Introduction
For this reason, many families continue to seek advanced care for autism spectrum disorder: not only because progress can vary on a per-child basis, but also because even ongoing therapy may leave ongoing challenges in daily life. Over the last few years, UC-MSCs have attracted a lot of attention as scientists explore how these cells might help support or nurture the body through immunomodulatory activity and signaling effects. A 2026 review summarized nine early-phase MSC trials in autism, describing the field as promising and as being of interest to families searching for more holistic strategies of support.
Why UC-MSCs are being studied in autism
Due to their ability to modulate pathways that are typically inflammatory in nature and facilitate a more favorable tissue microenvironment through paracrine signaling, UC-MSCs are potentially candidates for examining in autism research. That is just one reason they are considered an exciting possibility in contemporary regenerative studies. Instead of describing them as a stand-alone solution, it’s much better to explain that they are being investigated within a wider support structure that could complement developmental therapies and rehabilitative-based care.
Potential benefits families want to understand
In fact, when families ask about benefits, the answer that is out there and most meaningful to them really has to do with function and participation and day-to-day process. Encouraging signals have been reported in early clinical work, with some children showing improved measures of autism following infusion of cord tissue mesenchymal stromal cells. In the Duke phase I study, six of 12 participants showed improvement in at least two ASD-specific measures, and the treatment process was termed well tolerated in that small cohort. Such early finding helps illustrate why families are still interested in UC-MSC-based care.
Benefit should not, however, be expressed exclusively in the language of points. For many families, the actual objective is better day-to-day engagement: better attention to tasks and calmer routines; better engagement in therapy; more consistent function at or home or school. What parents really need is not just “stem cell treatment,” but integrated autism support that combines investigational medical care with therapies for helping children leverage their abilities in the real world.
Why occupational therapy matters so much
Occupational therapy, or OT, is one of the most practical elements in autism care because it emphasizes how a child participates in everyday routines. Recent practice guidelines from AOTA focus on OT for ADL, IADL, play, leisure, positive mental health and self-determination. That means OT is directly relevant to some of the most common priorities for families: dressing, feeding, sensory regulation, play skills and routines in the classroom and at home.
As such, OT is certainly a good companion to any broader autism program in Thailand. When a family is faced with the decision of considering advanced regenerative care, occupational therapy helps translate treatment goals into tangible priorities. OT works with a child to create tolerance, participation, consistency and confidence in ‘real’ places rather than just focusing on biology. Because occupational therapy may help with quality of life and participation in daily life, a review from 2024 on the use of OT in children with ASD noted it’s also particularly helpful as part of a multidisciplinary care plan.
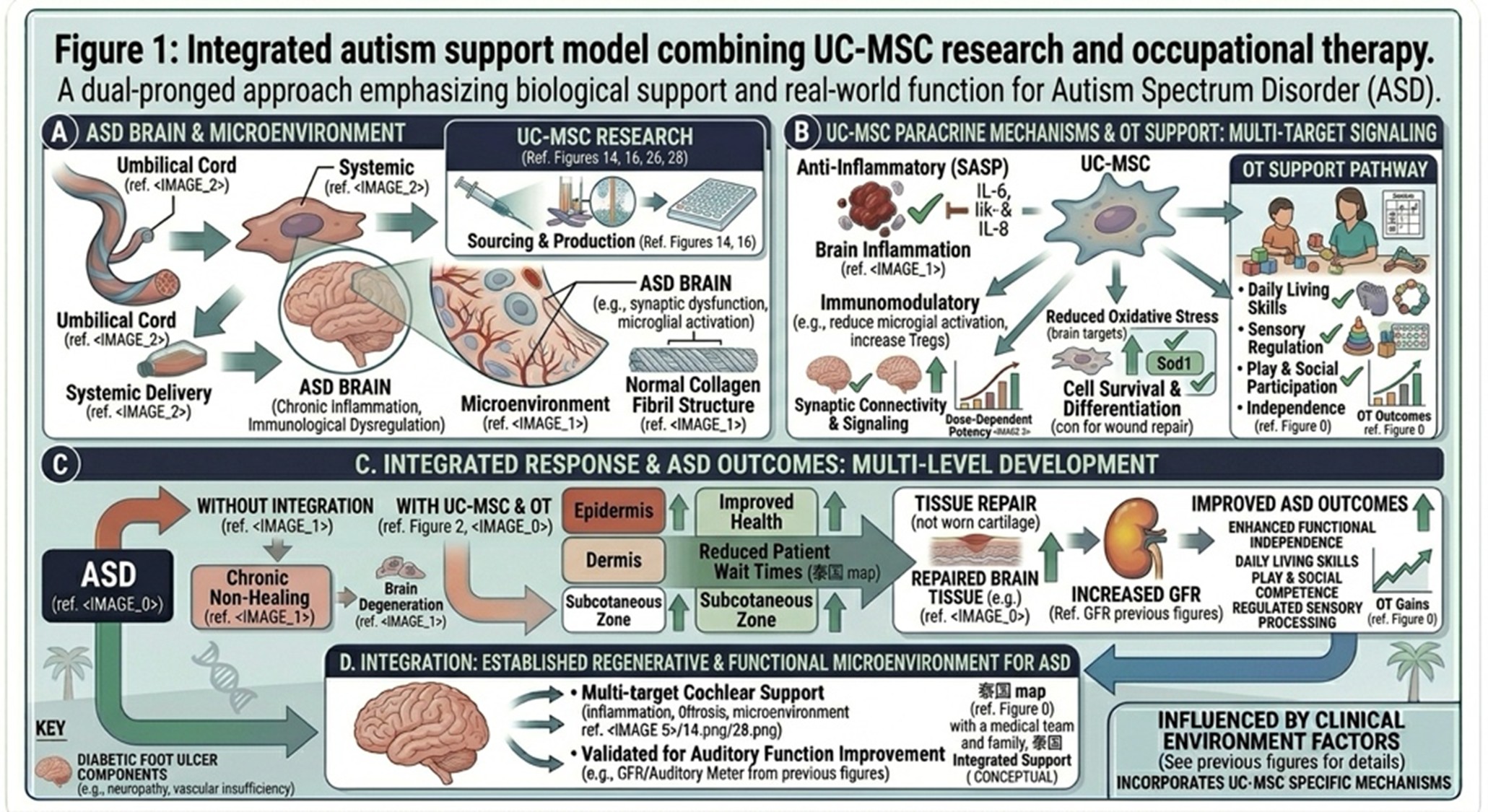
How to explain the benefit of OT
A OT section might say that therapy can assist children in developing:
- sensory regulation
- feeding and self-care routines
- sitting tolerance and task participation
- play and interaction
- school readiness and classroom engagement
- independence at home
This kind of benefit language tends to resonate more with parents, because it ties treatment to real life. The article strengthens and makes it more family-centered, as OT practice guidelines explicitly promote participation-focused care throughout the lifespan.

