A well-functioning metabolism depends on multiple organs working in coordination to produce energy, manage nutrient storage, regulate hormones, and control inflammatory activity. When these systems remain in balance, the body is better able to maintain steady blood sugar, regulate fat metabolism, and turn food into energy effectively.
As regenerative medicine continues to develop, researchers are exploring new ways to promote metabolic wellness at the cellular level. One area receiving growing attention is the use of umbilical cord–derived mesenchymal stem cells (UC-MSCs). These cells are of interest because they can secrete biologically active molecules, influence immune responses, and assist natural repair processes. For this reason, stem cell–based strategies are being investigated as supportive approaches that may contribute to metabolic balance and general health.
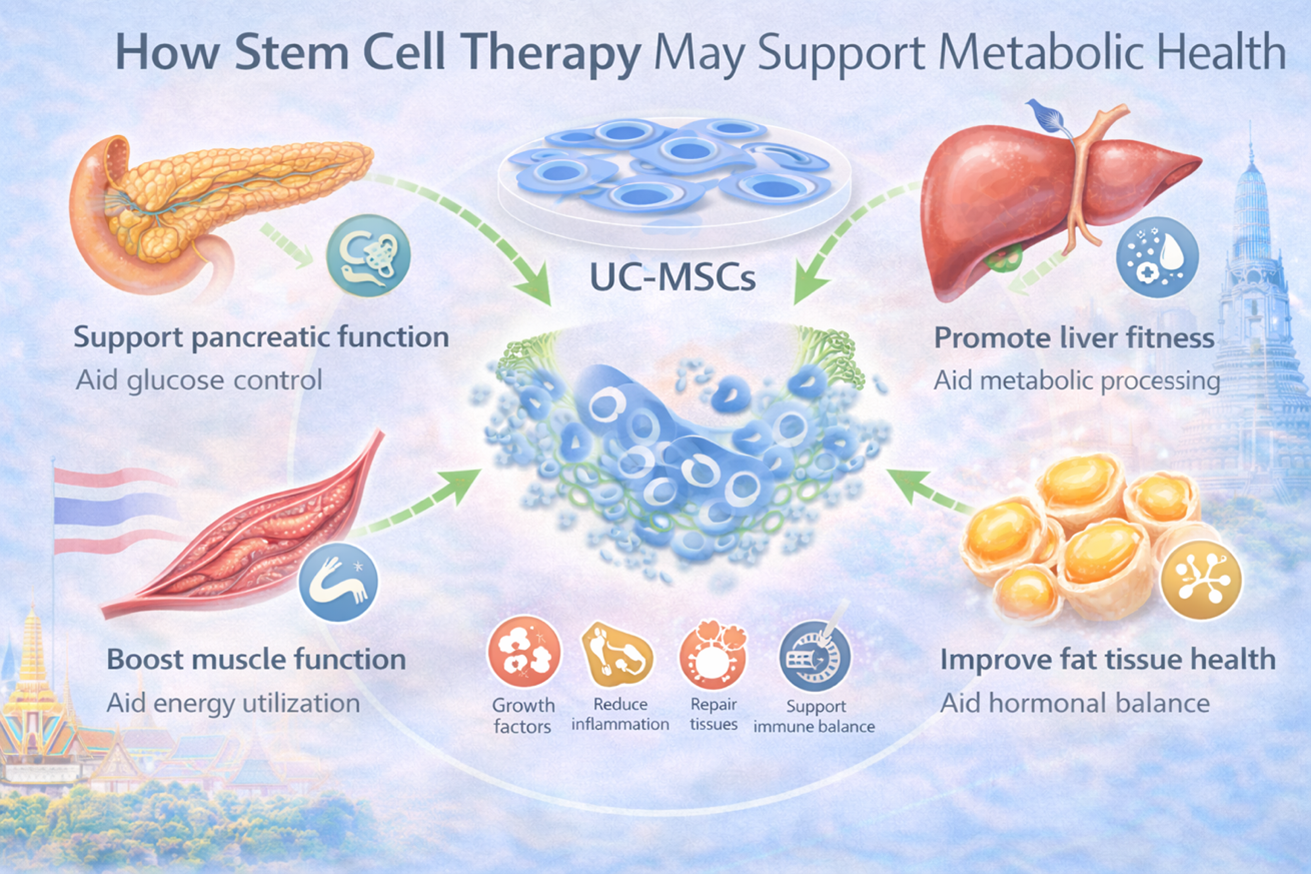
Supporting the Pancreas and Blood Sugar Balance
In disorders involving metabolism, such as diabetes, the insulin-producing beta cells of the pancreas may decline in number or lose function. When this happens, the body may not produce enough insulin to meet its needs, which can result in persistently high glucose levels.
UC-MSC–based therapy is being examined for its potential to help protect pancreatic tissue by lowering localized inflammation and releasing signaling molecules that may support cell survival and recovery. Some studies also look at whether these effects may help preserve insulin-related function. By helping maintain pancreatic health, this approach may contribute to improved glucose balance and potentially reduce the risk of long-term metabolic complications.
Encouraging Liver Recovery and Better Metabolic Processing
The liver is essential for controlling blood sugar, processing fats, and regulating many hormones linked to metabolism. When liver function is impaired by conditions such as fatty liver disease or fibrosis, these metabolic processes may become less efficient.
UC-MSCs may help create conditions that are more favorable for liver healing by reducing inflammatory stress, limiting scar formation, and supporting regenerative responses. Improved liver health may help the body process nutrients more effectively, better regulate cholesterol, and maintain a healthier metabolic state overall.
Helping Muscle Tissue Use Energy More Efficiently
Skeletal muscle is a major site for glucose uptake and fatty acid utilization. When muscle quality or function declines, insulin responsiveness and energy use can also worsen.
UC-MSCs may assist muscle recovery by releasing factors that stimulate repair pathways and support the activity of satellite cells, which are involved in maintaining and rebuilding muscle fibers. Stronger and healthier muscle tissue may improve the body’s ability to use glucose efficiently and support better metabolic performance over time.
Supporting Healthier Fat Tissue Activity
Fat tissue does more than store excess energy. It also plays an active role in hormone signaling and inflammatory regulation. When adipose tissue becomes dysfunctional, it can contribute to insulin resistance and broader metabolic disruption.
UC-MSCs may help improve the condition of fat tissue by calming inflammation, promoting healthier tissue remodeling, and supporting circulation within adipose areas. These actions may help maintain a better balance between storing fat and breaking it down, which can support overall metabolic stability.
Promoting Better Insulin Responsiveness
The body’s response to insulin depends on tissues being able to receive and act on insulin signals correctly. Ongoing inflammation can disrupt these pathways and reduce metabolic efficiency.
Because UC-MSCs are being studied for their anti-inflammatory and immune-regulating properties, they may help preserve insulin signaling while also supporting tissue repair. Together, these effects may improve how the body handles and uses glucose.
Lowering Inflammation and Improving Immune Regulation
One of the most studied features of UC-MSCs is their ability to interact with the immune system. They can release substances that help reduce excessive inflammation while also supporting healing and cellular recovery.
Since chronic low-level inflammation is closely associated with many metabolic disorders, reducing this inflammatory burden may help protect important metabolic organs and improve overall metabolic control.
Supporting Energy Regulation Over Time
A healthy metabolism also depends on the body’s ability to adapt to different demands, including changes in diet, physical activity, and stress. This adaptability is often referred to as metabolic flexibility.
UC-MSCs may help support this capacity by helping preserve the health and repair potential of tissues involved in energy balance. Through their signaling effects and support of regenerative processes, these therapies are being explored for their possible role in maintaining more stable energy regulation over the long term.
Conclusion
Umbilical cord–derived mesenchymal stem cells are becoming an area of increasing interest in the field of metabolic support. By helping regulate inflammation, encouraging tissue recovery, and improving communication between cells, UC-MSC–based approaches may offer supportive benefits for important metabolic organs such as the pancreas, liver, muscle, and adipose tissue.
Although this area of research is still developing, stem cell–based strategies are being studied for their potential to support insulin sensitivity, blood sugar control, and broader metabolic function, with the aim of promoting better long-term health and wellness.

