Why this topic keeps getting attention
When people search stem cell therapy Thailand for Disc Degeneration, they are usually not looking for abstract science. They are looking for something more hopeful than painkillers, more durable than a temporary flare-up fix, and more biological than “just live with it.” That reaction makes sense. Degenerative disc disease is a major contributor to chronic low back pain, and low back pain itself remains one of the leading causes of disability worldwide.
The problem is that the phrase stem cell shots for back pain sounds much simpler than the actual science. Back pain is not one diagnosis. Chronic primary low back pain, discogenic pain, facet-related pain, muscular pain, and nerve-related pain are not interchangeable problems. That is why the stem cell conversation only really becomes meaningful once the pain generator is narrowed down, especially when the suspected source is degenerative disc disease rather than “back pain” in general.
Why Disc Degeneration became a regenerative medicine target
Disc degeneration creates a treatment gap
The traditional treatment for many of these conditions achieves partial or even complete symptom relief without altering the actual disc biology, which is one reason regenerative medicine keeps coming back to spine care. The 2025 systematic review of stem cell therapy for degenerative disc disease states this specifically: current therapies, from conservative care to fusion do not reverse the molecular degeneration itself creating a true treatment gap [4]. And that, it seems, is where stem-cell-based strategies became appealing.
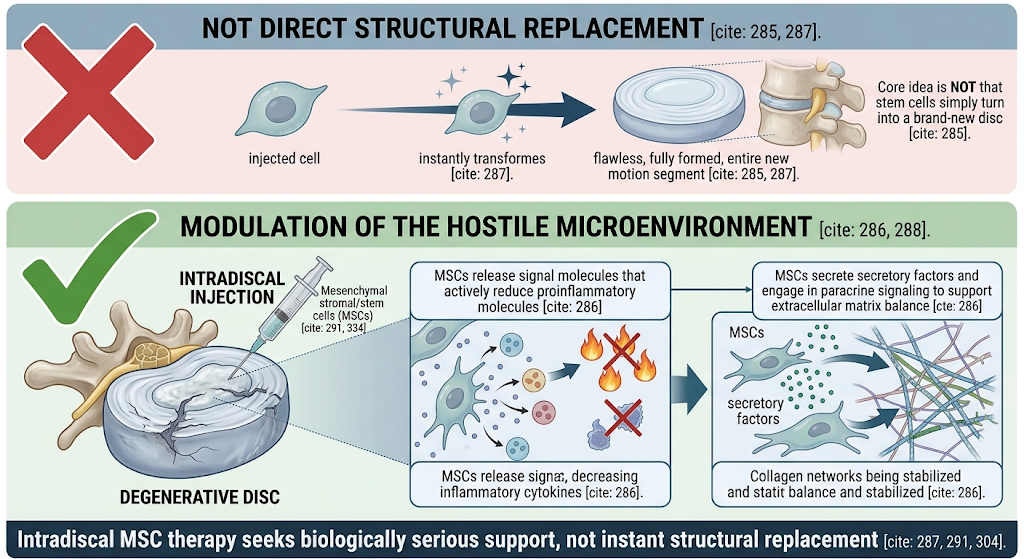
The biology is more interesting than the marketing
The core idea is not that stem cells simply turn into a brand-new disc. Current reviews describe a more subtle mechanism: stem cells may help modulate inflammation, support extracellular matrix balance, and influence the hostile disc microenvironment through regenerative and paracrine effects. That distinction matters, because the best current science does not describe stem cell therapy as magical structural replacement. It describes it as an attempt to improve a biologically difficult environment.
What “stem cell shots for back pain” usually refers to
Usually, it means intradiscal injections for discogenic pain
In the actual clinical literature, stem cell shots for back pain typically refers to intradiscal mesenchymal stromal/stem cell injections in lumbar degenerative disc disease and discogenic low back pain. The 2026 randomized-trial meta-analysis featured here addressed intradiscal MSC therapy for lumbar degenerative disc disease, while the 2025 systematic review instead focused on intervertebral disc regeneration strategies related to pain, disability and MRI findings.
This is not a blanket treatment for every bad back
That point is easy to miss online. These studies are not saying stem cells are a general answer to any person with back pain. They are studying selected patients with suspected discogenic pain from disc degeneration. That is a much narrower and more honest frame than broad clinic language sometimes suggests.
What the evidence actually shows right now
The results are promising, but modest
This is where the conversation gets productive. The 2026 PubMed-indexed meta-analysis concludes that intradiscal MSC injection is safe and effective, but also characterizes the clinical benefit as modest improvements in pain and function. The 2025 systematic review makes a related point from the wider perspective: clinical trials reported small but statistically significant improvement in pain and disability, whilst safety over shorter term to mid-term appeared acceptable.
The field is still limited by trial quality
The same 2025 review also adds the part people most need to hear: clinical evidence is still limited, imaging proof of true biological repair is not compelling, and existing trials have significant methodological weaknesses. That is a very important sentence for anyone evaluating regenerative claims. It means the field is scientifically serious, but not clinically settled.
Even supportive guideline work still implies caution
The issuance of a 2025 update by the American Society of Interventional Pain Physicians on regenerative therapies for moderate to severe chronic low back pain is evidence that this field continues apace, requiring an evidence-based review. However, that does not necessarily mean stem cell injections have become a common routine standard of care. This means that the evidence base is thicker and we are still figuring it all out.
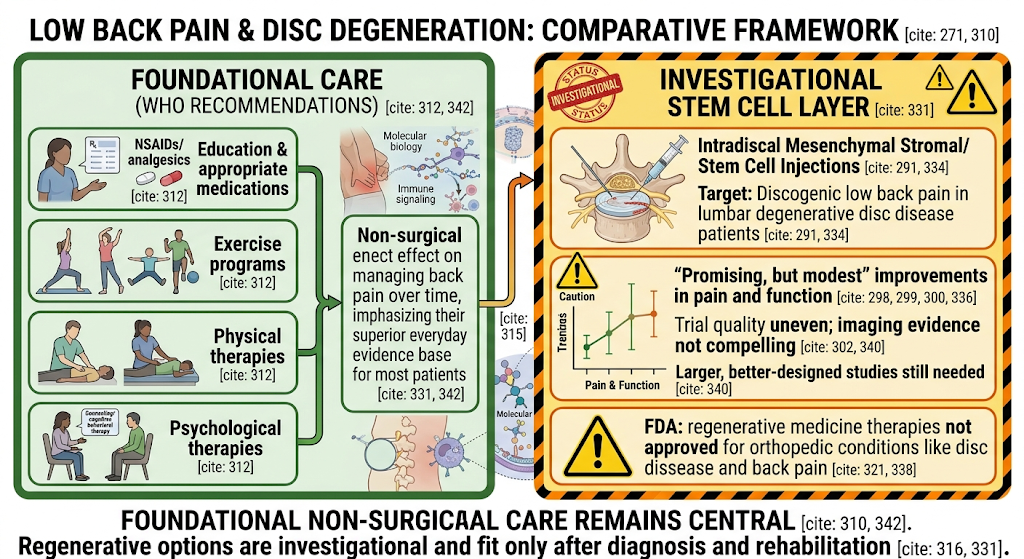
Why standard care still matters more than many people expect
Most people with chronic low back pain still need foundational care first
This part may sound less exciting, but it is clinically more honest. WHO’s guideline for chronic primary low back pain recommends non-surgical care such as education, exercise programs, some physical therapies, psychological therapies, and NSAIDs where appropriate. WHO also emphasizes that a suite of interventions may be needed instead of relying on a single intervention in isolation. That is worth remembering whenever a regenerative therapy is presented as though it should replace everything else.
Good regenerative care should sit on top of good spine care
In practical terms, that means the smartest discussion about stem cell therapy Thailand and Disc Degeneration is not “stem cells instead of everything.” It is “Where do regenerative options fit after diagnosis, rehabilitation, load management, and a careful assessment of what is actually driving the pain?” That usually leads to better medicine than chasing the flashiest option first.
What patients should know about clinic claims
Availability is not the same as approval
The FDA is very clear here: regenerative medicine therapies have not been approved for orthopedic conditions such as disc disease and back pain. The same FDA page also warns that if people are being charged for these products outside a clinical trial, they may be being deceived, and it lists serious risks including infection, immune reactions, tumor formation, and contamination. That is not a side note. It is central to how any clinic claim should be judged.
A credible clinic should sound more specific than dramatic
A trustworthy clinic conversation should be able to answer very plain questions: Is the pain truly suspected to be discogenic? What exact cell product is being used? What evidence supports that approach? What outcome measures are realistic? What remains uncertain? If the language sounds more confident than the published trials do, that is usually a sign that the marketing is stronger than the evidence.
The most honest conclusion
The neatest way to put it is stem cell therapy Thailand and Disc Degeneration need a hard science conversation — not a fantasy one. The biologic rationales are sound, the trial results promising and stem cell injections in selected discogenic low back pain cohorts have demonstrated modest improvements. But the field is still investigational, overall benefits are modest at best and standard non-surgical spine care maintains a superior everyday evidence base for most patients.
Frequently Asked Questions
1) What do “stem cell shots for back pain” usually mean?
Usually, the phrase refers to intradiscal mesenchymal stromal/stem cell injections being studied for lumbar degenerative disc disease and discogenic low back pain, not for every type of back pain.
2) Do stem cell injections for disc degeneration work?
Current studies suggest they may provide modest improvements in pain and function in selected patients, with acceptable short- to mid-term safety, but the evidence is still limited and not definitive.
3) Are stem cell treatments approved for back pain?
No. FDA says regenerative medicine therapies have not been approved for orthopedic conditions such as disc disease and back pain.
4) Why are these treatments still considered investigational?
Because trial quality remains uneven, imaging evidence of true disc repair is still not compelling, and larger, better-designed studies are still needed before routine use can be justified.
5) What still matters most in chronic low back pain care?
WHO still recommends foundational non-surgical care such as education, exercise, some physical therapies, psychological support, and appropriate medications, with care tailored to the whole person rather than built around one intervention alone.