Parkinson’s disease is a long-term and progressive neurological condition that primarily affects movement. It develops as dopamine-producing neurons in a specific region of the brain gradually deteriorate. Dopamine is a critical neurotransmitter responsible for coordinating smooth and controlled muscle activity. As these neurons decline, individuals begin to experience symptoms such as tremors, muscle rigidity, slowed movements, and impaired balance. Over time, these symptoms can worsen, significantly affecting independence and overall quality of life.
Conventional treatments for Parkinson’s disease are mainly designed to manage symptoms rather than cure the condition. Medications such as Levodopa are commonly used to replenish dopamine levels in the brain, helping to improve movement-related symptoms. However, these treatments do not stop the ongoing degeneration of neurons. As the disease progresses, their effectiveness may diminish, and patients may experience fluctuations in symptom control. This highlights the need for therapies that can address the underlying causes of neuronal loss.
In recent years, regenerative medicine has introduced stem cell therapy as a potential breakthrough in the treatment of neurodegenerative disorders. Unlike traditional approaches, stem cell-based therapies aim to repair or replace damaged cells and restore normal function. In Parkinson’s disease, this strategy focuses on replenishing lost dopamine-producing neurons, protecting those that remain, and improving the overall brain environment. This approach offers hope for slowing disease progression and possibly reversing some of its effects.
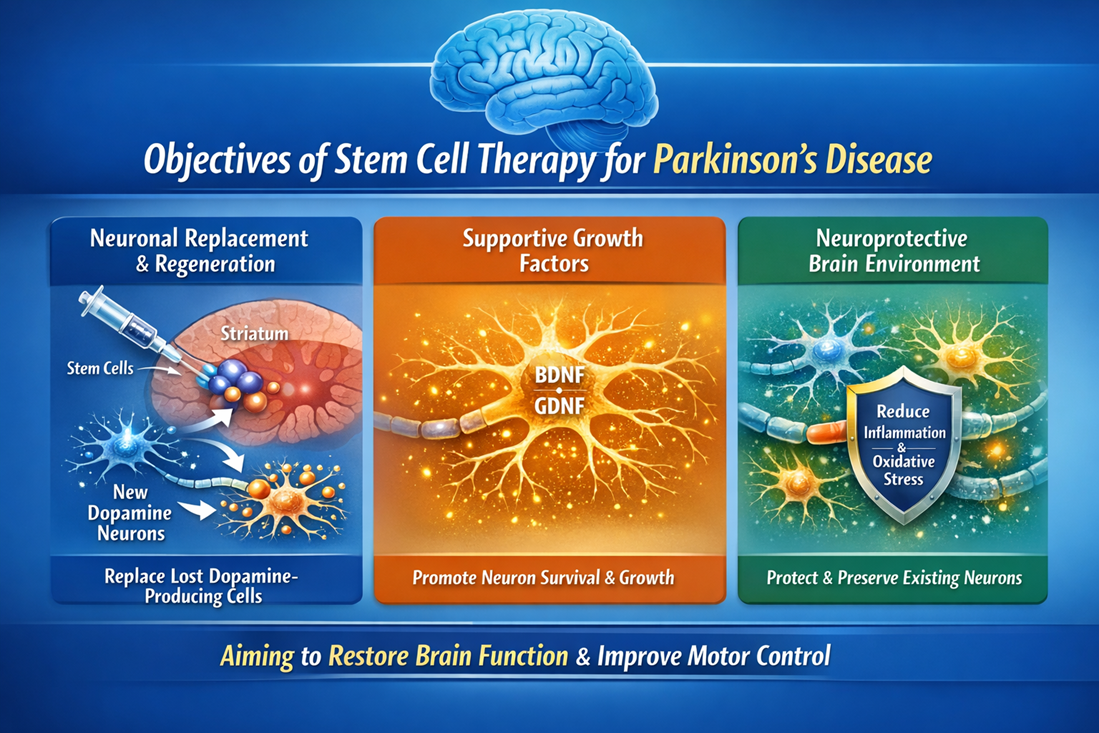
Objectives of Stem Cell Therapy for Parkinson’s Disease
Neuronal Replacement and Regeneration Strategies
One of the main objectives of stem cell therapy in Parkinson’s disease is to replace the neurons that have been lost. This can be achieved by introducing specialized precursor cells, such as neural stem cells or dopaminergic progenitors, into affected areas of the brain. Regions like the striatum or substantia nigra are often targeted because they play key roles in movement control. Once transplanted, these cells have the potential to mature into functional dopamine-producing neurons, helping to restore neurotransmitter balance and improve motor function.
In addition to replacing damaged cells, stem cells can provide significant supportive benefits through the release of growth factors. These include important molecules such as Brain-Derived Neurotrophic Factor and Glial Cell Line-Derived Neurotrophic Factor. These substances play a crucial role in maintaining neuron health by promoting cell survival, encouraging growth, and enhancing connections between nerve cells. By strengthening the neural network, they help remaining neurons function more effectively and resist further degeneration.
Creating a Neuroprotective Brain Environment
The brain environment in individuals with Parkinson’s disease is often affected by chronic inflammation and oxidative stress, both of which contribute to neuronal damage. Certain stem cells have the ability to counteract these harmful conditions. They can reduce inflammatory signals and neutralize reactive oxygen species, creating a more supportive and less toxic environment. This neuroprotective effect helps preserve existing neurons and enhances the overall conditions needed for brain repair and recovery.
Approaches for Delivering Stem Cells in The Treatment of Parkinson’s Disease
Direct Transplantation Techniques for Targeted Therapy: Delivering stem cells directly into the brain is one of the most precise methods of treatment. In this approach, cells are surgically implanted into specific regions affected by Parkinson’s disease, such as the substantia nigra or striatum. This targeted delivery allows for accurate placement of cells, increasing the likelihood that they will integrate effectively and perform their intended function. However, because it involves surgery, this method requires careful consideration of potential risks and benefits.
Intravenous Delivery as a Minimally Invasive Option: Another method of administering stem cells is through intravenous infusion. In this technique, stem cells are introduced into the bloodstream and circulate throughout the body. Some of these cells may reach the brain and exert beneficial effects. Although this approach is less invasive and easier to perform, it is generally less efficient in delivering cells directly to the areas most affected by Parkinson’s disease. Nevertheless, it may still provide systemic benefits, particularly through anti-inflammatory and immunomodulatory actions.
Scaffold-Based Approaches for Enhanced Cell Integration: Innovative strategies such as scaffold-assisted implantation are being developed to improve the success of stem cell therapy. In this method, biocompatible materials are used to support the survival and growth of transplanted cells. These scaffolds provide a stable environment that helps cells integrate into existing brain tissue. By enhancing cell survival and function, scaffold-based approaches may improve the overall effectiveness of treatment.
Advances in Genetic Engineering and Cell Optimization
To increase the effectiveness of stem cell therapies, researchers are exploring genetic modification techniques. By altering stem cells to produce more dopamine or resist harmful conditions, scientists aim to enhance their therapeutic potential. These engineered cells may be better equipped to survive in the challenging environment of a Parkinson’s-affected brain and provide more consistent benefits over time.
Future Potential of Stem Cell Therapy in Parkinson’s Disease
Stem cell therapy represents a promising and evolving frontier in the treatment of Parkinson’s disease. By targeting the root cause of the condition—dopamine neuron loss—this approach has the potential to go beyond symptom relief and achieve meaningful restoration of function. Whether through neuron replacement, neuroprotection, or environmental improvement, stem cells offer multiple pathways for therapeutic benefit.
Conclusion: Toward Regenerative and Personalized Care
The development of stem cell-based therapies marks a significant shift in how Parkinson’s disease may be treated in the future. By focusing on regeneration and repair, this approach offers hope for slowing disease progression, improving motor function, and enhancing quality of life. As research continues to advance, particularly in areas such as patient-specific induced pluripotent stem cells and combination therapies, stem cell treatment may become a key component of personalized medicine. While further studies are necessary to confirm long-term safety and effectiveness, the potential of this innovative therapy continues to grow, offering new possibilities for individuals living with Parkinson’s disease.

