Back pain has become one of the most prevalent causes of discomfort, restricted movement, work incapacity and chronic disability across the globe. Chronic back pain can be related to intervertebral disc degeneration, inflammation, nerve irritation, facet joint problems, muscle dysfunction or structural changes of the spine even though many cases improve with conservative care. Over the last few years, stem cell therapy Thailand has emerged as a major search term in patients with chronic pain related to the spine looking for regenerative solutions.
UC-MSCs stem cell therapy for back pain are investigational indications with umbilical cord-derived mesenchymal stem cells as a tool to assist the homeostasis of biological pathways involved in inflammatory modulation, paracrine signal transduction, extracellular matrix state unity and inter vertebral disc microenvironment. Regenerative therapies targeting lumbar degenerative disc disease: literature review with meta-analysis in human MSC-based clinical trials. A 2024 literature review on regenerative therapies for lumbar degenerative disc disease stated that human clinical trials involving MSCs have provided the basis for pain reduction and functional improvement but also emphasized that clinical translation remains limited by key challenges that remain to be established through further studies.
Thus, UC-MSCs for back pain should be framed as an investigational regenerative approach; not a panacea or substitute to standard spine care.
Back Pain Is More than a Simple Muscle Problem
Chronic low back pain (CLBP) is often treated as a lifestyle problem or simply a consequence of aging, yet it may have more profound biological and structural changes. Intervertebral discs can degenerate with loss of disc hydration, proteoglycan content and disc height. Annular fissuring, inflammatory cytokine activity in the disc, altered biomechanics (destruction of normal load bearing function), nerve irritation by inflammation and barely able to maintain its own collagen tissue is not just a model for degenerating discs. These changes can lead to pain, stiffness, decreased flexibility and loss of motion in your daily movements.
Internet Cognitive Behavioral Therapy ICBT for low back pain, Contrast with Standard Care Standard care for back pain can include medication, physical therapy and exercise rehabilitation, lifestyle modification, image-guided injections or spine surgery in selected severe cases. While many traditional approaches focus on symptomatic relief, these approaches primarily target symptom resolution in the short term instead of directly rebuilding a viable biological scaffold that serves to restore structure and function in the degenerated disc. This is the main reason, why regenerative medicine has been investigated as a potential adjunctive option for certain patients with discogenic low back pain.
Therefore, stem cell therapy Thailand for back pain should be described as a treatment option that should be considered under medical guidance and based on scientific evidence, not something one-size fits all type of treatment for every kind of back pain.
Regenerative Overview of Back Pain
2.1 Intervertebral Disc Degeneration
Composed of Nucleus Pulposus, Annulus Fibrosus and Cartilaginous endplates. The nucleus pulposus is to absorb pressure and provide spinal cushioning. Degenerative changes in the disc can lead to loss of water content, proteoglycans and structural integrity which may affect its ability to cushion the vertebrae (shock absorption) as well as contribute to chronic pain.
2.2 Inflammation and Pain Signaling
Disc degeneration is not merely a mechanical problem. Inflammatory mediators (IL-1β, IL-6 and TNF-α) related with degenerating discs and pain-related changes. Inflammation might have a role in making the nerves more sensitive, irritation of the tissues, and keeping pain cycles alive.
2.3 Why UC-MSCs are Investigated
UC-MSCs are the subject of investigation because they may have immunomodulatory, anti-inflammatory, paracrine and tissue-supportive effects in both a nursing role directly on tissue and an indirect role through stimulation of other cells. The umbilical cord mesenchymal stem cells for intervertebral disc degeneration: future directions and potential use in regeneration with clinical relevance may ensure an important improvement by offering new avenues for regenerative strategies of disc repair – However, more robust evidence and critical evaluation are required before clinical translation.
Stem Cell Treatment for Back Pain
The scope of UC-MSCs stem cell therapy for back pain is mostly the investigational use of reasonably umbilical-vein derived mesenchymal stem cells in adults with selected musculoskeletal pathological conditions, particularly discogenic low back pain or intervertebral disc degeneration.
It is not an intention to just “replace” the disc or promote immediate pain relief. Specifically, researchers are analysing the possibility that UC-MSCs will modulate the disc niche through:
anti-inflammatory signaling
paracrine factor release
extracellular vesicle communication
extracellular matrix support
modulation of local cellular stress
possible Nucleus Pulposus-like cell activity
Injury Prevention — How Do UC-MSCs Benefit the Osteo-Cartilaginous Tissue?
4.1 Anti-Inflammatory Support
Our preliminary data suggests that UC-MSC infusion may be the treatment of choice to deliver a bioactive soluble factor/s that can regulate specific inflammatory pathways in disc degeneration and chronic low back pain. The significance of this mechanism is that inflammation involved on disc cell stress, hyperalgesia and local tissue degeneration.
A 2024 review describes the role of inflammatory cytokines and structural changes in degenerating discs and states that cell-based therapies are being developed in part to limit inflationary conditions within the intervertebral disc.
4.2 Paracrine Signaling
MSC = mesenchymal stem cell, paracrine signalling = signalling from cells that do not directly contact a tissue in which they exert their effectsMany people think MSCs are acting generally by secreting something to affect the behaviour of nearby cells (paracrine signalling) rather than as committed progenitor cells replacing tissues. This, in turn, implies that UC-MSCs can secrete cytokines and growth factors as well as extracellular vesicles and other signalling molecules modulating the activity of neighbouring disc cells, immune cells and local tissue microenvironment.
Inflammatory back pain translates to the degenerative disc environment and in relation to that, paracrine signaling may be important for shifting this degenerative environment towards a more reparative or less inflammatory state.
4.3 Support of Disc Microenvironment and Extracellular Matrix
In intervertebral disc degeneration, loss of proteoglycans and organization of collagen are reported. Contributing to balancing the extracellular matrix and improving the biological environment of the disc in degenerative state, UC-MSCs are into focus.
Now, this does not mean UC-MSCs can recreate an entire rotten disc in anybody. Instead, the scientific question is if these cells support matrix related signalling and tissue homeostasis in specific cases.
4.4 Pain and Functional Support
In clinical studies applying MSC-based approaches to target intervertebral disc degeneration, improvements in pain and disability scores have been reported in some patient groups. Nonetheless these results depend on cell source, dosing strategy, delivery route, disease stage, patient selection and follow-up period. A 2024 review has concluded that human MSC trials showed promising pain and function outcomes, with a note of rationale for further study.
Current Clinical Evidence
5.1 Promising Yet Limited Human Evidence
Clinical studies of MSCs for discogenic low back pain have included bone marrow-derived MSCs, adipose-derived MSCs and umbilical cord-derived MSCs. For example, a review summarised human studies and reported that several MSC trials have shown improvements in pain and function over time in patients with intervertebral disc degeneration.
Data specific to UC-MSC is still much less abundant than some other sources of MSC. One PubMed indexed study of human umbilical cord mesenchymal stem cell transplantation for chronic discogenic low back pain reported promising early clinical outcomes, but this must be interpreted in the context of preliminary findings, not conclusive.
5.2 UC-MSCs Are Still in Clinical Assessment
ClinicalTrials. We searched in pubmed and clinicaltrials.gov, for studies assessing human umbilical cord mesenchymal stem cells for lumbar disc degeneration or lumbar discogenic pain. As an example, one of the listed study aimed to involve hUC-MSCs to evaluate lumbar disc degeneration and another studies early-stage lumbar discogenic pain. These registrations indicate the field is still under clinical investigation rather than an established standard of care.
5.3 Standardización de la investigación
However, a strong limitation in the studies regarding UC-MSCs stem cell therapy for back pain is that they differ significantly by cell source, range of cell dose employed, culture method, route of injection or patient diagnosis, imaging criteria used to evaluate response and follow-up time-point. This heterogeneity means that findings from one study cannot simply be applied to all individuals with back pain.
Thailand as a Regenerative Spine Care Destination
However, Thailand is now a destination for overseas health care, wellness and regenerative medicine consultation. For patients who are looking for stem cell therapy Thailand, back pain is a popular problem due to the impact of chronic spinal pain on mobility, sleep, travel, work and quality of life.
Interestingly, we regularly advocate for stem cell therapy Thailand for back pain. Regenerative approaches must follow proper medical assessment, appropriate imaging review, neurological screening and discussion of standard spine-care options with patients.
FAQ Section
Can UC-MSCs cure back pain?
So, you cannot say that UC-MSCs can cure back pain. UC-MSCs might be rather promising stem cell type for these purposes since back pain can have a few reasons, UC-MSCs are solely being investigated for some conditions like discogenic low back pain and intervertebral disc degeneration. The evidence is new but promising.
Physiotherapy or standard of care for spine is not replaceable by UC-MSCs
No. it is not appropriate to present UC-MSCs as an alternative for physiotherapy, exercise rehabilitation, medical assessment, pain management or spine specialist treatment. This should be in the context of a medically assisted, comprehensive strategy only.
UC-MSCs are being investigated as the cure for back pain, why not?
UC-MSCs are currently being investigated since they instruct the secretion of cytokines and growth factors, as well as extracellular vesicles and other bioactive molecules that can affect inflammation, disc-cell stress, ECM constitution and turnover, and the IVD micro-environment.
Background information required before UC-MSCs can be considered safe for back pain
They may include MRI finding, the site, severity and duration of pain, neurological symptoms laboratory results, previous treatments and its effectiveness, medication history functional limitation and whether it is disc degeneration nerve compression muscle dysfunction or any other spine-related issues.
Stem Cell therapy Thailand for back pain
Back pain centre Thailand may consult dedicated programs for you here at some regenerative medicine centers. Patients should seek out providers offering physician-led screening, cell sourcing in a manner that is clear to patients, imaging review when appropriate, adequate protocols for safety and realistic expectations.
Is the evidence strong enough?
The evidence is promising but not yet definitive. Results of studies utilizing MSC based strategies for IDD expectantly indicate that these therapies may not only reduce pain but also improve function in some patients with disc degeneration, although this will require larger high-quality well standardized long-term clinical trials.
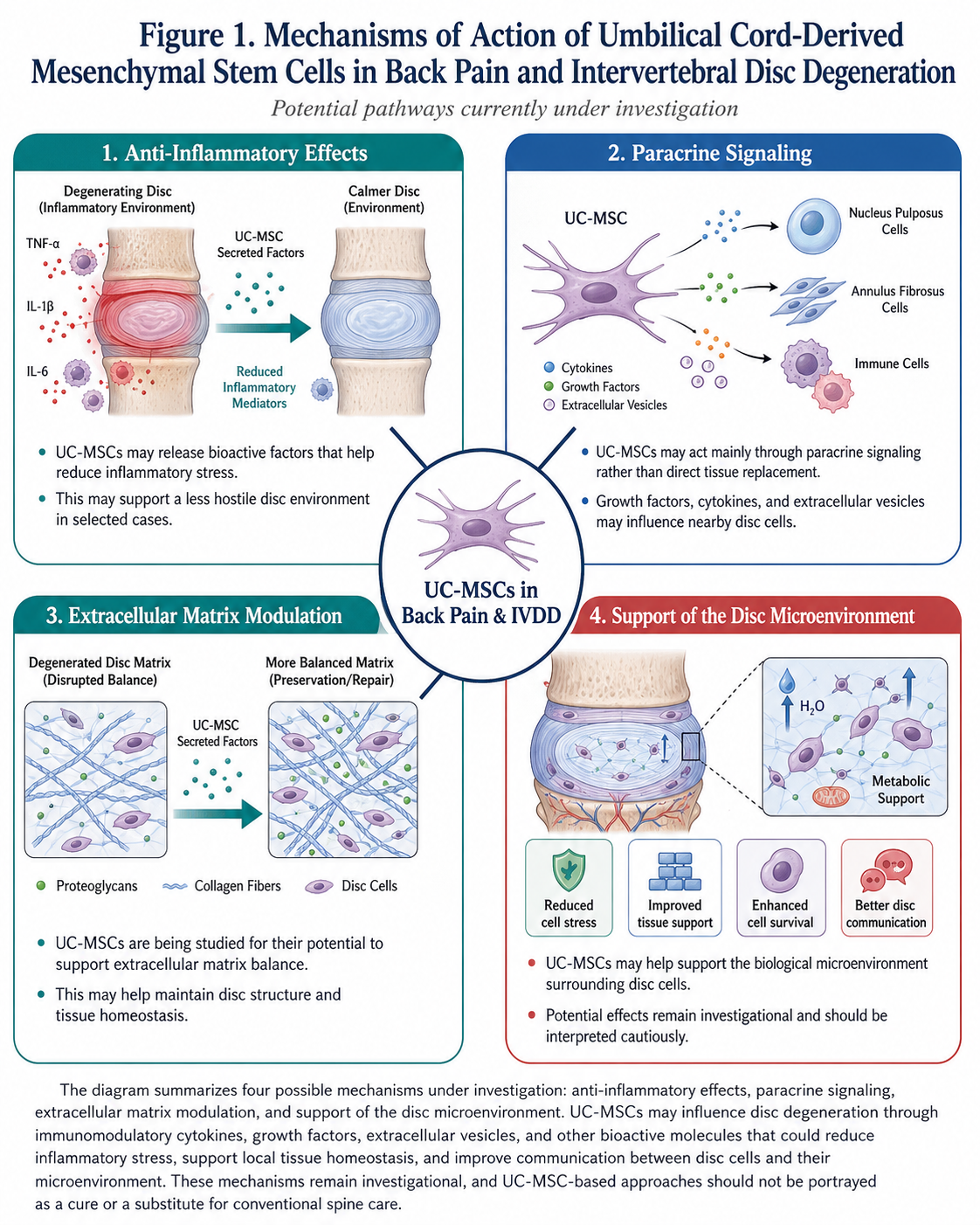
The diagram summarizes four possibilities being explored as mediators of therapeutic disc regeneration: (1) anti-inflammatory effects, (2) paracrine signaling, (3) extracellular matrix modulation, and (4) support of the disc microenvironment. The therapeutic effects of UC-MSCs on the degeneration induced by back pain may be a consequence of their ability to secrete immunomodulatory cytokines, growth factors, extracellular vesicles and other bioactive molecules that could curb inflammatory stress, maintain local tissue homeostasis and enhance communication between disc cells and their microenvironment. The mechanisms underlying these are still investigational, and UC-MSC-based approaches should not be portrayed as a cure or a substitute to conventional spine care.

