Ovarian aging is a natural process that begins early in life. Women are born with a finite number of egg cells, and this reserve steadily declines over time. As women reach their late 30s and 40s, both the quantity and quality of these eggs diminish more rapidly.
Traditional approaches to fertility treatment can offer temporary solutions but typically do not address the underlying deterioration of ovarian tissue.
Advances in regenerative medicine are reshaping the landscape of reproductive health, offering new hope to women facing fertility challenges. Among these innovations, stem cell–based therapies—are emerging as a promising approach for ovarian rejuvenation. Unlike conventional fertility treatments that focus on short-term stimulation, stem cell therapy seeks to restore the ovarian environment itself, potentially reactivating its natural functions.
Stem Cells in Reproductive Regeneration
Stem cells possess the distinctive capacity to renew themselves and differentiate into a wide range of specialized cell types. Their regenerative properties have been widely studied in fields such as neurology, cardiology, and dermatology. In reproductive medicine, their role is less about creating new egg cells and more about revitalizing the ovarian microenvironment. By improving tissue quality, enhancing blood circulation, and supporting cellular communication, stem cells may help dormant follicles resume activity.
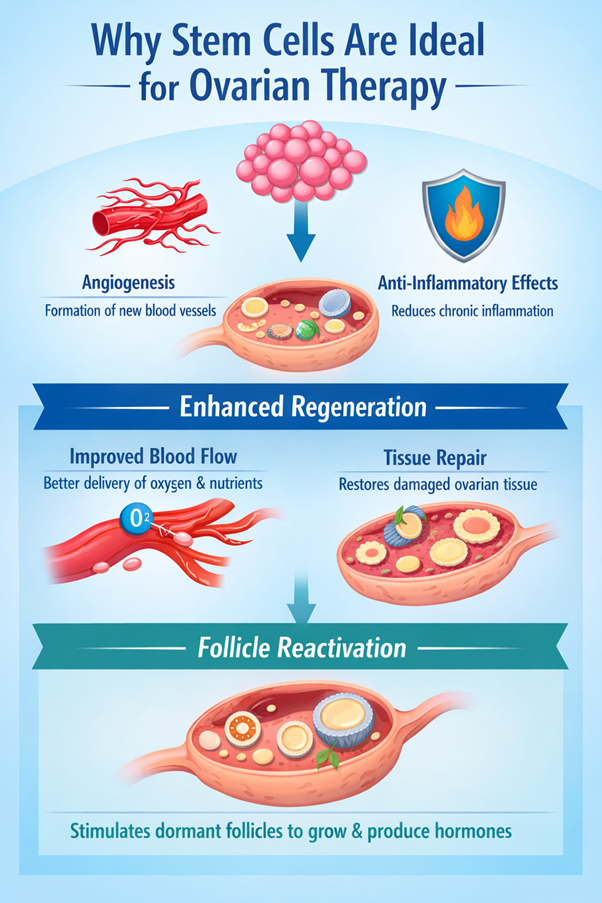
Why Stem Cells Are Ideal for Ovarian Therapy
Stem cells are particularly well-suited for this purpose. These cells are known for their strong regenerative capacity, low immunogenicity, and ability to release beneficial signaling molecules. The therapeutic process typically begins with the careful collection and laboratory preparation of these cells under strict safety standards. Once processed, they are administered directly into the ovaries using minimally invasive techniques such as laparoscopy or ultrasound-guided injection.
After introduction into ovarian tissue, stem cells initiate a range of biological responses that support regeneration. One of the key mechanisms is angiogenesis, the formation of new blood vessels. Improved blood flow enhances the delivery of oxygen and nutrients, which are essential for cellular repair and follicular development. Additionally, these stem cells exert anti-inflammatory effects, helping to reduce chronic inflammation that can impair ovarian function.
Another important aspect of their action is tissue repair. Stem cells release growth factors and cytokines that stimulate local cells to regenerate damaged structures within the ovary. This process may help restore a healthier environment for follicles, increasing the likelihood that dormant or early-stage follicles can resume growth and contribute to hormone production.
Clinical Outcomes and Early Evidence
Early clinical observations have shown encouraging results. Some women undergoing ovarian stem cell therapy have experienced the return of menstrual cycles after extended periods of absence. Others have demonstrated improvements in hormone levels, including increased AMH, which is often used as an indicator of ovarian reserve. In certain cases, spontaneous pregnancies have been reported following treatment, suggesting a potential restoration of natural fertility.
While much of the existing research has focused on mesenchymal stem cells derived from bone marrow or adipose tissue, stem cells may offer additional advantages. Their origin from neonatal tissue gives them a more youthful profile and enhanced regenerative signaling capabilities. This allows them to produce a wide array of bioactive factors that support healing and tissue renewal.
Emerging Techniques in Ovarian Recovery
In parallel with stem cell therapy, other experimental techniques are being explored to further enhance ovarian recovery. One such method is in vitro activation (IVA), where ovarian tissue is temporarily removed, treated externally to stimulate follicle growth, and then reimplanted. When combined with stem cell support, this approach may improve outcomes by creating a more favorable environment for follicle activation.
Ongoing research is also focusing on ways to optimize treatment effectiveness. For instance, combining stem cell therapy with platelet-rich plasma (PRP) has gained attention. PRP, derived from the patient’s own blood, is rich in growth factors that can complement the regenerative effects of stem cells. Additionally, advances in tissue engineering have led to the development of bioengineered scaffolds—three-dimensional structures designed to support stem cell growth and integration within ovarian tissue.
Another promising area involves the identification of predictive biomarkers. By understanding which patients are most likely to respond positively to stem cell therapy, clinicians can tailor treatments more precisely, improving outcomes and minimizing unnecessary interventions.
Thailand as a Leader in Regenerative Fertility Care
Thailand has emerged as a leading destination for this type of advanced reproductive care. The country combines modern medical infrastructure with experienced fertility specialists and a strong focus on innovation. Clinics offering stem cell therapy operate under established safety and ethical guidelines, ensuring that treatments meet international standards.
Patients seeking care in Thailand often benefit from personalized treatment plans that include thorough pre-treatment evaluations and ongoing monitoring. Hormonal levels, ovarian response, and overall health are carefully assessed to track progress and adjust therapies as needed. In addition to clinical expertise, Thailand is known for its affordability and patient-centered approach, attracting individuals from around the world.
Conclusion: Renewed Hope for Women with Infertility
The future of fertility treatment is increasingly moving toward regenerative solutions. Stem cell–based ovarian rejuvenation represents a shift away from purely supportive therapies toward interventions that aim to restore natural biological function. Current findings suggest that stem cell therapy holds significant potential.
For women facing infertility due to ovarian aging or premature decline, this innovative approach offers renewed possibilities. By enhancing ovarian health, improving hormone production, and potentially reactivating dormant follicles, stem cell therapy may help restore fertility in ways previously thought unattainable.
As research continues to evolve, stem cell therapy may become an integral part of mainstream reproductive medicine. Its ability to address the root causes of ovarian dysfunction positions it as a transformative option in fertility care—one that not only supports conception but also promotes overall reproductive well-being.

