Novel Therapeutic Frontiers for Parkinson’s Disease in Stem Cell Therapy Thailand
Parkinson’s Disease represents one of the most debilitating neurological conditions facing the aging population today. Characterized by the progressive loss of dopaminergic neurons in the substantia nigra, this condition leads to a catastrophic decline in motor control and cognitive function. The severity of the disease often robs individuals of their independence, creating a heavy emotional and financial burden on families. While pharmaceutical interventions have existed for decades, they often fail to address the underlying cellular death, merely masking symptoms temporarily. This limitation has catalyzed the search for regenerative solutions, specifically Stem Cell Therapy Thailand, to provide a more permanent biological repair mechanism that goes beyond traditional chemical supplementation. The urgency for such innovation is underscored by the rising global prevalence of the disorder, necessitating a shift toward cellular-based interventions that can actually alter the disease’s natural history.
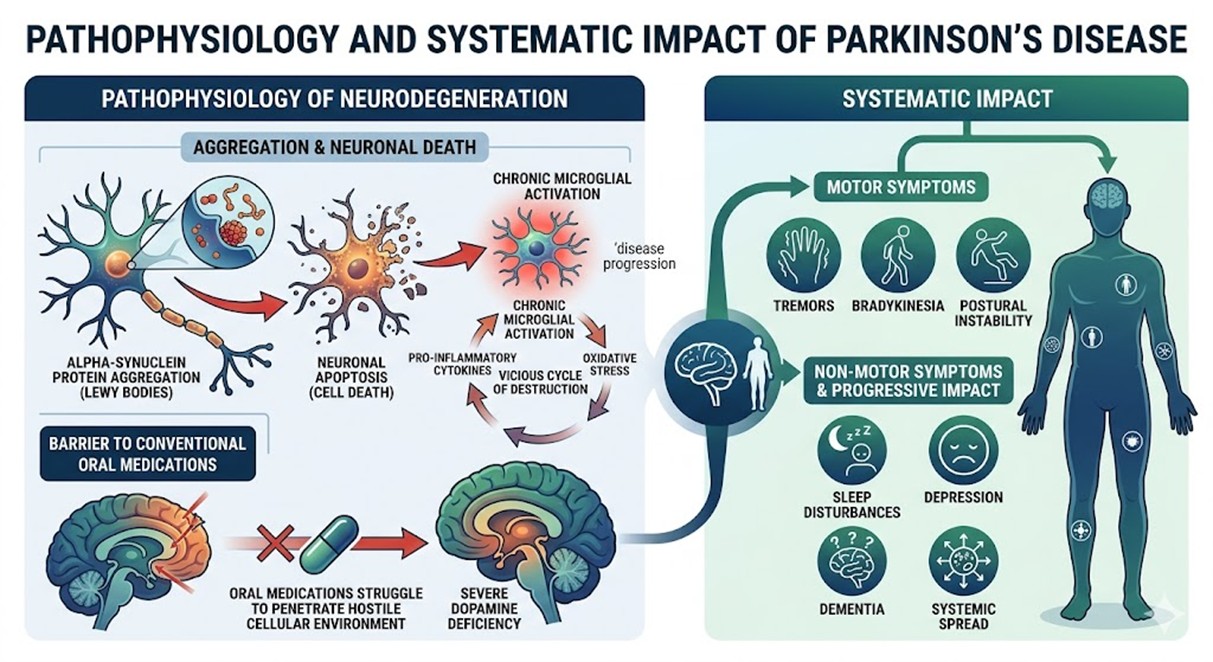
- Pathophysiology and Systematic Impact of Parkinson’ Disease
The mechanism of Parkinson’ Disease is rooted in the aggregation of alpha-synuclein proteins, which form toxic Lewy bodies within the brain. These aggregates trigger chronic neuroinflammation and oxidative stress, leading to the apoptosis of vital neurons. As these cells perish, the brain’s ability to produce dopamine—a neurotransmitter essential for smooth movement—is severely compromised. Patients typically experience tremors, bradykinesia, and postural instability. Beyond motor symptoms, the impact on life includes sleep disturbances, depression, and dementia, which progressively worsen as the neurodegenerative process spreads to other regions of the central nervous system. The cellular environment becomes increasingly hostile as microglial cells remain in a chronically activated state, releasing pro-inflammatory cytokines that further accelerate the destruction of neighboring healthy tissues. This vicious cycle of neuroinflammation and oxidative damage creates a physiological barrier that conventional oral medications simply cannot penetrate effectively.
- Limitations of Conventional Parkinson’ Disease Management
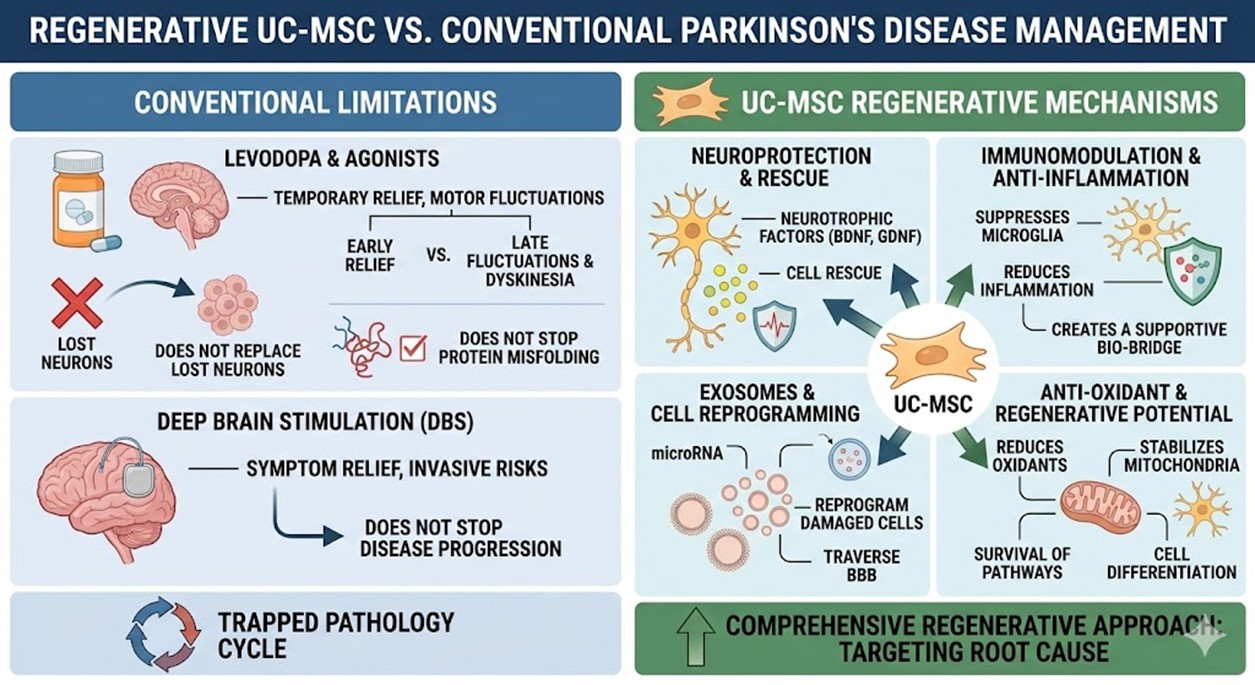
Current Parkinson’ Disease management primarily relies on Levodopa or dopamine agonists to replenish declining neurotransmitter levels. While effective in the early phase of the disease, these medications frequently lead to motor fluctuations and debilitating dyskinesia over time. Surgical options like Deep Brain Stimulation offer symptomatic relief for some but involve invasive procedures with inherent risks and do not stop the disease’s progression. The primary constraint of these traditional paths is their inability to replace lost neurons or alter the toxic environment of the brain. Patients often find themselves trapped in a cycle of increasing dosage and diminishing returns, where the side effects of the medication eventually become as burdensome as the disease itself. Furthermore, these Parkinson’ Disease methods do nothing to address the protein misfolding or the underlying inflammatory cascade, leaving the root cause of the neurodegeneration untouched and allowing the pathology to advance unchecked.
- Therapeutic Mechanisms of UC-MSCs Stem Cell Therapy Thailand
Umbilical Cord-derived Mesenchymal Stem Cells (UC-MSCs) have emerged as a superior alternative in the field of Stem Cell Therapy Thailand due to their unique immunomodulatory and neuroprotective properties. Unlike other cell types, UC-MSCs secrete a potent array of neurotrophic factors such as Brain-Derived Neurotrophic Factor (BDNF) and Glial Cell Line-Derived Neurotrophic Factor (GDNF). These factors work to rescue struggling neurons and stimulate endogenous repair. Furthermore, the mechanism involves the suppression of overactive microglia, which reduces the chronic inflammation that drives neuronal death. By modulating the cytokine environment, UC-MSCs create a bio-bridge that supports the survival of existing dopaminergic pathways while potentially differentiating into neural-like cells under specific microenvironmental cues.
The deep cellular mechanism involves the secretion of extracellular vesicles or exosomes that contain specialized microRNA. These tiny messengers travel through the blood-brain barrier to deliver genetic material that can reprogram damaged cells and inhibit the apoptotic pathways triggered by alpha-synuclein toxicity. By reducing the presence of reactive oxygen species and stabilizing the mitochondrial function within remaining neurons, UC-MSCs provide a comprehensive biological shield. This multifaceted approach targets the root causes of neurodegeneration rather than just the outward symptoms, offering a regenerative potential that was previously thought impossible in adult neurology. This is why Stem Cell Therapy Thailand is becoming a focal point for international patients seeking more than just chemical management of their condition.
- Future Outlook for MSCs in the Thai Medical Landscape
The trajectory of MSC research for Parkinson’s Disease is exceptionally promising in Thailand. The nation has positioned itself as a global leader in regenerative medicine through sophisticated laboratory infrastructure and supportive regulatory frameworks. By choosing Stem Cell Therapy Thailand, patients access cutting-edge protocols that integrate UC-MSC transplantation with holistic rehabilitative care.
This decision is driven by high standards in cell processing and advanced cultivation techniques ensuring cell potency. As clinical trials demonstrate safety and efficacy, the integration of MSCs into routine neurological care is expanding. This growth is supported by a robust ecosystem of specialized clinics focusing on the quality of life for aging populations. The future of Thai medicine emphasizes a personalized approach, making Stem Cell Therapy Thailand a beacon of hope for those seeking to halt Parkinson’s Disease progression through advanced biological intervention.
In summary, the transition from symptom management to regenerative repair marks a significant turning point in the fight against Parkinson’ Disease. The integration of UC-MSCs offers a sophisticated biological strategy to combat neuroinflammation and promote neuronal health. By addressing the cellular environment and providing neurotrophic support, this therapy moves beyond the limitations of traditional pharmacology. With its advanced facilities and specialized expertise, Thailand remains at the forefront of this medical revolution. The synergy between scientific innovation and clinical application ensures that patients receive the most advanced care possible. By focusing on the deep cellular mechanisms of repair, Stem Cell Therapy Thailand provides a viable path forward for improving the quality of life and restoring hope to those affected by this complex neurodegenerative disorder.

