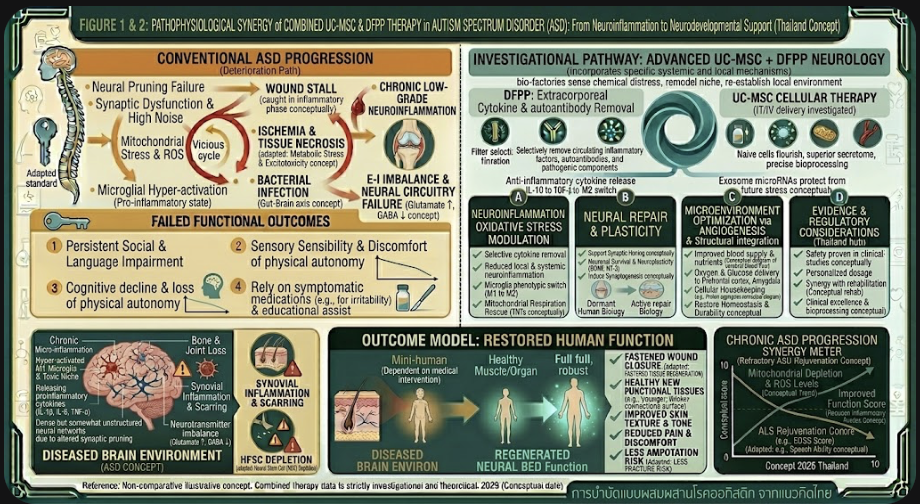
Autism Spectrum Disorder (ASD) is now viewed as a patterned neurodevelopmental disorder shaped by genetics and environmental factors. While still mostly interpreted as behavior, ASD has transitioned to be integrated with brain development and immune regulation topics such as neuroinflammation, synaptic activity, and cell–cell communication.
Under these circumstances, umbilical cord-derived mesenchymal stem cells (UC-MSCs) are gaining more popularity among the field of regenerative medicine. Rather than directly “replacing” brain cells, the goal is to prop up the biological landscape where nervous system interactions ensue.” Modeling UC-MSC-based approaches focused on promoting immune-modulation, paracrine signaling, mitochondrial support and vascular regulation may help to establish a more conducive local microenvironment for learning, adaptation and functional recovery.
Biological Features Associated With ASD
There are many biological pathways that overlap in ASD. Not everyone is the same, but there are a number of mechanisms which have typically been discussed in the literature.
Neuroinflammation and Microglial Activation
Microglia are immune cells in the brain responsible for maintaining neural health. Microglia have been characterized as hyperactivated with their production of inflammatory mediators such as IL-1β, IL-6, and TNF-α in some ASD-associated research. Chronic presence of this inflammatory state can disrupt neuronal signalling, brain development and synaptic organisation.
Altered Synaptic Pruning
In the course of normal brain development, less efficient and redundant neural connections are honed such that optimal circuits operate more effectively. This process may be impaired in ASD leading to dense yet somewhat unstructured neural networks. This can have an impact on sensory processing, communication, attention and social interaction.
Excitation–Inhibition Imbalance
Related to this is the balance between excitatory and inhibitory signalling, also a major idea in ASD biology. Too much activity in the neurotransmitter glutamate or too little inhibition related to GABA may result in sensory sensibility, irritability, disrupt assistive sleep, mood dysregulation and an inability to filter environmental input.
These mechanisms substantiate consideration for targeting inflammation, cellular signaling, and neuroplasticity as opposed to solely treating outward behavioral symptoms.
Limitations of Current ASD Management
However, current ASD care typically incorporates behavioral therapy, occupational therapy (OT), speech therapy, educational assistance and sometimes medications as needed. These may include medications for irritability, hyperactivity, sleep disturbance or severe behavioral dysregulation.
Nevertheless, these treatments do not directly address all of the biological processes that underlie ASD, including chronic inflammation, divergent immune signaling, mitochondrial stress or synaptic development. Filling this gap has motivated the investigation of regenerative and cell-based strategies that may enhance the endogenous repair environment within the brain.
MODE OF ACTION—HOW UC-MSCs MAY ASSIST IN NEURODEVELOPMENTAL FUNCTION
UC-MSCs should not be thought of as simple replacement cells. The bulk of their proposed actions derive from the biological signals that they release and how they respond to the immune system and damaged tissue environments.
Immune Regulation and Inflammation Control
Introducing MSCS to high IRR, inflammatory signals can be used as initiators that activate UC-MSCs which release sufficient anti-inflammatory molecules for the regulated resolution of inflammation. Including but not limited to anti–inflammatory cytokines like IL-10 & TGF-β and immunoregulatory enzymes including IDO.
In principle, this could help push microglia away from high inflammatory state and more towards a repair-supportive microglial profile By decreasing neuroinflammatory load, the biological milieu may be less repressive of neural networking and modulatory therapies applied.
Paracrine Signaling and Neurotrophic Support
Paracrine signaling is one of the key mechanisms of UC-MSCs. Rather than acting simply as cells, UC-MSCs release growth factors, cytokines, extracellular vesicles (EV), and exosomes that have far-reaching effects on nearby cells.
The secreted factors could include neurotrophic molecules like BDNF and NT-3 known to promote neuronal survival, synaptic support, and neuroplasticity, which are consistent with the function of MN. This signaling may support the brain in its ability to adapt, learn and respond to therapy in an ASD-focused context.
Mitochondrial and Cellular Energy Support
Some autism spectrum disorder (ASD) literature discusses mitochondrial dysfunction and oxidative stress. UC-MSCs have been evaluated for their potential to mediate cellular energy balance, including through mechanisms related to extracellular vesicles as well as mitochondrial transfer in experimental systems.
UC-MSC-related mechanisms may facilitate more stable cellular function by improving the metabolic state of stressed cells. This does not guarantee a difference in neurological recovery, but it allows an evidenced-based rationale for continuing the pass through testing.
Supporting Blood Flows in Arteries and Its Branches
Alternatively, UC-MSCs can secrete pro-angiogenic factors including VEGF that are engaged in angiogenesis and tissue perfusion. So with the microvasculature support improved, it may help by providing oxygen and nutrients to brain areas responsible for attention, emotional control and executive functions better.
This vascular-support mechanism is still under investigation, but it is one reason why regenerative medicine has been talked about more during discussions of neurodevelopmental and neurological conditions.
UC-MSC Therapy and Clinical Practice: Thailand
Thailand is now branded as a hub for regenerative medicine in Asia, including programs on UC-MSC. Delivery of care for ASD should occur in a clinical model that is ultimately the most responsible with respect to safety, quality control, medical supervision and integration into established therapies.
Laboratory Quality and Cell Processing
It has high-quality requirements including controlled processing in a laboratory, strict donor profiling and screening, sterility testing, identity confirmation, viability test and potency-related evaluation. All the above steps are crucial for uniformly and safely preparing cells to be used for clinical applications.
Medical Supervision and Individualized Planning
Due to the high variability of ASD, there is not one protocol that works for every child or adult. The treatment plan should include the review of medical history, developmental evaluation, and neurological evaluation when indicated. Goals and limitations should be carefully discussed.
Integrated with Rehabilitation and Developmental Therapy
Do not frame UC-MSC therapy as an isolated endpoint. The most pragmatic model, modeled after comprehensive fashion determined by whom these children are and one that integrates regenerative support together with speech therapy, occupational therapy, behavioral intervention, nutritional support, sleep management and long-term follow-up of developmental manifestations.
Perhaps the most clinically relevant value would lie in reforming the brain to better accommodate structured learning and rehabilitation if UC-MSCs are capable of enhancing this biological milieu.
Conclusion
UC-MSC therapy is a novel and potentially valuable type of regenerative medicine for Autism Spectrum Disorder. It has a suggested value in immune modulation, attenuation of inflammatory signaling, paracrine signaling, mitochondria support, and maintenance of the neural niche.
However, we must remember that ASD is a heterogeneous disorder and thus UC-MSC therapy cannot be presented as a curative or definitive treatment. This is consistent with the most balanced interpretation that UC-MSCs may provide a biological substrate that could enhance contemporary developmental and behavioral therapies in select cases.
Prioritizing safety, scientific reasoning, personalized care, and realistic expectation will fold UC-MSC-based approaches into a wider conversation about the role of regenerative medicine in neurodevelopmental health.