Diabetes ulcers, especially that particularly foot ulcers are the most common and serious of its complications. These chronic wounds which affect almost a quarter of all diabetic patients over the course of their disease are also mainly what cause below the knee amputations. Although we have seen improvement in wound care we still see that healing is a very slow process or does not happen at all which is a result of poor blood flow, nerve damage, and immune deficiency. Umbilical cord derived mesenchymal stem cells (UC-MSC stem cells) put forth a very good solution to this issue by targeting the basic biological issues that cause wound not to close and also by stimulating tissue regeneration.
Pathophysiology of Diabetic Ulcers’ Healing Issues
Diabetes related ulcers which do not heal are a result of many related issues:.
- Peripheral neuropathy causes loss of protective sensation which in turn causes injuries to go unnoted.
- Impaired circulation of blood to the wound area.
- Prolonged inflammatory response breaks the normal healing process.
- High blood sugar levels impair immune response and fibroblast function.
These processes in total present a very poor environment for tissue repair which in turn makes standard treatments less effective.
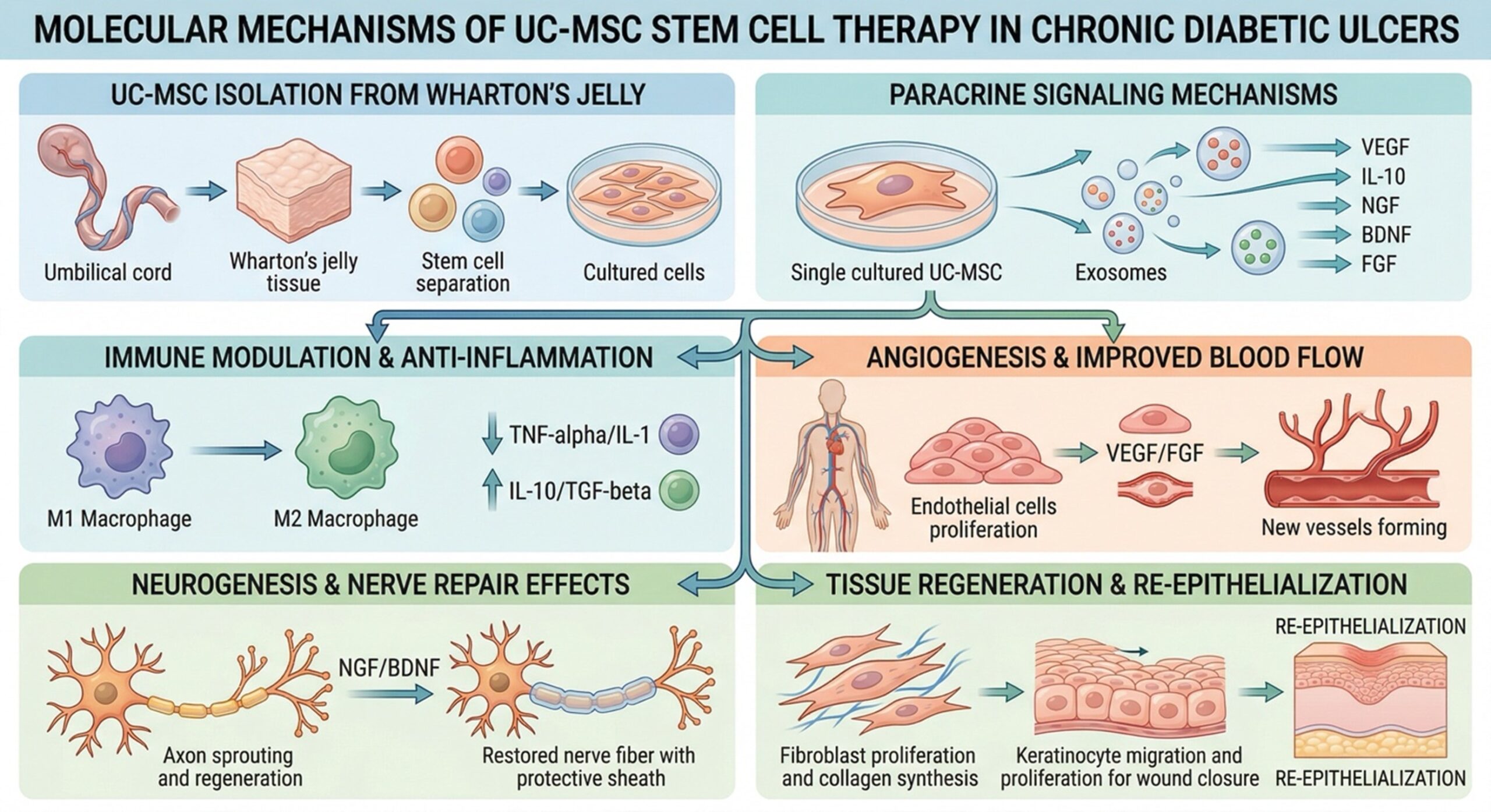
MSC Mechanism of Action: How UC-MSC cells Play a Role in Wound Healing
UC-MSC stem cells possess multiple therapeutic properties that are particularly suited to treating chronic wounds:
- UC-MSC stem cells produce growth factors such as VEGF which promote new capillary formation.
- Immunomodulation: They reduce levels of proinflammatory cytokines and modulate the immune response.
- Through paracrine action UC-MSC stem cells promote skin cell growth and also support tissue reconstruction.
- UC-MSC stem cells may put out peptides which in turn control infections.
- Recruitment of host cells: They play a role in bringing the patient’s own repair cells to the site of injury.
These complimentary processes create a healing oriented environment in ulcers which tend to not respond to treatment.
Delivery of UC-MSC stem cells into chronic wounds
UC-MSC stem cells may present as a number of different options for use in diabetic ulcer treatment:.
- Topical treatment with bio-compatible gels applied directly to the wound.
- Peri wound injections to augment adjacent tissue and blood flow.
- Advanced wound care products that include UC-MSC stem cells for sustained release.
Clinical Evidence: UC-MSC stem cells Outcomes in Diabetic Ulcers
Several clinical studies have demonstrated promising results:
- Patients treated with UC-MSC stem cells experienceaccelerated healing and smaller wound areas within a few weeks.
- Improved tissue granulationand quicker skin reformation have been noted.
- Cases showlower infection incidence and fewer amputations among treated individuals.
- Clinical trials confirm that UC-MSC stem cells arewell-tolerated with minimal to no adverse reactions.
These findings reinforce the potential of UC-MSC stem cells therapy to change diabetic wound care outcomes.
Benefits: Unique Advantages of UC-MSC Stem Cells Therapy
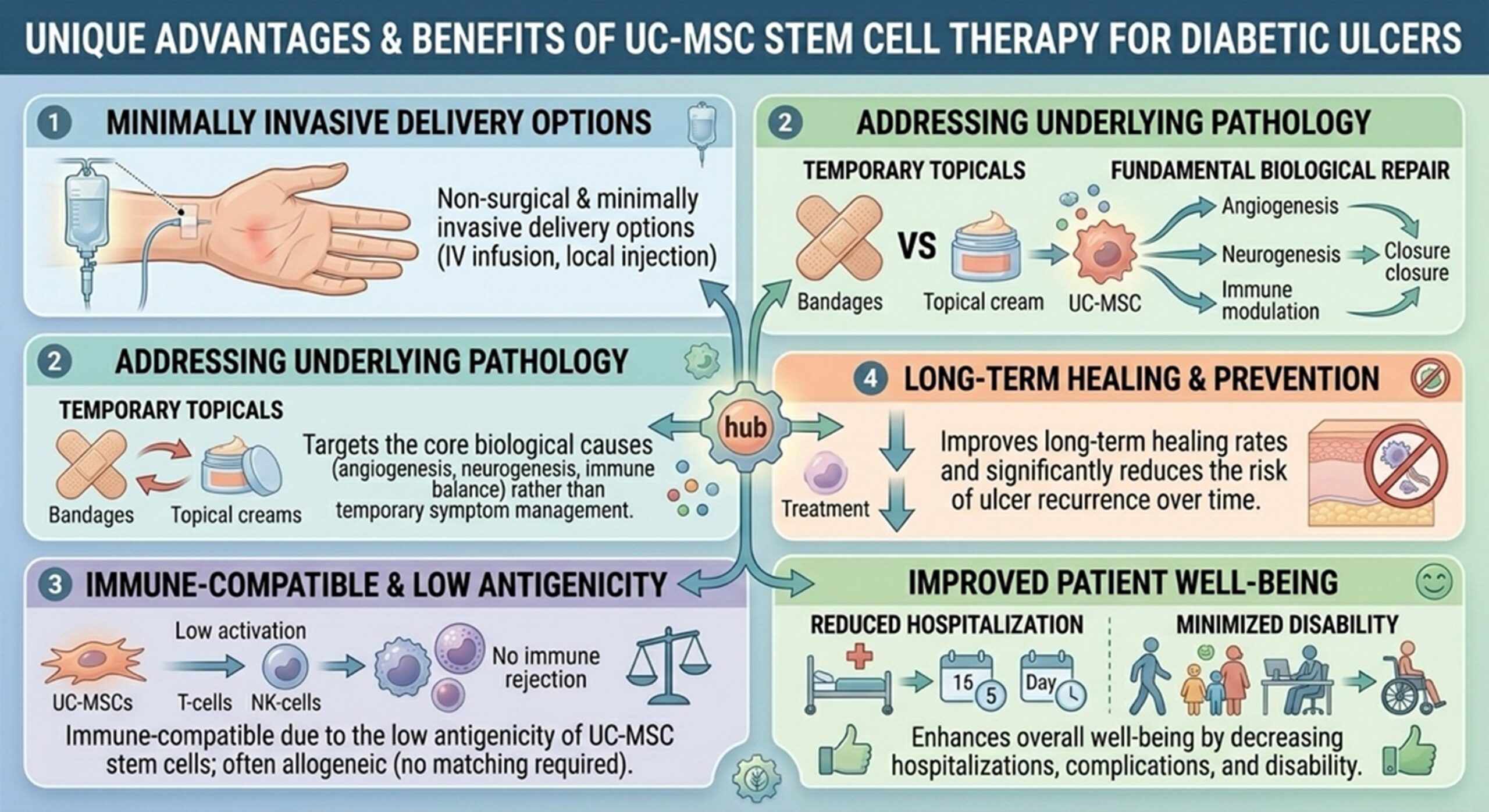
- Non-surgical and minimally invasivedelivery options.
- Addresses underlying pathologyrather than merely covering symptoms.
- Immune-compatibledue to the low antigenicity of UC-MSC stem cells.
- Long-term effectsin improving healing rates and preventing ulcer recurrence.
- Enhancement of patient well-beingby reducing hospitalization and disability.
Challenges: Hurdles to Widespread Adoption
While promising, several limitations must be acknowledged:
- High treatment costsand limited reimbursement.
- Variability in treatment protocolsacross clinical settings.
- Regulatory complexitiessurrounding cell-based therapies.
- Differences in patient healthand ulcer conditions may influence success.
- Insufficient long-term datato assess sustained healing and recurrence.
Future Directions: Evolving the Role of UC-MSC Stem Cells
Research and innovation are driving further improvements in this field:
- Customized treatmentsbased on patient-specific needs.
- Genetic enhancementsto boost UC-MSC regenerative capacity.
- Smart biomaterialsfor adaptive cell delivery.
- Therapeutic combinations, such as using UC-MSC stem cells with oxygen therapy or antibiotics.
- Broader clinical trialsto establish guidelines for mainstream use.
Conclusion: Transforming Diabetic Wound Care
UC –MSC stem cell therapy is a new approach which we see in the management of diabetic ulcers which overcomes key issues related to healing. We see with their regenerative and anti inflammatory properties that UC –MSC stem cells do in fact greatly improve wound repair and also prevent issues like amputation. As we see more clinical data and technology improve in this field UC–MSC stem cells are to become a game changer in diabetic wound care.

