Wound healing is a complex biological process that allows the body to restore damaged skin and underlying tissues following injury. This natural repair mechanism occurs through several coordinated stages, including inflammation, tissue formation, and structural remodeling. While most minor wounds heal efficiently, certain injuries—such as diabetic ulcers, pressure sores, and severe burns—can be far more difficult to treat. These complicated wounds often heal slowly or fail to heal completely, increasing the risk of infection, chronic pain, and long-term health complications that significantly affect a patient’s quality of life.
In recent years, regenerative medicine has introduced innovative therapeutic strategies to address these difficult cases. Among the most promising approaches is stem cell therapy, particularly the use of umbilical cord–derived mesenchymal stem cells (UC-MSCs). These specialized cells possess unique regenerative properties that allow them to support tissue repair in multiple ways. UC-MSC stem cells can transform into different cell types, release bioactive molecules that promote healing, regulate inflammation, and stimulate the formation of new blood vessels. Because of these capabilities, stem cell–based therapies are gaining attention as a powerful tool for managing chronic wounds and improving recovery outcomes.
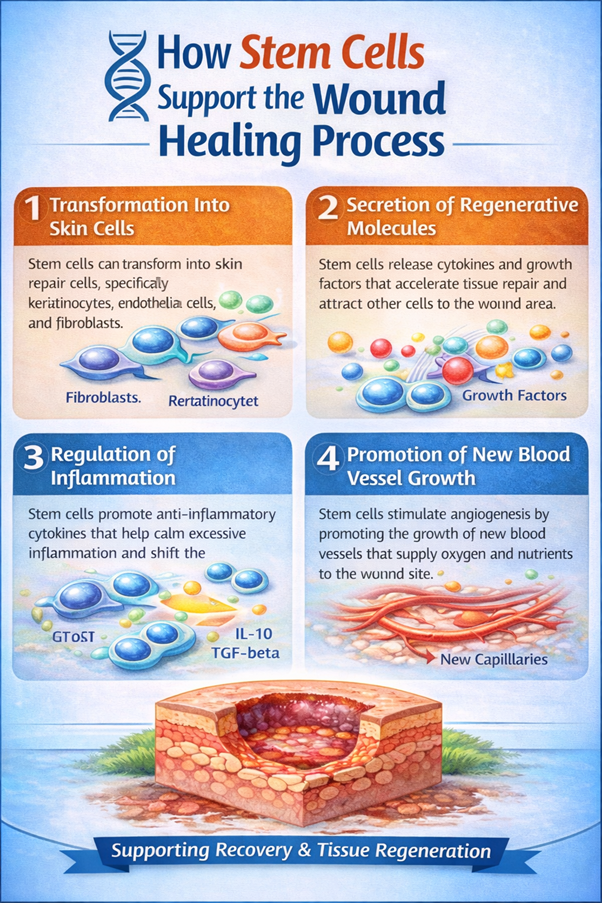
How Stem Cells Support the Wound Healing Process
- Transformation Into Skin Cells: When applied to injured skin, stem cells can differentiate into keratinocytes and fibroblasts. Keratinocytes form the protective outer layer of the skin, while fibroblasts produce structural components such as collagen and extracellular matrix proteins. Stem cells replace damaged tissue with new, functional cells. The regenerated tissue helps rebuild the skin’s protective barrier and restores its normal structure and elasticity.
- Secretion of Regenerative Molecules: Beyond directly replacing damaged cells, stem cells also influence healing through the release of therapeutic signaling molecules. This mechanism, commonly referred to as paracrine signaling, involves the secretion of growth factors, cytokines, and other biologically active compounds.
These substances help guide surrounding cells to the wound site, stimulate the production of collagen, and encourage tissue regeneration. Important signaling molecules released by stem cells can activate nearby skin cells and immune cells, creating an environment that supports faster and more effective wound closure. In addition, these molecules assist in coordinating communication between cells, which is essential for organized tissue repair.
- Regulation of Inflammation: Stem cells help maintain a healthy balance within the immune system. They can suppress harmful inflammatory responses while encouraging anti-inflammatory pathways that promote tissue rebuilding. By modulating immune activity, stem cells support a smoother progression from the inflammatory phase of healing to the stages of tissue formation and remodeling.
- Promotion of New Blood Vessel Growth: Adequate blood supply is critical for successful wound healing because oxygen and nutrients must reach the injured tissue. Stem cells play an important role in angiogenesis, the formation of new blood vessels.
Through the release of vascular growth factors, stem cells stimulate the development of additional blood vessels around the wound area. Improved circulation enhances the delivery of oxygen, nutrients, and immune cells, all of which are necessary for tissue regeneration. Enhanced vascularization also helps reduce the likelihood of complications such as infection or tissue death, particularly in wounds with poor circulation.
Medical Applications of Stem Cell Therapy in Wound Care
- Treatment of Chronic Wounds: Stem cell therapy offers a regenerative approach for these conditions. By introducing stem cells directly into the affected area, physicians can stimulate tissue regeneration and improve the local healing environment. The therapy helps increase blood flow, reduce inflammation, and encourage the formation of new skin tissue, leading to improved healing rates in wounds that previously resisted treatment.
- Recovery From Burn Injuries: Stem cells can significantly enhance recovery following burn injuries. They support the development of new skin layers and assist in reconstructing the damaged tissue matrix. As a result, healing can occur more rapidly, and the regenerated skin often shows improved flexibility and strength. Additionally, stem cell therapy may help reduce the formation of thick scars and contractures that can limit mobility.
- Improving Surgical Wound Healing: Stem cell therapy can support recovery by enhancing collagen production, improving tissue regeneration, and reducing inflammation at the surgical site. These effects help wounds close more quickly and decrease the risk of complications. In some cases, stem cell–based treatments may also shorten the overall recovery period.
- Reducing Scarring and Enhancing Cosmetic Outcomes: Stem cells show potential in improving the appearance and texture of healed skin. They influence collagen remodeling and help reorganize the tissue structure within the healing wound. This process may lead to smoother skin, improved pigmentation balance, and less prominent scar tissue. Because of these benefits, stem cell therapy is becoming increasingly relevant in both reconstructive surgery and cosmetic dermatology.
Benefits of Stem Cell-Based Wound Treatments
Stem cell therapy offers several advantages compared with conventional wound care methods. One of the most significant benefits is faster healing, as the regenerative activity of stem cells accelerates tissue repair. Rapid wound closure also lowers the risk of infection by reducing the time that tissues remain exposed.
Another advantage is improved cosmetic results. Because stem cells help regulate collagen formation and tissue remodeling, healed skin often appears smoother and more natural. The therapy can also be particularly effective for chronic or treatment-resistant wounds that do not respond well to traditional approaches.
In addition, tissue regenerated with the support of stem cells may be stronger and more resilient, restoring both function and durability to the affected area.
Conclusion: A New Era in Wound Treatment
Stem cell therapy represents a transformative advancement in modern wound care. By harnessing the regenerative capabilities of stem cells, this treatment approach addresses the underlying biological processes involved in tissue repair. Stem cells help rebuild damaged tissue, regulate immune responses, stimulate blood vessel formation, and accelerate healing.
With ongoing scientific progress, stem cell–based treatments may soon become a standard option for managing complex wounds, offering patients faster recovery, reduced complications, and a significantly improved quality of life.

