Natural Cellular Regeneration and Erectile Dysfunction: What PRP for ED Really Means
Why this topic keeps coming up
Erectile dysfunction is rarely just about sex
Most prominent when people are searching Natural Cellular Regeneration And Erectile Dysfunction, perhaps they notice that it poses a deeper question than any other. Although often described as a sexual problem, clinically, erectile dysfunction is better regarded as an expression of vascular disease (arterial or venous), diabetes, obesity, hormonal imbalance, neurologic problems, and cancer treatment side effects in addition to emotional stressors. Both the EAU guideline and NIDDK reinforce that ED has common risk factors with cardiovascular disease, as well as may be caused by abnormalities of blood vessels, nerves or hormones.
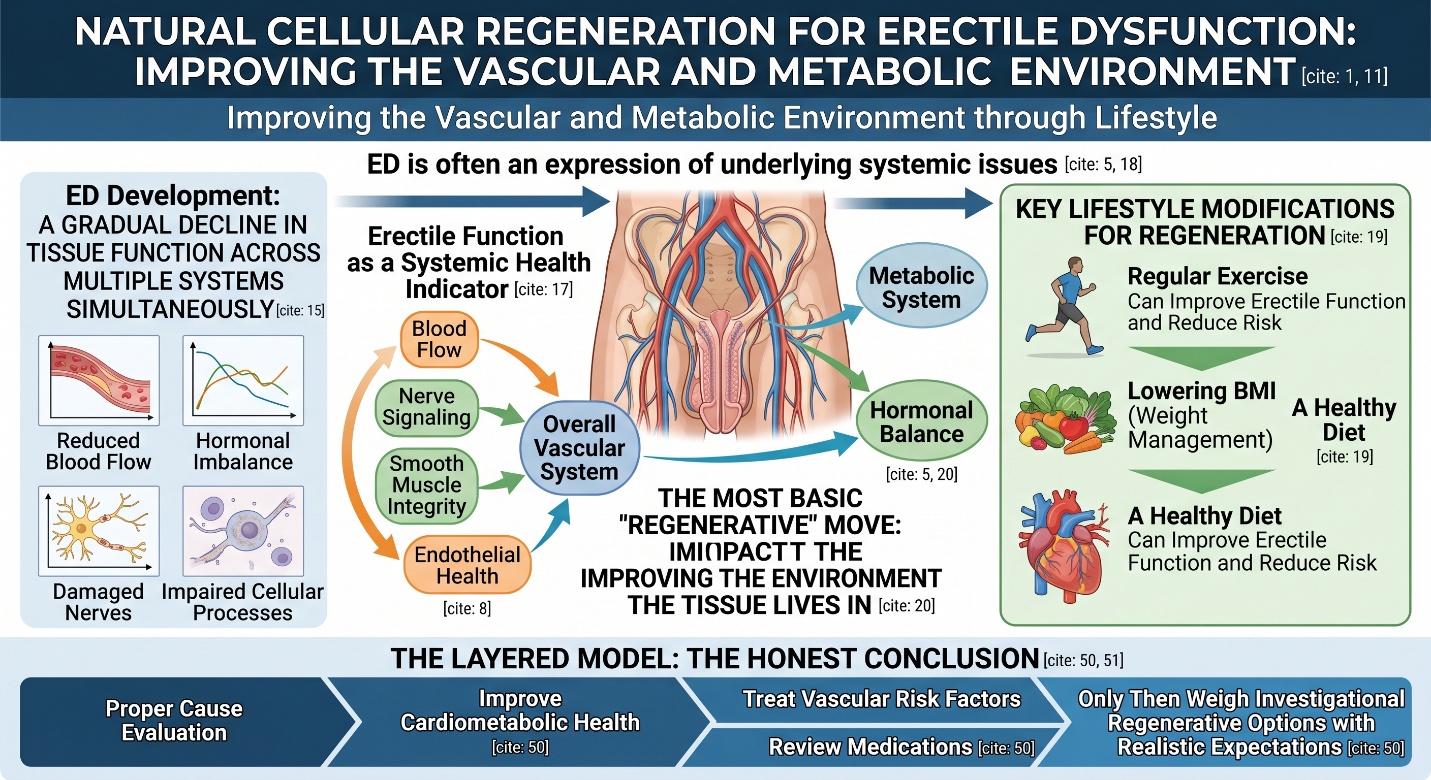
That is exactly why regenerative language feels so appealing here. If erections depend on blood flow, nerve signaling, smooth muscle integrity, and endothelial health, then it makes intuitive sense to ask whether damaged tissue can be supported rather than simply bypassed. The phrase Natural Cellular Regeneration taps into that hope. But hope is not the same thing as proof, and in erectile dysfunction the gap between biologic plausibility and established treatment still matters a great deal.
What “Natural Cellular Regeneration” should mean in ED
The real issue is tissue quality, not just temporary performance
Natural Cellular Regeneration in ED is best viewed not as a magical phrase, but through the lens of a framework. Normal erections [and their determination] involve a cascade of signaling events that include but are not limited to nitric oxide release, cavernosal smooth muscle relaxation, arterial inflow and trapping by the venous outflow as well intact neural input. In ED development, the problem is frequently not an absent switch but a gradual decline in tissue function across multiple systems simultaneously. Regenerative approaches provide the reason for hope: they seek (at least in theory) to ameliorate the underlying tissue environment, rather than just provoke a transient response.
Lifestyle still matters because the penis is not separate from the rest of the body
This is where the article needs its first layer. Many people look for regenerative treatment as though ED begins locally and stays locally. It usually does not. The EAU guideline states that lifestyle modification, including regular exercise and lowering BMI, can improve erectile function, while NIDDK notes that a healthy diet can reduce ED risk and improve symptoms. In other words, the most basic “regenerative” move is often not a procedure at all, but improving the vascular and metabolic environment the tissue lives in.
Where PRP for ED fits right now
Why PRP became one of the most searched regenerative options
The interest in PRP for ED is easy to understand. Platelet-rich plasma is an autologous product prepared from the patient’s own blood and concentrated for platelets and growth factors. In theory, that could support local healing responses, angiogenesis, and tissue signaling in ways that are appealing for mild-to-moderate organic ED. It sounds less invasive than surgery, more “natural” than drug dependence, and more biologically ambitious than symptom-only treatment. That combination makes it a very strong keyword and a very easy therapy to oversell.
What recent evidence actually says
This is where the story becomes more interesting, and more honest. The 2025 EAU guideline notes that a meta-analysis of randomized trials found a mean improvement in IIEF-EF score with PRP versus placebo at six months, and a newer systematic review and meta-analysis in World Journal of Men’s Health likewise reported statistically significant improvement in randomized comparisons. But the same EAU guideline immediately adds the key limitation: the evidence remains insufficient for a clinical recommendation because studies vary widely in timing, dosing, platelet concentration, activation methods, and overall protocol design.
The most important sentence is the cautious one
Despite all the buzz surrounding PRP for ED, its most definitive current status remains that of conservatism. According to the EAU guideline, intracavernous PRP should be limited to clinical-trial settings as larger and better-designed studies are still required to validate its efficacy and safety. But that does not render PRP ineffective. It means it is still investigational, and that matters if we are going to have a conversation about regenerative medicine without every interesting signal becoming an answer.
The stem-cell side of erectile dysfunction
Stem cell therapy is being studied, but it is not routine care
The same pattern appears with stem cells. According to the 2025 EAU guideline, stem cells as a regenerative treatment for ED are still under investigation. The guideline summarizes a systematic review of 18 phase I and II clinical trials involving 373 patients and notes that intracavernous stem-cell injection appeared safe overall, but efficacy remains uncertain because only four small trials were placebo-controlled and their findings conflicted. That is a strong sign of scientific interest, but not a green light for broad clinical certainty.
Why researchers are still interested anyway
The mechanistic rationale has not disappeared. A 2025 Frontiers review describes preclinical work suggesting that adipose-derived stem cells may improve erectile tissue biology through paracrine signaling, nitric oxide synthase pathways, cyclic GMP signaling, and favorable changes in the smooth-muscle-to-collagen balance. In plain language, researchers are not chasing stem cells for no reason; they are trying to see whether damaged erectile tissue can be biologically nudged back toward healthier function. The problem is that animal and mechanistic promise still has to survive the harder test of human clinical reality.
What this means for real patients
The keyword is exciting, but the best medicine is still layered
This is where the conversation becomes more human. Someone searching Natural Cellular Regeneration for Erectile Dysfunction is usually not looking for theory. He is looking for something that feels less temporary, less mechanical, and more restorative. That instinct makes sense. But the strongest current evidence still supports a layered model: evaluate the cause properly, improve cardiometabolic health, treat vascular risk factors, review medications, address hormonal issues when relevant, and only then weigh investigational regenerative options with realistic expectations.
The honest conclusion
So, where is the field at? PRP for ED is among the more hotly debated regenerative alternatives, with some promising trial signals in existence but still being considered investigational based on current guideline-level evidence. The experimental and scientific interest associated with stem-cell therapy for ED, although early studies suggest that the treatment is safe, it continues to be investigated as no clinical recommendation can yet be made. Regenerative medicine has made erectile dysfunction a more biologically interesting field than it was when we wrote that first commentary 10 years ago, but the science needs to mature before some of the bolder claims warrant broad confidence in their boldness.