Scientific Advancements of UC-MSCs for Rheumatoid Arthritis Treatments via Stem cell therapy in Thailand to Improve Patient Quality of Life
Rheumatoid Arthritis represents a formidable challenge to modern medicine because it is a chronic systemic autoimmune disorder characterized by persistent synovial inflammation. This condition does not merely cause temporary discomfort but leads to progressive joint destruction, functional disability, and a significant reduction in quality of life. For many patients, the physical pain is accompanied by systemic complications affecting the heart and lungs, making the severity of the disease profound. While pharmacological interventions have advanced, a substantial portion of the patient population remains unresponsive to traditional biological therapies. This therapeutic gap has necessitated the exploration of regenerative medicine, specifically Stem cell therapy in Thailand, as a transformative approach to reset the immune system rather than just masking the symptoms. By utilizing UC-MSCs, researchers and clinicians are now looking toward a future where long-term remission is a tangible reality for those suffering from this debilitating bone and joint ailment.
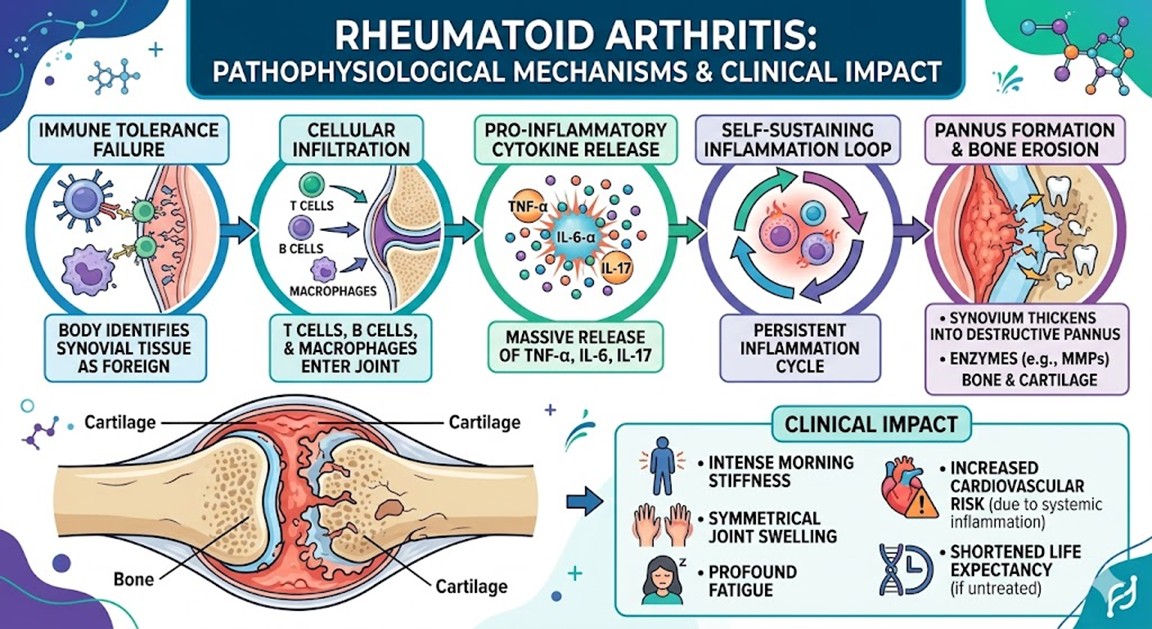
1.Pathophysiological Mechanisms and Clinical Impact
The onset of Rheumatoid Arthritis is marked by a complex failure of immune tolerance where the body identifies its own synovial tissue as foreign. The primary mechanism involves the infiltration of T cells, B cells, and macrophages into the joint capsule. This cellular influx triggers a massive release of pro-inflammatory cytokines, including Tumor Necrosis Factor-α and various Interleukins like IL-6 and IL-17. These molecules create a self-sustaining loop of inflammation that causes the synovium to thicken into a destructive tissue called pannus. The pannus eventually invades the cartilage and bone, utilizing enzymes like matrix metalloproteinases to dissolve the joint structure. Beyond the physical erosion, patients experience intense morning stiffness, symmetrical joint swelling, and profound fatigue. If left unchecked, the inflammatory environment extends to the vascular system, increasing the risk of cardiovascular disease and significantly shortening life expectancy for many individuals.
2.Current Therapeutic Approaches and Limitations
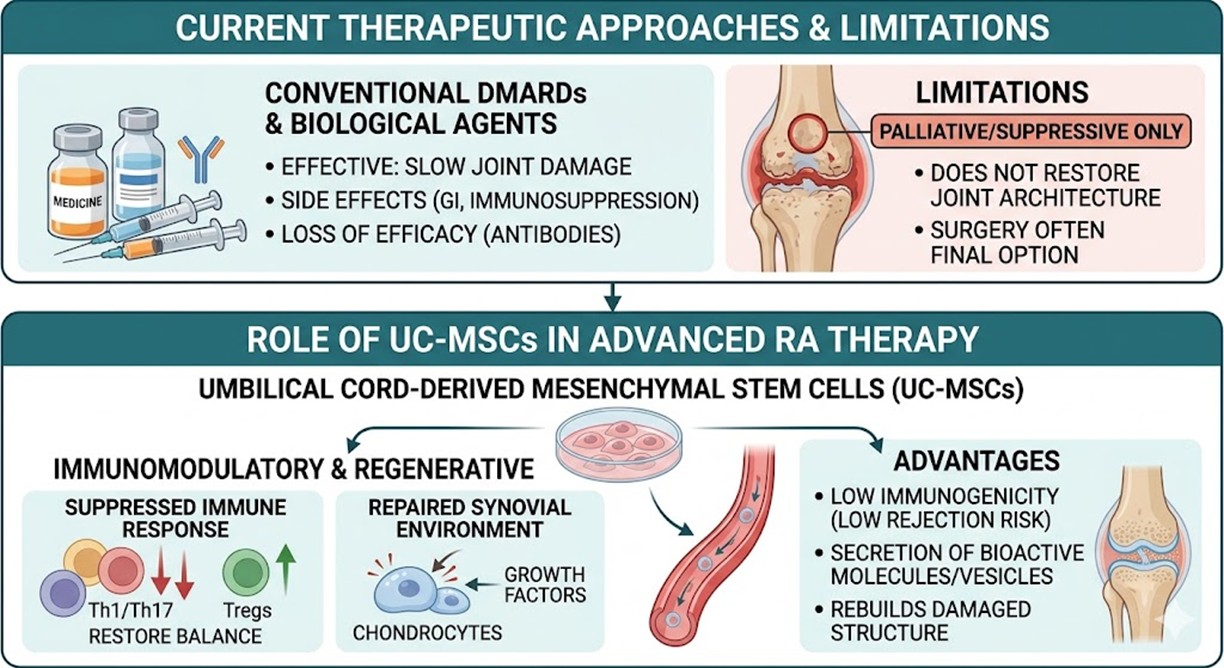
Traditionally, the Rheumatoid Arthritis management of this condition has relied on Disease-Modifying Anti-rheumatic Drugs and more recently, biological agents. While these treatments are effective at slowing down the progression of joint damage, they are not without significant drawbacks. Many patients suffer from side effects ranging from gastrointestinal distress to severe immunosuppression, which leaves them vulnerable to opportunistic infections. Furthermore, biological therapies often lose their efficacy over time as the body develops neutralizing antibodies against the medication. Perhaps the most critical limitation is that these standard treatments are purely palliative or suppressive; they do not address the underlying immune dysregulation or repair the damaged cartilage. Once the joint architecture is lost, pharmacological intervention cannot restore function, often leaving surgery as the final, invasive option for those in advanced stages.
3.The Role of UC-MSCs in Advanced Rheumatoid Arthritis Therapy
Transitioning toward UC-MSCs offers a biological advantage that traditional drugs cannot replicate. These Umbilical Cord-derived Mesenchymal Stem Cells are prized for their potent immunomodulatory and regenerative properties. Unlike other cell sources, these cells possess low immunogenicity, meaning they can be administered without the high risk of rejection. The core mechanism of the treatment involves the secretion of bioactive molecules and extracellular vesicles that actively suppress the overactive immune response. Specifically, these cells inhibit the proliferation of Th1 and Th17 cells while simultaneously promoting the expansion of regulatory T cells. This shift restores the balance of the immune system. Additionally, the cells secrete growth factors that stimulate the resident chondrocytes to begin repairing the damaged synovial environment. This dual action of stopping the fire while rebuilding the structure makes this form of Rheumatoid Arthritis therapy a superior alternative for refractory cases.
4.The Future of UC-MSCs Research in Thailand
The landscape for Stem cell therapy in Thailand is expanding rapidly, positioned at the intersection of high-quality medical infrastructure and progressive regulatory frameworks. Thailand has emerged as a regional leader in regenerative medicine due to its significant investment in biotechnology and specialized medical facilities. The future of treating Rheumatoid Arthritis in the country looks promising as clinical trials continue to demonstrate the safety and efficacy of UC-MSCs. The reason Thailand has become a focal point for this research is the combination of world-class medical expertise and a cost-effective healthcare model that allows for broader access to cutting-edge treatments. As the global medical community moves toward personalized medicine, the integration of these advanced cellular therapies into the local clinical practice ensures that patients have access to the most modern options available globally.
In summary, the transition from managing symptoms to addressing the root cause of autoimmune joint destruction represents a pivotal shift in rheumatology. The integration of UC-MSCs into the clinical workflow provides a multifaceted solution that targets inflammation while encouraging tissue repair. While traditional drugs have served their purpose, the limitations in their long-term efficacy and safety profiles highlight the need for the innovative solutions found within Stem cell therapy in Thailand. By leveraging the unique immunomodulatory mechanisms of mesenchymal cells, clinicians can offer hope to patients who have previously exhausted all other medical avenues. The ongoing research and clinical successes within the Thailand medical sector continue to pave the way for a new era of treatment where the goal is no longer just survival but the complete restoration of joint health and systemic well-being.

