly on mesenchymal stem/stromal cells (MSCs), but also in this case, the clinical application needs to be cautiously interpreted and safely monitored with realistic expectations.
The Liver Does More Than Most People Realize
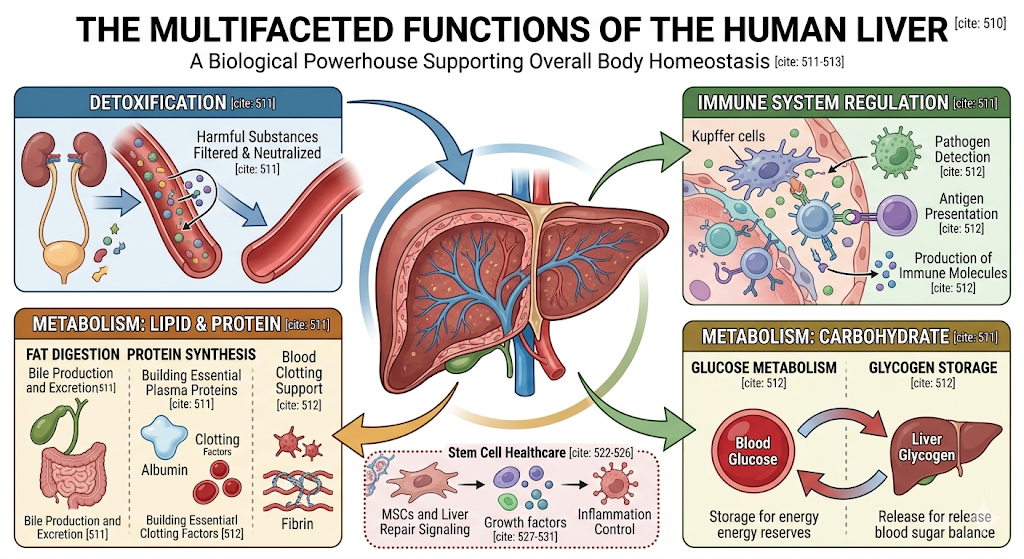
It has many functions, including detoxification, bile production and excretion; metabolism of fat digestion, protein synthesis; support for blood clotting, regulation from the immune system, glycogen storage, and glucose metabolism. The whole body notices when your liver is inflamed or scarred.
Chronic liver disease can be attributed to a number of different causes, such as alcohol-associated liver disease, chronic hepatitis B or C virus-related injury, nonalcoholic fatty liver disease associated with metabolic dysfunction (formerly known as non-alcoholic fatty pancreas), autoimmune hepatic diseases, drug-induced, and long-term toxic injury related to metabolopathies/genetic conditions. Major causes of cirrhosis include alcohol-associated liver disease, nonalcoholic fatty liver disease, chronic hepatitis C, and chronic hepatitis B, according to the U.S. NIDDK.
Why Liver Disease Can Progress Quietly
The most painful part of Liver Disease is that the liver stays compensated for a long time. A patient may be doing well, working, and only experiencing fatigue, while in the background, inflammation and fibrosis continue.
Cirrhosis is the progressive scarring and warping of liver tissue as a consequence of prolonged hepatic insult. Cirrhosis in advanced states may lead to liver failure, and some patients eventually need a liver transplantation.
This is why early assessment of matters. As a responsible stem cell clinic, we will never start any treatment without first being able to clarify the stage of liver disease (if applicable), what caused it, and its severity.
Where Stem Cell Healthcare Enters the Conversation
The phrase stem cell healthcare should not mean selling cell therapy as a shortcut. A more responsible meaning is an integrated medical model that looks at the liver’s biological environment and asks: what factors are still modifiable?
For Liver Disease, this may include inflammation, oxidative stress, immune activity, fibrosis signaling, nutritional depletion, metabolic dysfunction, alcohol exposure, viral control, and overall physical condition. In this wider context, a stem cell clinic may discuss regenerative medicine as one possible supportive area, but not as a standalone solution.
The Main Scientific Interest: MSCs and Liver Repair Signaling
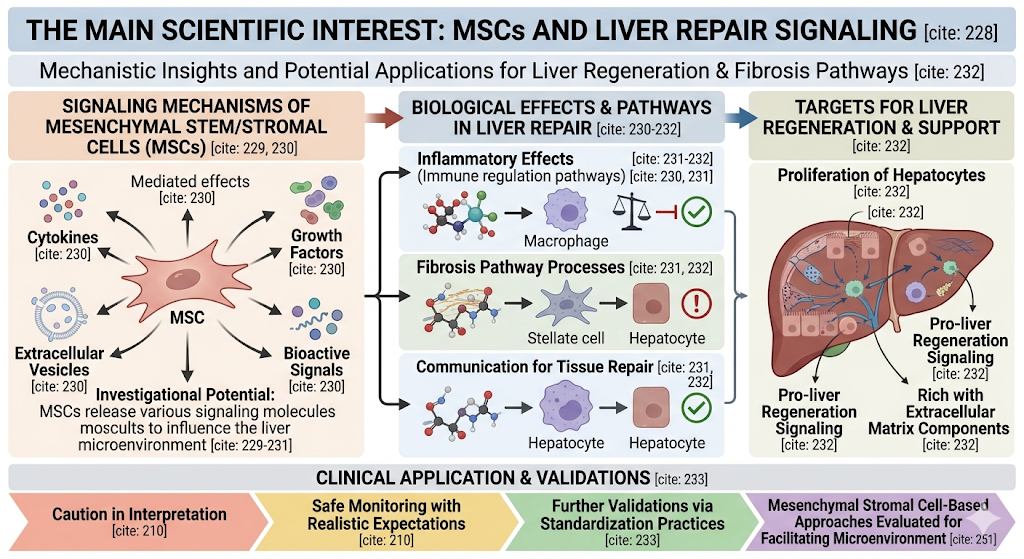
Research relative to stem cells and liver diseases has undoubtedly highlighted your focus on mesenchymal stem/stromal cells, often referred to as MSCs. These cells are under research due to their potential in releasing cytokines, growth factors, extracellular vesicles, and other bioactive signals mediating inflammatory effects; immune regulation pathways; fibrosis pathway processes and communication for tissue repair.
Reviewing MSC therapy for end-stage liver disease in 2025 concluded that potential mechanisms included immunomodulation, anti-fibrotic properties, and pro-liver regeneration signaling, both supporting the proliferation of hepatocytes as well as providing a niche rich with extracellular matrix components; nevertheless, clinical translation requires further validations via standardization practices.
What a Stem Cell Clinic Should Assess Before Liver Support
A serious stem cell clinic should treat Liver Disease as a medical condition first, not a marketing category. The evaluation should be careful and individualized.
Identify the Type of Liver Disease
Fatty liver disease, viral hepatitis, autoimmune hepatitis, alcohol-associated liver injury, cholestatic liver disease, and cirrhosis do not behave the same way. The treatment plan must depend on the cause.
Understand the Stage
A patient with early fatty liver has different needs from someone with decompensated cirrhosis, ascites, varices, jaundice, or hepatic encephalopathy. Advanced cases need hepatology supervision and sometimes transplant evaluation.
Review Liver Function and Risk
Blood tests such as ALT, AST, bilirubin, albumin, INR, platelet count, kidney function, viral markers, and fibrosis assessment may be important. Imaging, FibroScan, ultrasound, CT, MRI, or specialist review may also be needed.
Build a Wider Stem Cell Healthcare Plan
The best stem cell healthcare program should also address nutrition, protein intake, metabolic health, alcohol avoidance, viral control, weight management, sleep, inflammation, and follow-up monitoring.
Stem Cell Clinic for Liver Disease: What Should Be Said Carefully
All a stem cell clinic that addresses Liver Disease should not claim dramatic statements like “reverse cirrhosis”, or similar, such as regrow the liver or guarantee to avoid transplant. The assertions are overblown and misleading for patients.
A more scientifically cautious explanation is that MSC-based approaches are being evaluated for their potency to facilitate the liver microenvironment. Although some trials indicate liver function marker improvements, immune modulation, and fibrosis-related pathways with diverse results across different protocols, these results are not yet fully standardized.
A 2025 meta-analysis of MSC therapy in acute-on-chronic liver failure found improvements in MELD score and albumin as measures of liver function, although with no increase in AEs or SAEs across the studies analyzed—but this does not imply all patients with impaired livers are candidates, and better still, that outcomes for everybody would be favorable.
Why Safety Matters in Stem Cell Healthcare
The liver is one of our strongest organs, which is connected with immunity, metabolism, and the detoxification process. These patients with decompensated Liver Disease also have a bleeding tendency, infection risk, low albumin levels, and kidney stress in the form of higher creatinine, portal hypertension, or fluid buildup. These reasons make safety screening necessary.
According to the U.S. FDA, some stem cell and exosome products claiming regenerative properties are marketed with false claims about their safety or science, such that prospective patients may be misled. The FDA also said that in the U.S., only blood-forming stem cells from umbilical cord blood for diseases of cell formation are grandfathered, not general regenerative uses being touted as available today in clinics.
This is not an excuse to throw research out the window. This is a reason to select a stem cell clinic that uses clear language, adheres to medical standards, and is not hyperbolic.
A Better Model for Liver Regenerative Support
A strong stem cell healthcare program for Liver Disease should feel structured, not rushed. It may include:
Medical Diagnosis First
Before any regenerative discussion, the clinic should understand the liver diagnosis and whether the patient is stable enough for supportive care.
Hepatology Collaboration
For advanced liver disease, care should involve a liver specialist. A stem cell clinic should not work against standard medical care.
Cell Quality Transparency
If cell-based therapy is discussed, the clinic should explain cell source, testing, sterility, viability, release criteria, physician supervision, and follow-up plan.
Measurable Follow-Up
Progress should be monitored through symptoms, liver function tests, imaging context, inflammation markers, nutrition status, and quality-of-life tracking.
Lifestyle and Metabolic Correction
No stem cell healthcare program can replace the basics. Alcohol avoidance, viral treatment when indicated, weight control, blood sugar management, adequate protein, and medical monitoring are still central.
Conclusion
Ideally, a clinic that focuses on stem cells in the modern era should methodically study Liver Disease both scientifically and clinically. The liver is one of the only organs that, even in certain contexts, can regenerate, so to some degree, chronic inflammation/fibrosis/cirrhosis are very serious and need traditional diagnosis / longer-term medical care.
Integrating immune modulation, anti-inflammatory signaling pathways, fibrosis-related and liver repair communication together with MSCs research: an area of stem cell exploration. This is encouraging for the area, but not straightforward.
Writing here about stem cell healthcare most particularly focuses not upon miracle claims as the model of responsibility. We construct it on principles of careful assessment, laboratory quality, and adherence to safety monitoring, collaboration with hepatology specialists by utilizing meals in the context of nutrition/ lifestyle modification through safe, practical targets.
It is time for the best path, which that noisy promise from Liver Disease would not often give me at all. So, it is to turn toward a medical team most deeply versed in the liver—and who can explain what stem cells may help with, and not be painted as having any guarantees—while offering, along with the question of why 100% foundational care for the state of ones introoster makes good sense.
FAQ: Stem Cell Clinic and Liver Disease
1. Can a stem cell clinic cure Liver Disease?
No. A responsible stem cell clinic should not claim to cure Liver Disease. Stem cell-based approaches are being studied for liver support, inflammation balance, and repair signaling, but they should not be promoted as guaranteed cures.
2. What is stem cell healthcare for liver support?
Stem cell healthcare refers to a broader care model that may combine medical assessment, regenerative science, nutrition, lifestyle correction, inflammation control, laboratory safety, and follow-up monitoring.
3. Are stem cells being studied for cirrhosis?
Yes. MSCs are being studied for liver fibrosis, cirrhosis, acute-on-chronic liver failure, and other liver-related conditions. However, research is still developing, and treatment should be considered carefully.
4. Who may not be suitable for liver stem cell support?
Patients with severe decompensated cirrhosis, active infection, uncontrolled bleeding risk, liver cancer, severe kidney failure, or unstable medical status may need specialist management first.
5. Should standard liver treatment continue?
Yes. A stem cell clinic should not replace hepatology care. Antiviral treatment, alcohol avoidance, metabolic control, medication, transplant evaluation, and routine liver monitoring may still be essential depending on the case.