Chronic ulcerative wounds—such as diabetic foot ulcers, venous leg ulcers, pressure ulcers, and ulcers related to vascular disease—are persistent medical problems that affect millions of individuals worldwide. Traditional wound care methods—including debridement, wound dressings, antibiotics, and pressure management—play an important role in treating ulcers. In recent years, regenerative medicine has introduced a promising solution: stem cell therapy. Among the most widely studied options are umbilical cord–derived mesenchymal stem cells (UC-MSCs), which have shown remarkable potential in enhancing tissue repair and accelerating wound recovery.
The Role of Stem Cells in Regenerative Healing
In wound healing, stem cells contribute in two primary ways. First, they can differentiate into specialized cells required for rebuilding damaged tissues, such as skin cells, connective tissue cells, and blood vessel cells. Second, stem cells release a wide range of signaling molecules that influence surrounding cells and stimulate the healing process.
UC-MSC stem cells have gained significant attention because they are relatively easy to obtain, exhibit strong regenerative properties, and have demonstrated a favorable safety profile in many clinical studies.
Mechanisms Behind Stem Cell–Mediated Ulcer Repair
Stem cell therapy improves wound repair through several complementary biological mechanisms.
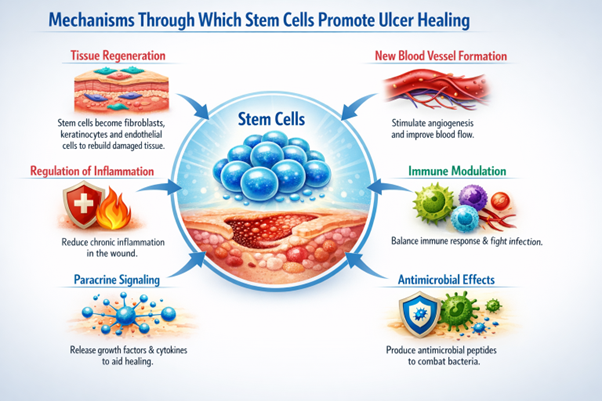
One of the most important effects is tissue regeneration. Mesenchymal stem cells can transform into cells needed for rebuilding damaged structures within the wound. These include fibroblasts that produce connective tissue, keratinocytes that form the outer skin layer, and endothelial cells that create new blood vessels.
Another critical mechanism is angiogenesis, the formation of new blood vessels. Chronic ulcers often suffer from poor circulation, which deprives tissues of oxygen and nutrients. Stem cells release growth factors, including vascular endothelial growth factor (VEGF), which stimulate the development of new capillaries. Improved circulation enhances oxygen delivery and supports faster tissue repair.
Stem cells also help regulate inflammation. Chronic wounds typically remain stuck in a prolonged inflammatory state that prevents normal healing. Mesenchymal stem cells produce anti-inflammatory molecules that help shift the wound environment from inflammation toward regeneration. This balanced immune response allows damaged tissues to rebuild more effectively.
In addition, stem cells interact with immune cells such as macrophages and T lymphocytes. These interactions help regulate immune activity, enabling the body to fight infection while preventing excessive inflammatory damage.
Another major benefit comes from paracrine signaling. Stem cells release numerous bioactive molecules—including cytokines, chemokines, and growth factors—that stimulate nearby cells to migrate, divide, and participate in the repair process. Even if stem cells do not directly become new tissue, these signals activate the body’s own healing capacity.
Some research also suggests that mesenchymal stem cells produce antimicrobial peptides, which may help limit bacterial growth within the wound. This potential antibacterial effect can further support the healing process.
Advantages of Stem Cell–Based Ulcer Treatment
Regenerative stem cell therapy offers several potential advantages compared with conventional treatments. One of the most significant benefits is the ability to promote full-thickness tissue repair rather than simply closing the wound surface. This means the therapy supports the restoration of deeper skin layers and underlying structures.
Stem cell therapy may also reduce scarring. By guiding tissue formation in a more organized manner, it can help produce skin that more closely resembles normal tissue.
Faster healing is another major advantage. Accelerated wound closure reduces the risk of infection and other complications that commonly occur in chronic ulcers. In addition, regenerated tissue tends to be stronger and more resilient, which may decrease the likelihood of future wound recurrence.
Perhaps most importantly, effective treatment of severe ulcers can reduce the need for limb amputation. By restoring circulation, repairing tissues, and improving immune responses, stem cell therapy offers hope for preserving both limb function and quality of life.
Future Perspectives in Regenerative Wound Care
Advances in biotechnology continue to expand the possibilities of stem cell therapy for chronic wounds. Researchers are developing innovative approaches such as 3D-printed skin grafts that incorporate stem cells and growth factors tailored to the patient’s wound dimensions.
Smart wound dressings are another emerging technology. These materials can monitor environmental changes—such as pH levels, temperature, or infection markers—and release therapeutic substances when needed.
Scientists are also exploring genetically modified stem cells that produce higher levels of healing proteins or survive better in low-oxygen environments typical of chronic wounds. Additionally, exosome-based therapies derived from stem cells are being investigated as a cell-free alternative that may deliver regenerative signals without requiring living cells.
Conclusion
Stem cell therapy offers a significant breakthrough in managing and treating chronic ulcers. By addressing the underlying biological deficiencies that prevent wounds from healing, this regenerative approach moves beyond symptom management and focuses on true tissue restoration. Through mechanisms such as tissue regeneration, improved blood vessel formation, inflammation control, and immune regulation, stem cells offer a powerful tool for repairing damaged skin and supporting long-term recovery.
As clinical research continues and new technologies emerge, regenerative therapies like UC-MSC stem cell treatment may become an increasingly important component of modern wound care. With the potential to accelerate healing, prevent complications, and preserve limb function, stem cell therapy holds great promise for improving the lives of patients suffering from chronic ulcerative wounds.

