Knee Osteoarthritis (OA) is a very present form of degenerative joint disease which we see progress into cartilage degeneration, chronic inflammation and function loss in affected joints. Presently we have treatment protocols which are aimed at symptom relief via pharmacology, physical rehabilitation and surgery in advanced stages. What we see is that these methods do not repair damaged cartilage or reverse the base level of joint degeneration. In this respect it has been the recent advances in regenerative medicine which have brought to light the possible pro healing and anti inflammatory role of mesenchymal stem cells (MSCs) which include umbilical cord derived MSCs (UC-MSCs). Thailand has become a region wide center for stem cell based therapies which have dedicated clinical infrastructure for this field also integrated care models. This article looks at the path physiology of knee osteoarthritis, the which traditional treatments fall short of and the use of stem cell therapy which is put forth as a research based approach to support joint health in Thailand.
- Introduction
Knee osteoarthritis (OA) is among the most common causes of chronic joint pain and disability globally. It is known as a degenerative joint disease. As it progresses, the patients will experience pain, stiffness, limited mobility and diminished quality of life. Risk factors are aging, obesity, joint injury and mechanical stress. Management strategies currently mostly centre on reduction of symptoms rather than restoration of structure. Consequently, there is an ever-growing interest in regenerative medicine strategies designed to promote tissue repair and alter the disease course. Thailand gained international recognition as one of the stem-cell therapy-focused countries, providing patients with the opportunity to explore new methods of regenerative therapies.
- Pathophysiology of Knee Osteoarthritis
Multiple mechanical, biomechanical, and inflammatory processes drive knee OA.
Cartilage Degeneration
Extracellular matrix components such as collagen and proteoglycans are lost with the effect that cartilaginous integrity decreases.
Synovial Inflammation
Joint Pain and Ongoing Cartilage Degeneration Related Concepts
Subchondral Bone Changes
Changes in the underlying bone structure alter joint stability and load distribution.
Oxidative Stress
Reactive oxygen species accumulation leads to chondrocyte dysfunction, and tissue injury.
Imbalance in Repair Mechanisms
Cartilage has a reduced regenerative capacity and cannot restore damaged cartilage. These processes interact to form a cycle of progressive joint degeneration.
- Limitations of Conventional Therapeutic Approaches
Knee OA is generally treated with NSAIDs, physical therapy, suprapatellar injections and/or similar surgical procedures. Although these approaches can alleviate symptoms, they do not restore damaged cartilage. Corticosteroid injections can temporarily reduce inflammation, but they do not change disease progression. In severe cases, surgical procedures such as total knee replacement may be necessary. Though efficient, surgical intervention poses risks and is not applicable in all patients.
A scarcity of therapies to regenerate cartilage has fueled interest in alternative strategies.
- Mesenchymal Stem Cells in Knee Osteoarthritis
Research in mesenchymal stem cells which includes that of umbilical cord derived MSCs looks at their role in improving joint health. Instead of producing cartilage themselves what these cells do is emit what are called paracrine signals which in turn guide and support the entire joint ecosystem.
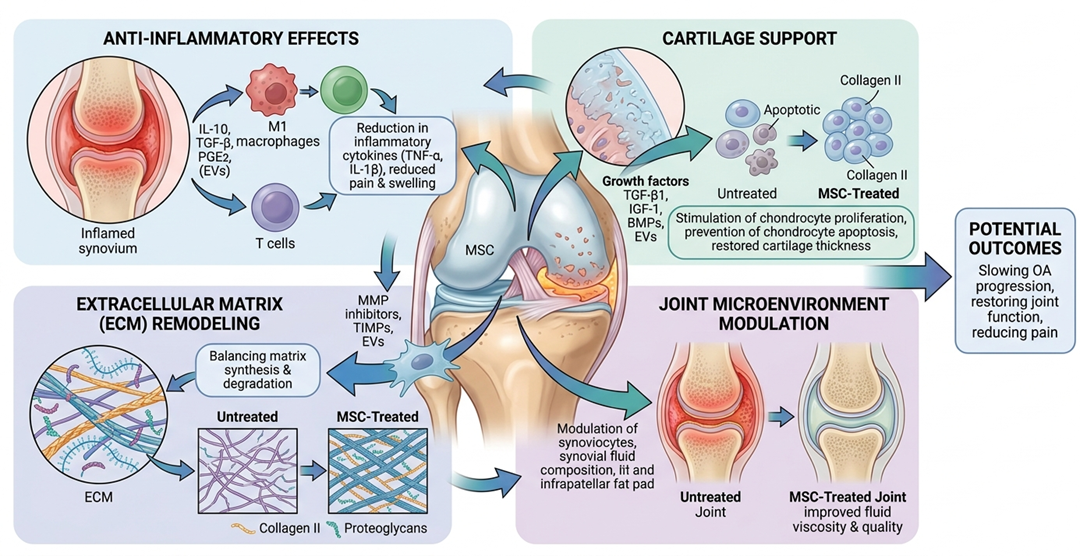
How They May Help
- Reducing Inflammation : MSCs secrete molecules that reduce inflammation of the joint lining and will help drive the immune response to balance.
- Supporting Cartilage Cells : Their signaling can improve cartilage cell performance and prompt them to make the proteins required to maintain healthy joint
Improving Tissue Structure : MSC formulations can perhaps facilitate collagen production and promote a straighter alignment of joint tissue (and thereby aligning those tissues to arthritic injury throughout the disease process).
- Helping With Pain: MSCs can potentially alleviate joint pain by reducing inflammation as well.
- Creating a Healthier Joint Environment
Overall, it appears that MSCs create an environment more conducive to the joint’s self-repair.
- Clinical Applications and Thailand as a Medical Hub
Thailand has become a regional hub of regenerative medicine and numerous specialized clinics provide advanced stem cell–based treatments.
In clinical settings, MSCs can be delivered into the knee joint via intra-articular injection, either alone or with simultaneous systemic administration. And imaging guidance might be used for accurate delivery.
While early clinical observations suggest that some patients may have improvements in pain, mobility and joint function. However, results can vary, and these treatments are still investigational.
Home to cutting-edge lab capabilities and a strong foundation of patient-centric care, Thailand is playing an increasingly significant role in the field of regenerative medicine.
- Future Perspectives
Stem cell therapy for knee OA reflects a change to regenerative strategies that target the underlying pathophysiology of disease and its progression.
Future research directions include:
- Dissecting molecular mechanisms of MSC-mediated cartilage repair
- Delivery methods & dosing approaches optimization
- Evaluating long-term safety and efficacy
- Recognizing patient populations with potential for the greatest benefit
- Non-cellular approaches, like exosome based therapies, are being considered as well.
Only large-scale randomized clinical trials will be sufficient to determine the clinical role of these therapies.
Conclusion
Knee osteoarthritis is a degenerative disease involving cartilage degeneration, inflammation, and impaired function. Therapies do not reach help improve symptoms and inflammation but they don’t necessarily restore the joint structure. Specifically, mesenchymal stem cells (MSCs) based therapies show great potential for enhancing tissue regeneration, rebalancing inflammatory response and modulating the destruction of joint microenvironment. The clinical applications in Thailand highlight the interest in regenerative approaches. Nevertheless, these therapies are investigational and additional studies are needed to clarify their long-term clinical value.

