Progressing liver fibrosis damages the liver and has a monumental global health impact, affecting the quality of life of millions of people. It is caused by chronic damage to the liver. Chronic damage from the liver can come from viral infections and metabolic chronic injuries, including diseases such as Non-Alcoholic Fatty Liver Disease (NAFLD). The damage caused by liver injuries lead to the degrees of transform by a healthy liver to a damage, a reed like tissue. Liver damage leads to organ failure that eventually results to death. The current pharmaceutical options available have no capacity to counter damage caused by liver injuries and fibrosis. Researchers are beginning to provide new ways for Liver fibrosis trials through regenerative medicine Thailand to manage chronic liver fibrosis. Researchers have started new cellular modalities to restore normal functioning tissues to populations afflicted by chronic tissue damage.
1.The Mechanism of Occurrence
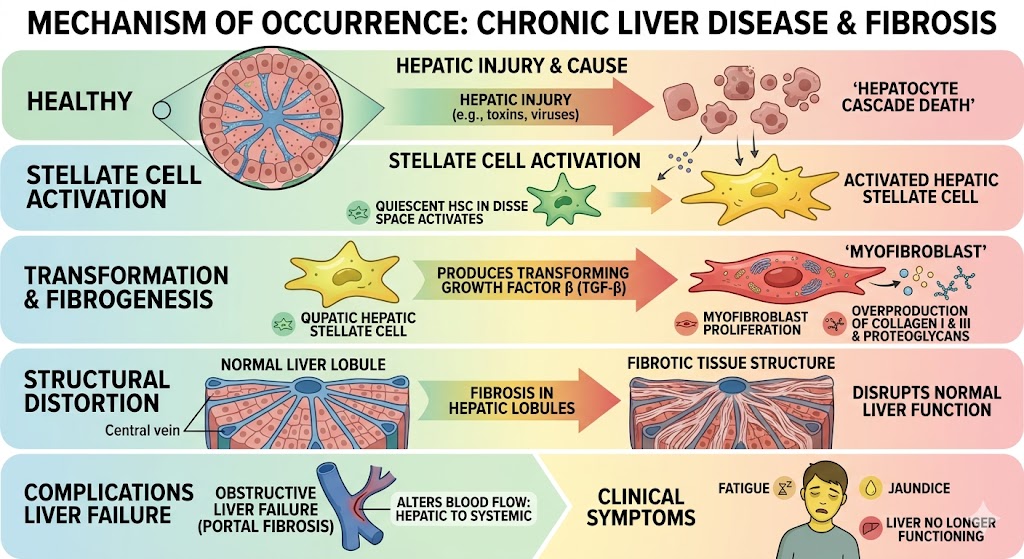
Chronic liver disease has a wide range of pathophysiological processes currently studied in Liver fibrosis trials. Major damage to the liver comes from hepatic injury, it involves hepatocyte cascade death that activates quiescent hepatic stellate cells that are in the Disse space. Activated cells produce an inflammatory cytokine called Transforming Growth Factor β (TGF-β), which proliferates into Myofibroblasts. Myofibroblasts tend to proliferate and overproduce, which is caused by an excessive amount of collagen type I and III and through a pathway of Proteoglycans, fibrosis in hepatic lobules disrupts normal liver function, which is hepatic lobules fibrotic tissues structures. The development of fibrotic tissues causes obstructive liver failure also referred to as portal fibrosis, which results to the blood flow in the hepatic circulatory system to change from hepatic to systemic. It causes fatigue and jaundice because the liver is no longer functioning. Understanding this gradual structural degradation is a priority for regenerative medicine Thailand, as it ultimately results in the final stages of hepatic decompensation, requiring rapid intervention to save the patient’s life.
2.Traditional Treatments
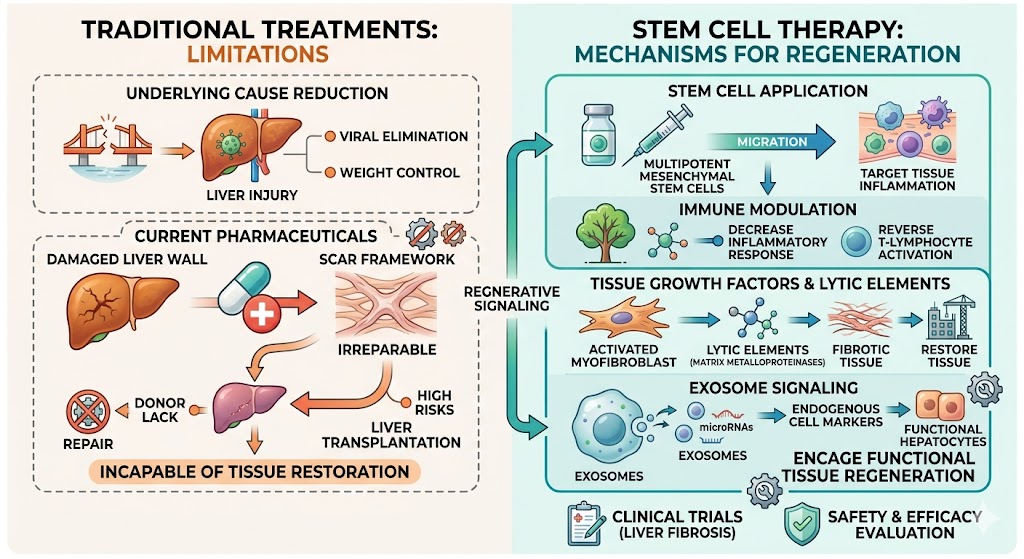
Physicians have long accepted that the best way to reduce injury to the liver is to treat the underlying fuel of the injury. To escape the injury, one must follow either viral elimination plans or, in extreme cases, weight control. Most current pharmaceutical agents target the lytic elements of the inflammatory chain that damage the liver wall but are incapable of tissue restoration. These therapeutic approaches have a significant weakness. They cannot restore advanced scars to a state of softness, which is merely lost to further concessions. The extracellular scar tissue framework, once consolidated, is virtually irreparable. The only complete repair of an irreversibly injured liver tissue occurs during organ transplantation; however, the lack of compatible donors and the high risks of the operation create a significant gap that must be filled by regenerative medicine Thailand and evaluated through Liver fibrosis trials to reverse the scarring of the liver.
3.Stem Cell Therapy Mechanisms
The use of multipotent mesenchymal stem cells is a highly sophisticated biological resource for the degradation of the otherwise irreversibly advanced scarring of fibrotic tissue. These cells have the ability to decrease the intensity of the hepatic fibrotic inflammatory response through the reversal of the activation of the targeted T lymphocytes. They migrate to the inflammatory lesion in target tissues by crossing the hepatic barrier, and through the controlled mechanisms of their cellular immune response, they synthesize a variety of tissue growth factors including endogenous lytic elements. These lytic elements are called matrix metalloproteinases, which are enzymes that degrade fibrotic tissue, and, in the case of their use, they restore tissue deformed by fibrosis. When stellate cell activation occurs, microRNAs are incorporated into exosomes that are released to halt further activation. This microRNA form of signaling encourages endogenous cell markers to expand to functional hepatocytes. This regenerative signaling process contrasts with symptom management as it goes beyond the biological process of cellular signaling at the micro-scale to counteract structural deterioration. Numerous ongoing Liver fibrosis trials evaluate the safety of activating this precise signaling. The application of these biological tools illustrates the potential of structural regeneration driving regenerative medicine Thailand beyond any current medical treatment.
4.Future Trends in Thailand
The localization of sophisticated biomedical systems places Southeast Asia at the forefront of cellular research. Biotechnology integrated into medicine creates government-funded research centers that facilitate frameworks of translational medicine. As even more advanced specialized regenerative medicine Thailand systems develop, public and private partnerships in this supportive regulatory environment allow for the control of global clinical standards. In a secure and sterile lab environment, the region possesses the tools to cultivate quality multipotent cells. This ecosystem incorporates a diverse patient base and highly qualified medical practitioners. Thailand establishes trustworthy partnerships to maintain patient safety as therapeutics move from an experimental stage to the clinical application stage during Liver fibrosis trials. The country has the potential to be the leading cellular-based advanced regenerative medicine provider supporting chronic metabolic disease within the region.
As the research and application of cellular therapies to address fibrotic longitudinal hepatic damage has been successfully developed, the future of patients suffering from hepatic damage will look even brighter. Tissue damage and organ failure occur in stages and are notoriously difficult to reverse using conventional medical approaches. From this clinical perspective, multipotent cellular modalities innovate in therapeutic intervention by offering cellular rejuvenation of tissues and degrading fibrotic tissue. Creating a more expansive infrastructure in regenerative medicine Thailand strengthens a solid base for therapeutic cellular interventions to proliferate. The ultimate therapeutic value of these treatment paradigms will be determined by the long-term outcomes associated with well-structured Liver fibrosis trials. The horizon promises radical innovation by offering the ability to transform the nature of advanced hepatic damage by making it a reversible, treatable condition rather than a progressive, terminal condition of organ failure.

