Type 2 diabetes mellitus (T2DM) develops gradually as the body’s ability to regulate blood glucose becomes impaired. The condition arises from two primary problems that occur simultaneously: the body’s cells become resistant to insulin, and the insulin-producing beta cells in the pancreas progressively lose their function.
Traditional treatments for Type 2 diabetes focus largely on controlling blood glucose levels. While these approaches can be effective in managing symptoms, they generally do not repair the underlying biological damage that causes the disease.
In recent years, regenerative medicine has introduced new possibilities for treating metabolic diseases. Among the most promising innovations is stem cell therapy, particularly treatments using umbilical cord–derived mesenchymal stem cells (UC-MSCs). This emerging approach seeks not only to regulate blood sugar but also to repair damaged pancreatic tissue, restore insulin production, and improve the body’s sensitivity to insulin.
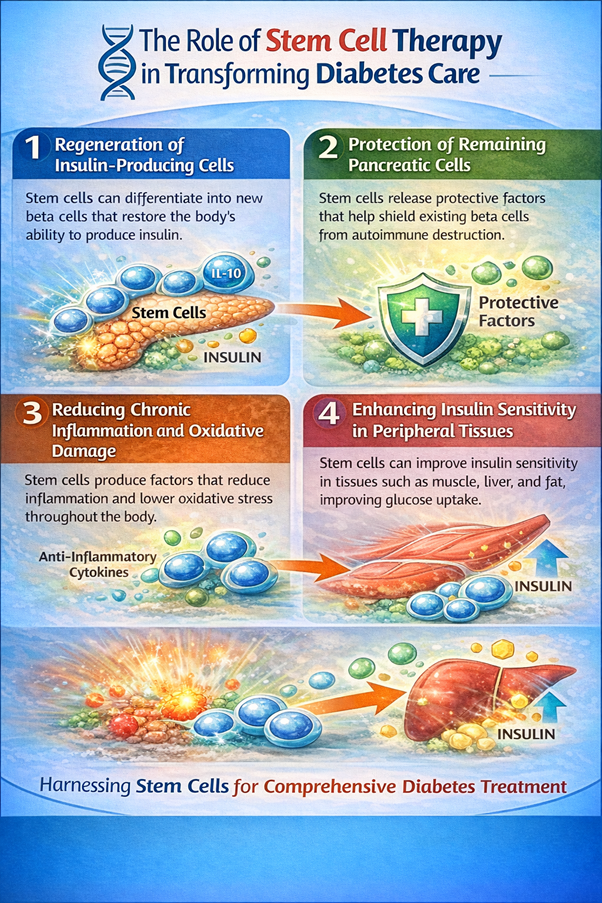
The Role of Stem Cell Therapy in Transforming Diabetes Care
- Regeneration of Insulin-Producing Cells
Stem cells can develop into insulin-producing cells. These newly generated beta-like cells are capable of responding to glucose levels and releasing insulin in a manner similar to natural pancreatic cells. By replacing or supplementing damaged beta cells, stem cell therapy may help restore the body’s natural glucose regulation.
- Protection of Remaining Pancreatic Cells
Stem cells can play an important supportive role in pancreatic health. Stem cells release a wide range of growth factors and signaling molecules that help protect existing pancreatic cells from further damage. These bioactive compounds create a favorable environment within the pancreas by reducing oxidative stress and encouraging tissue repair.
- Reducing Chronic Inflammation and Oxidative Damage
Stem cells are well known for their powerful anti-inflammatory and immunomodulatory properties. They release cytokines and signaling proteins that help regulate immune responses and calm excessive inflammation throughout the body. By restoring immune balance, stem cell therapy may reduce the inflammatory processes that disrupt normal metabolic function.
- Enhancing Insulin Sensitivity in Peripheral Tissues
In many individuals with the condition, muscles, liver cells, and adipose (fat) tissue fail to respond properly to insulin signals. Stem cell therapy may help address this issue by improving the metabolic activity of these tissues. Stem cells can enhance mitochondrial function, decrease inflammatory markers, and support healthier cellular metabolism. These effects can lead to increased glucose uptake by muscle and fat tissues, allowing insulin to work more effectively.
Clinical Research on Stem Cell Therapy for Type 2 Diabetes
- Findings from Clinical Trials
Multiple clinical studies and meta-analyses examining stem cell-based treatments have reported encouraging outcomes. Patients who received stem cell therapy often experienced improvements in several key indicators of metabolic health.
Common findings include reductions in HbA1c levels, which reflect long-term blood glucose control. Many patients also showed lower fasting blood glucose levels following treatment. Improvements in C-peptide levels—an indicator of insulin production—have been observed as well, suggesting that pancreatic function may be partially restored. In some cases, patients were able to reduce their dependence on insulin injections or oral diabetes medications.
- Evidence from Stem Cells Studies
Research specifically involving umbilical cord–derived mesenchymal stem cells has produced similarly promising results. Participants in these studies frequently demonstrated sustained improvements in blood glucose regulation.
Many patients experienced lower fasting glucose levels and increased C-peptide concentrations, indicating better pancreatic activity. Some individuals were able to significantly reduce their insulin requirements, while others achieved periods of insulin independence lasting several months or even years. These outcomes suggest that UC-MSC therapy may have the potential to influence the long-term progression of the disease.
- Long-Term Observational Studies
Follow-up research conducted in Asia and other regions has provided additional insight into the durability of stem cell therapy results. In certain studies tracking patients for one to two years after treatment, improvements in glucose control remained stable throughout the observation period.
Some reports have indicated that a substantial proportion of participants were able to maintain normal or near-normal glucose levels without regular insulin therapy for extended periods.
Stem Cell Therapy Advantages Compared With Conventional Treatments
Stem cell therapy offers several potential benefits compared with standard diabetes management strategies. One major advantage is its regenerative nature. Instead of only lowering blood sugar levels, stem cells work to repair damaged tissues and restore biological function.
As pancreatic cells recover and insulin sensitivity improves, patients may gradually decrease their reliance on medications. Additionally, current evidence suggests that stem cell therapy generally has a strong safety profile, with relatively few reported side effects when administered under proper medical supervision.
Improved metabolic control can also enhance overall quality of life. Patients may experience greater energy levels, fewer complications, and a reduced treatment burden. Perhaps most importantly, stem cell therapy raises the possibility of modifying the disease itself rather than managing it indefinitely.
Thailand’s Role in Advancing Regenerative Diabetes Treatments
Thailand has become an increasingly prominent center for regenerative medicine. The country offers advanced medical facilities equipped with modern biotechnology and specialized laboratories capable of processing stem cells according to international standards.
Clinics in Thailand often provide access to ethically sourced UC-MSC stem cells and experienced medical teams trained in regenerative therapies. In addition, treatment costs are often more accessible compared with many Western countries, attracting patients from around the world.
Many regenerative medicine programs in Thailand also incorporate holistic metabolic care. Patients may receive guidance on nutrition, exercise, and lifestyle modifications alongside stem cell therapy to support long-term health improvements.
Conclusion: A Promising Future for Diabetes Treatment
Stem cell therapy represents a significant shift in how Type 2 diabetes may be treated in the future. By targeting the fundamental biological mechanisms responsible for the disease—including inflammation, insulin resistance, and beta cell loss—regenerative medicine offers a pathway toward true tissue repair.
As regenerative medicine continues to evolve, countries such as Thailand are helping lead the way in developing innovative therapies that may redefine the future of diabetes care and offer new hope for patients worldwide.

