Innovation of UC-MSCs for Stem Cell Treatment for Chronic Back Pain in Thailand
Global healthcare systems are overwhelmed by severe spinal ailments results in permanent disability. Back Pain or thoracic region is not a trivial matter but it is a severe and protracted disability. It depletes the quality of life of multitudes of individuals culminates in death. The problems are cause for a society, including healthcare, occupational, and economic costs, can even include the opioid crisis. Conventional Back Pain remedying approaches ignore the ongoing biological degeneration of the intervertebral discs. This is why medicine is focused on the cutting edge of regenerative medicine, which, for the first time, allows doctors to offer a biological remedy that addresses the underlying causes of a patient’s problems, instead of merely relieving the patient’s problems. This is made possible by UC-MSCs.
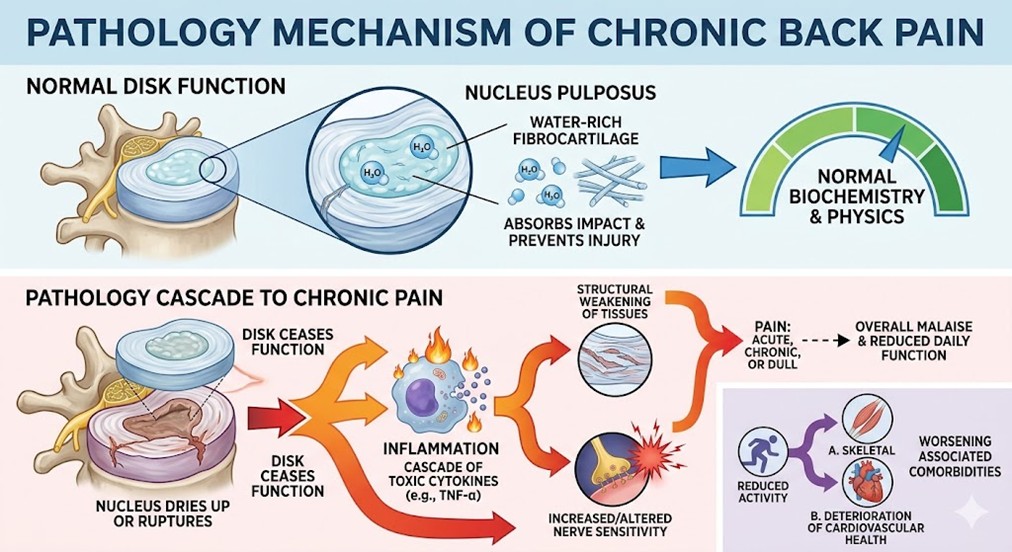
1.Pathology mechanism of Chronic Back Pain
In Normally, there is a system of specific biochemistry and physics that spinal discs utilize to function properly. Each disc contains a nucleus pulposus at its center, which is a fibrocartilage structure that is primarily composed of water. Discs act to prevent injury by absorbing impact. However, in the event that the nucleus dries up or ruptures, the disc ceases to function and a cascade of toxic cytokines will trigger adjacent tissues to become immensely inflamed. TNF-α and other cytokines that promote inflammation led to structural weakening of tissues, which subsequently elicits an increased or an altered sensitivity of the nerves in the area. This ultimately manifests as acute, chronic, or in some instances, dull Pain, which in turn leads to an overall malaise. The impact of this condition on an individual greatly reduces the ability to perform normal daily functions, and, in some instances, can lead to increased overall inactivity. Such a decrease in activity can initiate or worsen a number of associated comorbidities, including the deterioration of cardiovascular health and the atrophy of skeletal muscles.
2.The Conventional invention and Treatment limitations of Back Pain
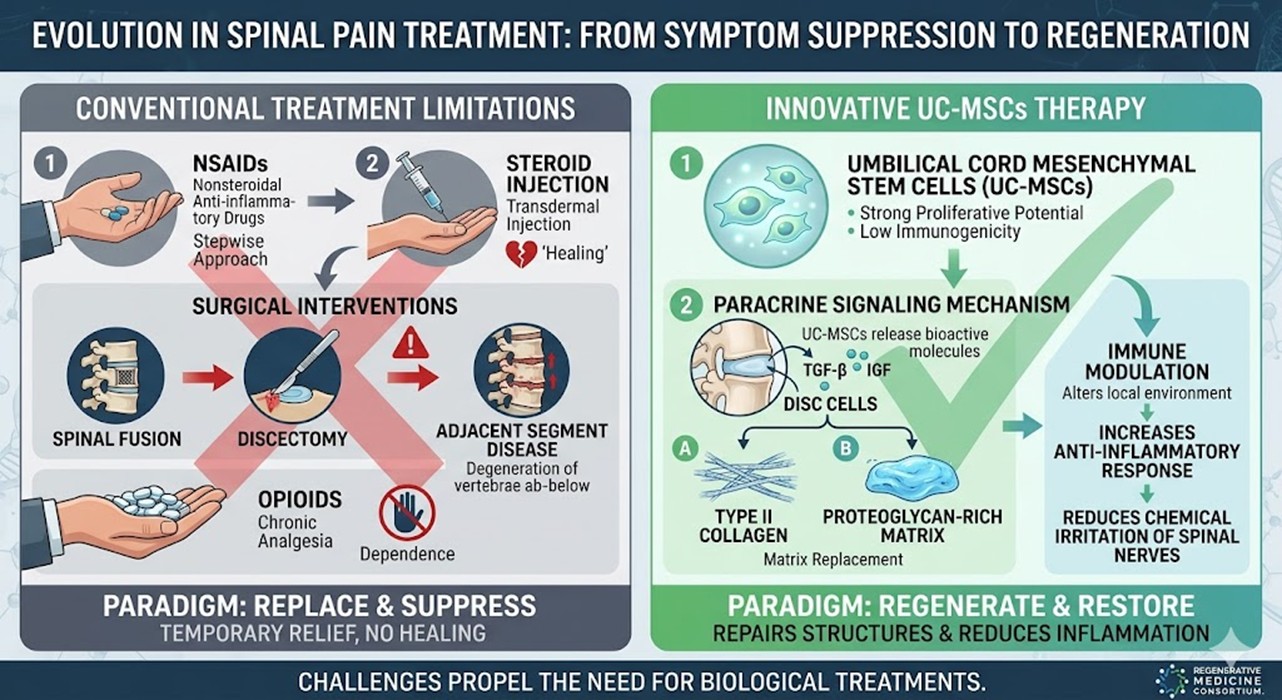
The most typical approach in treating Back Pain in contemporary medicine consists of a stepwise approach that initiates at the administration of nonsteroidal anti-inflammatory drugs and culminates in transdermal steroid injection. While such a regimen can provide transient analgesia, there is no impact on the healing of the injured tissues. In complicated presentations, devices for fusion or discectomy are placed surgically to provide stabilization of certain segments of the spine and/or to relieve the encroachment of nerves. Surgery is highly invasive and can provoke a condition known as adjacent segment disease, which is characterized by the rapid failure of the vertebrae immediately superior and inferior to the surgically reduced segment. Furthermore, in the chronic setting of opioid analgesia, there exists the potential for addiction and additional physical harm to the individual. Collectively, these challenges have necessitated the change in treatment modalities from a paradigm of replacement and suppression to regeneration and restoration. This has increased the demand for more biological treatments.
3.The innovative application of UC-MSCs
The advantages of UC-MSCs over earlier methods are their combination of strong proliferative potential with low immunogenicity which provides promise for clinical therapeutic transplantation. The effect of these cells is primarily mediated through paracrine signaling. Paracrine signaling is when transplanted cells release bioactive proteins such as transforming growth factor-β and insulin-like growth factor. These proteins signal cells in the disc to produce more type II collagen and the proteoglycan-rich matrix of the disc which assists in matrix replacement. These cells can also alter and potentially increase the local environment of the immune system to be more anti-inflammatory which can reduce the chemical irritation of the spinal nerves. The spinal Stem Cell Therapy in Thailand and elsewhere is becoming more widely accepted because in addition to repairing the structures it reduces inflammation.
4.The future of novel cellular therapies for Thai medical system
The future of these novel cellular therapies looks bright for the Thai medical system. Thailand has emerged as one of the top medical tourism destinations due to its investments in dedicated cellular biotechnologies and specialized healthcare. Due to the rigorous clinical protocols and the highly skilled regenerative orthopedic surgeons, international patients are increasingly seeking Stem Cell Therapy in Thailand. This is also true for Thailand’s novel UC-MSCs and integrated system for the management of chronic diseases. Thai clinical facilities in collaboration with research institutes are able to utilize the best available cellular therapies and their delivery systems to offer patients the highest quality of care. Spinal care is evolving from basic mechanical or chemical modalities to more sophisticated and integrated approaches.
Utilizes UC-MSCs and regenerative medicine to provide care at the cellular level, which neither medications, nor conventional surgery, can achieve. This level of care is required to break the cycles of cellular depletion and inflammation seen in chronic disc issues. For patients who have not responded to many other modalities, the introduction of high potency cellular treatments to the clinic is a significant milestone. As the physicians in Southeast Asia continue to refine these therapeutics, an increasing number of patients will be able to achieve complete recovery and restoration of functional autonomy. Stem Cell Therapy in Thailand is revolutionizing Back Pain management by placing emphasis on the body’s intrinsic healing mechanisms.

