Why This Topic Keeps Pulling So Much Attention
- Diabetes type 2 usually starts quietly
Type 2 diabetes doesn’t develop suddenly; it’s the result of long-term lifestyle habits. NIDDK notes that symptoms often develop slowly over several years and can be so mild that some people do not realize they have the disease until complications appear. This disease can be caused by a combination of factors, including insulin resistance, genetics, and beta-cell abnormalities. Which is why the condition often feels less like a single event and more like a gradual metabolic shift.
That slow, almost invisible progression is exactly why the phrase stem cell has become so magnetic in the diabetes world. Once people understand that type 2 diabetes is not only about “high sugar” but can also result from abnormal beta cells and malfunctioning metabolic control systems, they start looking beyond pills and insulin toward something that sounds more restorative. That is where stem cell research for diabetes type 2 starts to feel compelling: not as a trend word, but as a question about whether damaged insulin-producing systems can one day be biologically repaired.
What Stem Cell Actually Mean in Diabetes Research
- Stem cell is a platform, not one single treatment
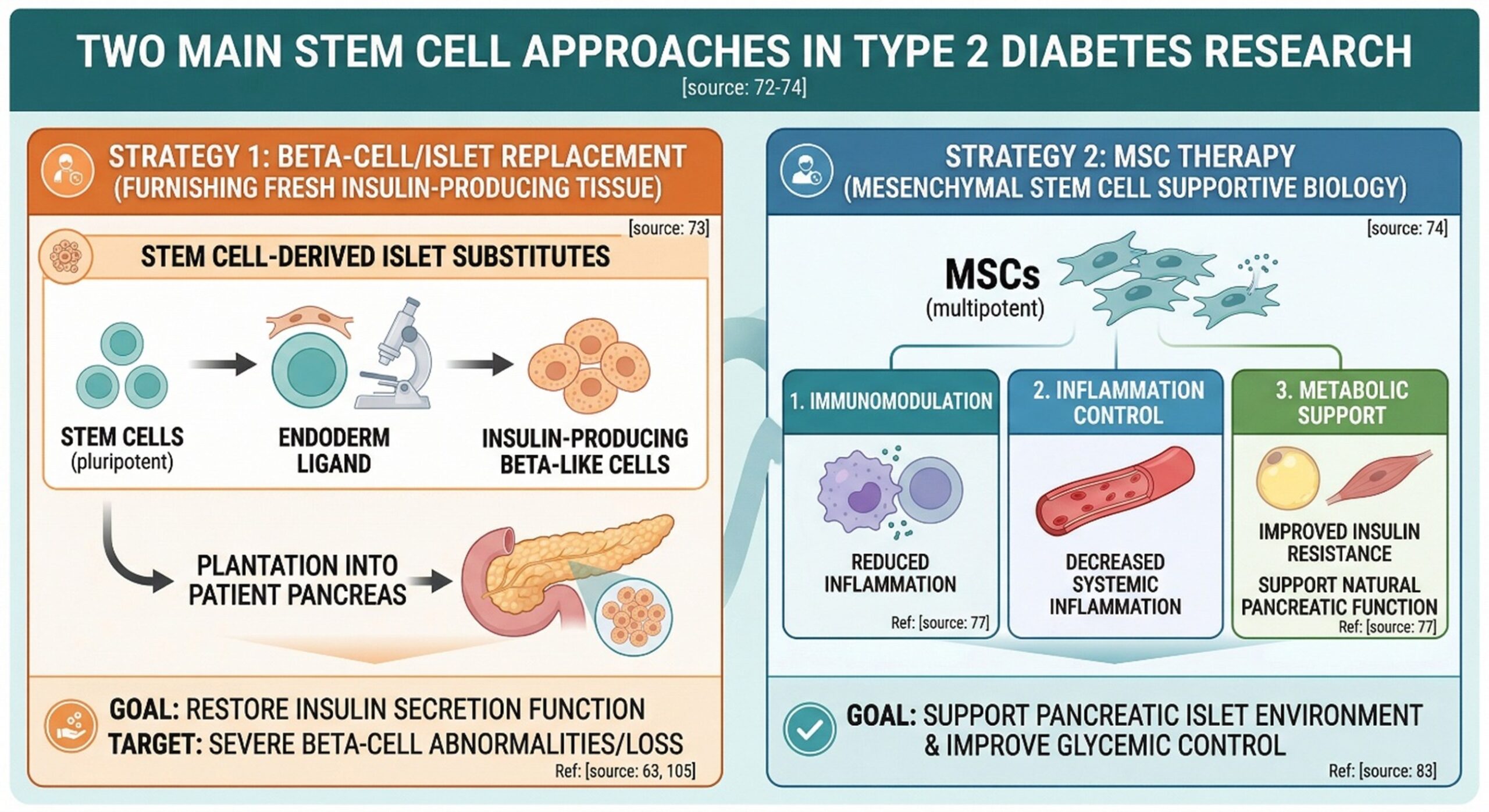
According to the NIH, they are significant in medical science because stem cells have both the capacity for self-renewal and development into diverse cell types; this is why scientists regard such material as being so important. In broad terms, this has fragmented into two major themes in diabetes research. One is stem cell-derived beta cell or islet substitutes, which researchers are currently working on to produce fresh insulin-producing tissue.
The other is MSC therapy (also known as “mesenchymal stem cell” therapy), which has been more studied as of late for its effects on immunomodulation, inflammation control, and metabolic support.
It makes a crucial difference because all too often diabetes type 2 developer’s research and treatment with stem cells is treated as if the problem were only one problem, when in fact that is simply not true. Some papers focus on replacing lost or defective beta cell ability; others look at whether MSCs can improve insulin resistance, reduce inflammation, and support natural pancreatic function as well. This is what makes it an exciting field to be in, but the reader must also be cautious not to conclude that every positive stem cell headline is tinged with the same biological color.
- The MSC story is getting stronger, but it is still not settled
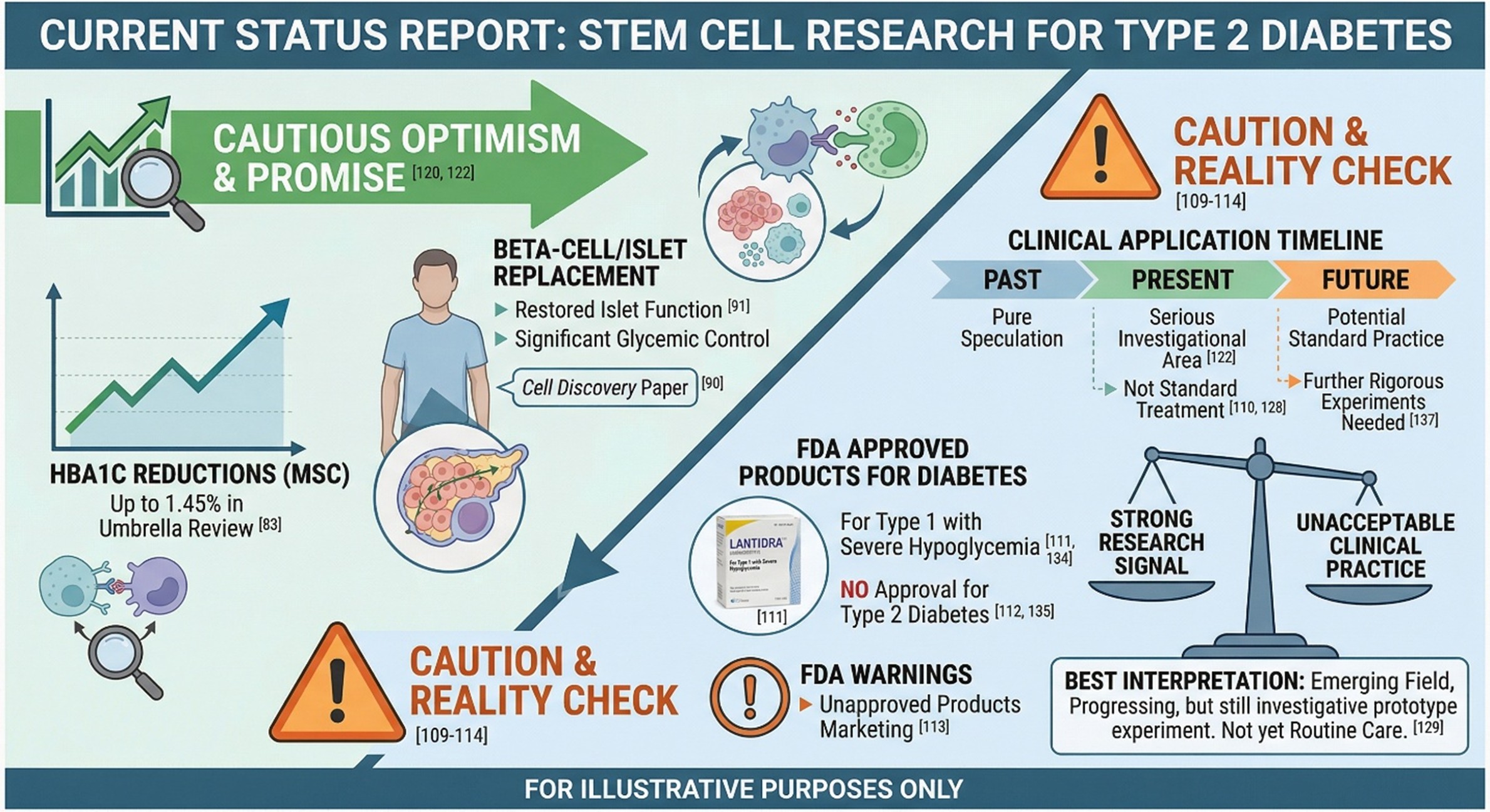
One of the most interesting developments in stem cell research for diabetes type 2 is the steady rise of MSC-based reviews. A 2025 review in Stem Cell Research & Therapy says MSC therapy for type 2 diabetes has mechanistic and clinical promise, but also emphasizes the need for standardized GMP-compliant production, predictive biomarkers, and robust randomized multicenter trials with long-term follow-up. Another 2025 umbrella review reported that MSC therapy showed meaningful improvements in glycemic control, particularly in type 2 diabetes, with HbA1c reductions of up to 1.45% and lower insulin requirements in some analyses.
That sounds impressive, and it is one reason stem cell and diabetes now make such a strong SEO pairing. But if you keep reading, the nuance becomes unavoidable. The same literature repeatedly highlights study heterogeneity: varying cell sources, doses, protocols, patient populations, and follow-up periods. A 2026 systematic review also found overall efficacy signals for diabetes stem cell therapy, but did not draw a simple “this now works routinely” conclusion. In other words, the direction is promising, but the field is still maturing.
- The beta-cell replacement story may be even more dramatic
If MSC therapy is the “supportive biology” side of the field, beta-cell replacement is the more futuristic side of stem cell research for diabetes type 2. A 2024 Cell Discovery paper reported the first-in-human use of autologous endoderm stem-cell-derived islet tissue as a tissue replacement therapy in a patient with type 2 diabetes and impaired islet function. The 27-month data showed significant improvements in glycemic control and provided early evidence that stem-cell-derived islet tissues may restore islet function in late-stage type 2 diabetes.
That paper matters because it changes the tone of the conversation. It suggests that stem cell science in type 2 diabetes is no longer only about laboratory models or hopeful theory. There are now human cases showing what a replacement strategy might look like in real life. But it is still a milestone case, not a routine therapy. A single striking study can move a field forward without automatically making it standard practice.
- Type 2 diabetes is more than insulin resistance
A lot of people still imagine type 2 diabetes as a disease of insulin resistance alone. But the research literature makes it clear that beta-cell decline is central to the story. NIDDK’s overview of type 2 diabetes points to insulin resistance as a key driver, while NIDDK’s diabetes research programs also focus heavily on pancreatic islet biology because insulin secretion failure is part of what drives the disease forward over time. That is exactly why stem cell research for diabetes type 2 is not just a side topic. It targets one of the deepest biological problems in the disease.
This is also what makes the field more interesting than a simple “better medication” story. If beta-cell dysfunction and beta-cell loss are part of disease progression, then stem-cell-derived islets, beta-cell engineering, and mesenchymal cell-based support are all attempts to change the biology underneath the glucose number, not just the number itself. That is why the papers feel so important even when they are cautious. They are not asking whether another drug lowers HbA1c. They are asking whether the pancreatic story itself can be rewritten.
What the Research Still Does Not Prove
- Promise is not the same as routine care
This is the part that honest articles cannot skip. The existence of strong stem cell research for diabetes type 2 does not mean stem cell therapy is now an established standard treatment for type 2 diabetes. FDA’s currently approved cellular therapy in diabetes, Lantidra, is for a specific group of adults with type 1 diabetes and repeated severe hypoglycemia despite intensive management. That approval is important, but it does not mean there is a broad FDA-approved stem cell therapy for type 2 diabetes.
The FDA has also warned companies for marketing unapproved stem cell products for serious conditions, including diabetes. That matters because the distance between published research and commercial claims can be large. A patient reading about stem cell and diabetes should understand that real progress in the literature does not automatically validate every clinic-level offer or broad treatment claim.
Why This Field Still Deserves Serious Attention
- The science is no longer fringe
Even with all the caution, it would be wrong to dismiss the field. Between the MSC umbrella reviews, the 2024 diabetes type 2islet replacement case, and the growing body of beta-cell engineering research, stem cell research for diabetes type 2 has clearly moved beyond pure speculation. There is now enough signal in the literature to justify serious interest from clinicians, researchers, and patients alike.
The most realistic conclusion is not that stem cell therapy has already solved diabetes. It is that the field is becoming too substantial to ignore. The papers are increasingly asking smarter questions, using stronger designs, and moving closer to the point where repair, replacement, and long-term metabolic restoration are not just abstract goals. That may not be a miracle headline, but it is the kind of progress that actually matters.
The FAQS are: Stem Cell, Diabetes, and Stem Cell Study to Treat Diabetes Type 2
- What is the primary goal of stem cell research diabetes type 2?
To improve MSC therapy, supporting cell therapies, and whether beta-cell or islet replacement strategies can restore insulin-producing function more directly.
- Is stem cell therapy already accepted clinical treatment for type 2 diabetes?
No, at this time. There are encouraging studies but this is still only categorized as investigative procedure introduced as a kind of prototype experiment and emerging trend instead of common practice.
- What makes stem cell research such a major topic in diabetes treatment?
Because the problem of type 2 diabetes is not only hyperglycemia but decline in beta cell function and metabolic balance. This has turned regenerative approaches into vivid anticipation.
- Anything to eat or drink now has been approved for diabetes?
Yes, but under specific circumstances. Lantidra was approved by the FDA for certain adults with type 2 diabetes who have repeated severe hypoglycemia despite intensive management. This is not the same as giving approval to treating type 2 diabetes with stem cells.
- What’s the most important thing to remember about stem cell research diabetes type 2?
That this is an emerging field as a matter of fact for now–with a history showing steady progress but still a long way from clinical application in humans and needing further rigorous and standardized experiments, following over the long term.

