Normal human growth is a tightly regulated process involving interaction between genetics, endocrine function, nutrition, and skeletal development. If the growth pattern of a child is sitting well below what would be expected, this indicates an issue that will influence not just physical development but confidence and social adjustment as well as cause considerable worry for the family. In a clinical context, short stature and growth delay are evaluated through hormonal, metabolic, nutritional and genetic pathways. But not all children respond equally well to standard endocrine treatment, particularly when the underlying problem is with the biological activity of the growth plate rather than just hormone production.
This has generated increasing scientific interest in regenerative medicine as a discipline that could one day help sustain or restore tissue-level function across select growth-associated conditions. Of the diverse cell types under investigation, umbilical cord-derived mesenchymal stem cells (UC-MSCs) have gained interest due to their trophic, immunomodulatory and tissue-supportive potential. Against the backdrop of this wider research landscape, Thailand has developed into a country that is increasingly linked to advances in clinical and translational development of regenerative medicine.
- Biological Basis of Linear Growth and Skeletal Development
In childhood, normal growth in height relies heavily on the activity of the epiphyseal growth plate, a specialized cartilaginous structure found at the ends of long bones. This area facilitates growth in a linear direction via endochondral ossification, wherein there is multiplication and enlargement of cartilage cells slowly replaced by osseous tissue. When this system works appropriately, children grow taller through their potential for growth based on genetics and stages of development.
However, in certain growth disorders, the growth plate may act suboptimally. This can be associated with endocrine disorders, nutritional deficiency, chronic disease, genetic factors or decreased cellular activity in the growth plate itself. In these circumstances, chondrocyte proliferation may diminish, the cartilage zone may be less active and skeletal development will be curtailed. This means that if the growth plates develop and fuse before enough height gain has happened, there is little to no potential remaining for extending the long bones of the skeleton. That is why it’s so often necessary to evaluate and manage pediatric growth concerns while the skeletal system is still actively growing.

- Conventional Approaches and Their Limitations
Recombinant human growth hormone (rhGH) therapy has been the most recognized medical treatment for some growth disorders. In children with documented growth hormone deficiency or certain related conditions, such treatment can be help and a significant piece of pediatric endocrinology. However, the response to therapy is not uniform and not all cause of short stature is due only to hormone deficiency.
European Society for Pediatric Endocrinology (ESPE) guidelines have recommended GH therapy in children with SHOX mutation, regardless of the extent to which they responded. In some patients, only a partial response may be seen and there are other underlying conditions like idiopathic short stature or tissue-level resistance that would only offer limited benefit from standard hormonal stimulation. Further, traditional therapies generally involve a longer treatment time and close monitoring. Due to these challenges, interest has slowly expanded upon understanding whether the biology of the growth plate itself can be a target for future treatment strategies.
That is not to say current endocrine care does not matter. On the contrary, it is still the basis for true management. But it does underscore the biologically diverse nature of growth disorders, and that one therapeutic pathway may not cover all underlying causes.
- Scientific Interest in UC-MSCs and Growth Plate Support
The interest in UC-MSCs for regenerative pediatric research stems from their secretory activity, as they can release biologically-active signals capable of modifying cell crosstalk responsible for cell regulation in inflammatory and reparative scenarios. Umbilical cord-derived mesenchymal stem cells are often mentioned as having a strong proliferative capacity and an active trophic secretome in comparison to many adult-derived cell sources.
Theoretically, these cells could potentially bolster the paracrine activity of the developing tissue microenvironment instead of directly replacing cells. This has led to inquiries within growth-related literature concerning the ability of UC-MSC-derived signals to help sustain chondrocyte health, matrix function, and the biological activity of the growth plate under specific settings. Frequently mentioned topics in this line of research include growth-associated mediators, e.g. IGF-related signaling and tissue-regulating pathways.
On the one hand, this needs to be presented carefully. UC-MSC-based therapy for pediatric enhancement of height is neither a standard treatment for low height concerns nor should it be promoted as a reliable tool for increasing height. The scientifically more responsible statement looks forward, suggesting that regenerative medicine is being investigated for potential utility in selective growth-related disorders, particularly where support at the level of tissue becomes the subject of scientific inquiry.
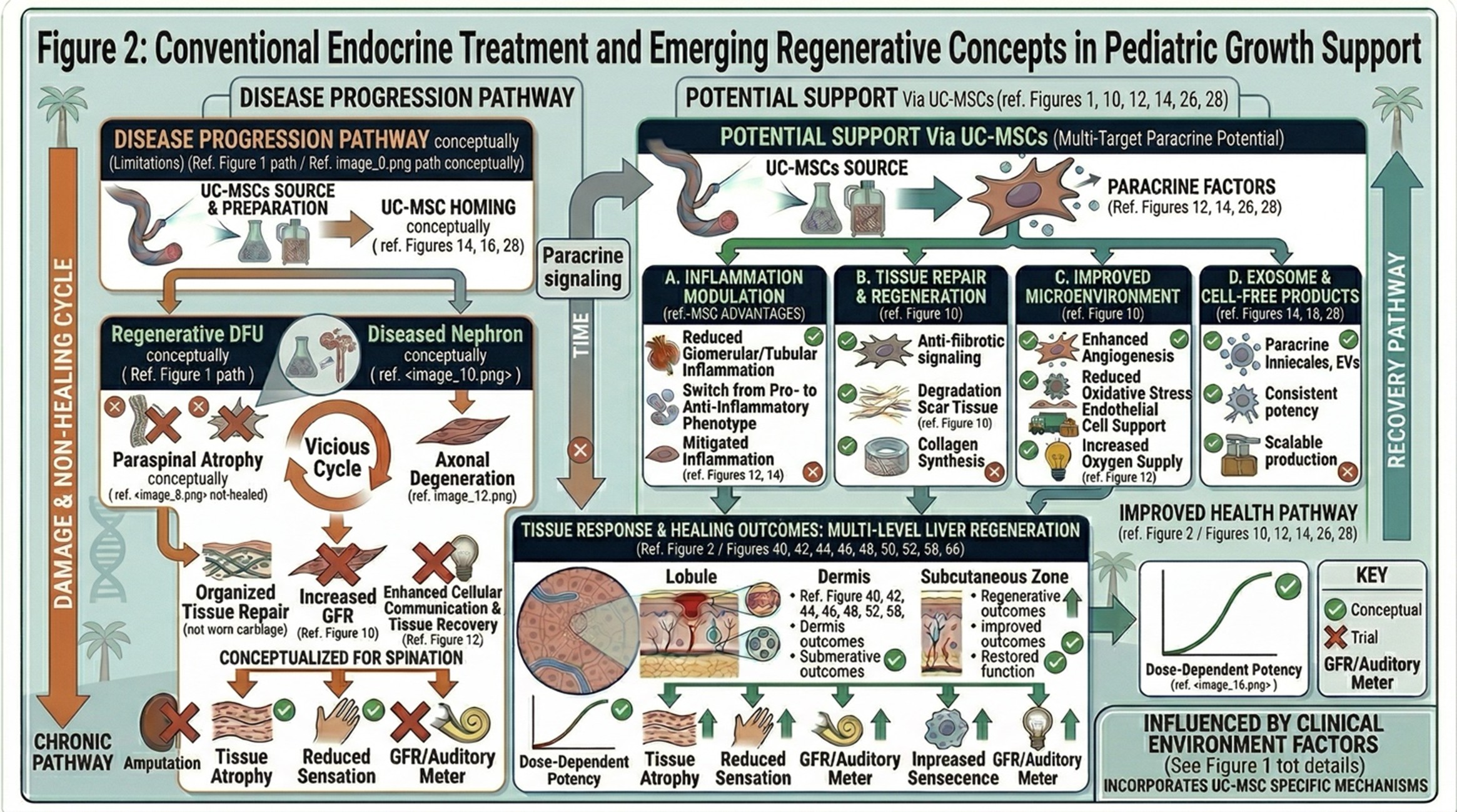
- Regenerative Medicine Development in Thailand
Thailand is becoming increasingly known in the field of regenerative medicine due to its growing life science infrastructure, international patient care and ongoing clinical interest in advanced biologic therapies. In certain areas of medicine, this has incentivised a shift toward tailored treatment paradigms that integrate laboratory-supported biologics with physician-guided clinical evaluation.
But in pediatric care, any consideration of regenerative intervention must be particularly measured and informed by ethical considerations. We need to do better divided into Sometimes it is a drugda in small children will not be Safety Must take priorityover proven medicine and investigational approaches. This holds true especially for growth-related disorders, where numerous causes can be recognized and treated conventionally through pediatric endocrinology.
The significance of the Thai program in this space stems less from high-level assertions but rather from choices made about infrastructure and capacity that might serve future research. As regenerative medicine advances, its place in treating growth disorders in children will require more powerful scientific proof, nonambiguous ethical guidelines and well-controlled clinical trials.
- Concluding Perspective
Deeper insight into skeletal biology, growth plate biology, and tissue-level regulation of growth is revolutionizing the management of pediatric growth disorders. Standard endocrine therapies are still at the heart of care, but in recent years ongoing research has opened the door to broader questions about how regenerative medicine might support the biology of growth under certain clinical conditions.
UC-MSCs are being studied within this emerging field due to their immunomodulatory and trophic characteristics as well as their potential impact on cellular microenvironments. That said, warning in this jurisdiction is best done with reverence. Cell-based therapy for children’s height concerns are still supportive and investigational, not a routine or widely accepted mechanism for increasing one’s height.
The next generation of this field will only arise through responsible conduct of clinical research, meaningful pediatric oversight, and realistic discussions with families. Within this framework, Thailand itself is drawing interest as a platform from which regenerative medicine infrastructure and translational appetite may drive the next stage of scientific progress in pediatric growth treatment.

