Alzheimer’s disease is a progressive neurological disorder that gradually impairs memory, thinking abilities, and everyday functioning. It is one of the leading causes of dementia worldwide and poses a major challenge to patients, families, and healthcare systems. The disease is marked by the accumulation of abnormal protein deposits in the brain—specifically amyloid-beta plaques and tau tangles—which disrupt communication between neurons and eventually lead to widespread cell death.
Despite advances in medical science, current treatments for Alzheimer’s disease are largely limited to symptom management. Medications may temporarily improve memory or cognitive function, but they do not address the root causes of the condition or stop its progression. As a result, attention has increasingly turned toward regenerative medicine. Among the most promising approaches is therapy using umbilical cord-derived mesenchymal stem cells (UC-MSCs), which aim to repair damaged brain tissue, reduce inflammation, and restore neural function.
In Thailand, where regenerative therapies are rapidly developing, stem cell treatment is gaining attention as an innovative strategy for tackling neurodegenerative diseases at a deeper biological level.
The Function of Stem Cells in Restoring Brain Tissue
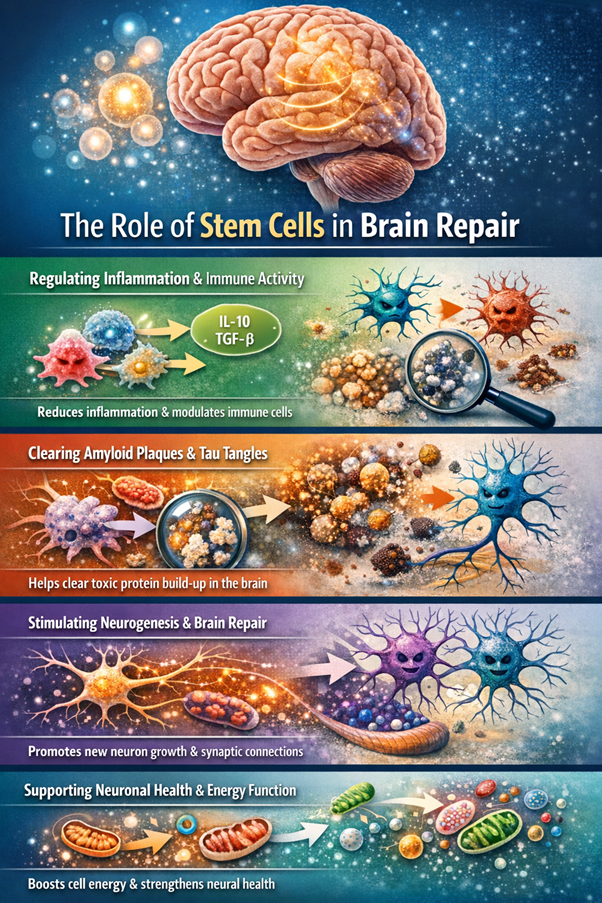
Regulating Inflammation and Immune Activity: Chronic inflammation in the brain is a key contributor to the progression of Alzheimer’s disease. Immune cells in the brain, including microglia and astrocytes, can become overactivated and shift into a harmful state, releasing substances that accelerate neuronal damage.
Stem cells help counteract this process by producing anti-inflammatory molecules such as interleukin-10 (IL-10) and transforming growth factor-beta (TGF-β). These substances suppress the release of pro-inflammatory cytokines like IL-1β and tumor necrosis factor-alpha (TNF-α), thereby reducing harmful inflammation.
In addition, stem cells can influence the behavior of brain immune cells. They encourage microglia and astrocytes to transition from destructive states into protective, healing-oriented forms. This shift not only limits ongoing damage but also creates a more supportive environment for tissue repair and recovery.
Addressing Amyloid Plaques and Tau Tangles: One of the defining features of Alzheimer’s disease is the accumulation of toxic proteins in the brain. Amyloid-beta plaques build up outside neurons, while tau tangles form inside them, both contributing to disrupted cell function and eventual cell death.
Stem cell therapy offers a unique advantage by targeting these pathological hallmarks directly. Stem cells can stimulate the brain’s natural mechanisms for clearing these harmful proteins. For example, they may activate microglia to identify and remove amyloid deposits more effectively.
Additionally, stem cells can promote the production of enzymes such as neprilysin and insulin-degrading enzyme, which help break down amyloid-beta. They also enhance cellular processes like autophagy and lysosomal activity, which are responsible for removing damaged or unnecessary components within cells.
Through these combined actions, stem cells may help reduce the accumulation of toxic proteins and support the restoration of healthier brain function.
Stimulating Neurogenesis and Brain Repair: Alzheimer’s disease disrupts the brain’s natural ability to generate new neurons, particularly in regions like the hippocampus, which is critical for memory formation. Stem cell therapy may help revive this regenerative capacity.
Stem cells can activate dormant neural stem cells within the brain, encouraging them to produce new neurons. They also support the formation of new synaptic connections, improving communication between nerve cells. Increased synaptic density is closely linked to better cognitive performance and memory retention.
By enhancing neurogenesis and rebuilding neural networks, stem cell therapy may not only slow cognitive decline but also contribute to functional recovery in certain cases.
Supporting Neuronal Health and Energy Function: Beyond promoting regeneration, stem cells provide important protective benefits for existing neurons. One remarkable mechanism involves the transfer of mitochondria—tiny structures within cells responsible for energy production—from stem cells to damaged neurons. This transfer can help restore energy balance and improve cellular function.
Stem cells also release extracellular vesicles, which are small particles that carry proteins, lipids, and genetic material such as microRNAs. These vesicles deliver signals that can reduce inflammation, enhance cell survival, and strengthen synaptic connections.
MicroRNAs such as miR-21 and miR-124 play a role in regulating gene expression and supporting neuronal health. By delivering these molecules, stem cells contribute to a more stable and resilient neural environment.
A Multifaceted Treatment Strategy
One of the greatest strengths of stem cell therapy lies in its ability to address multiple aspects of Alzheimer’s disease simultaneously. Rather than focusing on a single target, stem cells provide a comprehensive approach that includes:
- Supporting neuron survival through growth factor release
- Reducing harmful inflammation in the brain
- Promoting the breakdown and clearance of toxic proteins
- Encouraging the formation of new neurons and synaptic connections
- Enhancing cellular energy and metabolic function
- Delivering therapeutic molecules via extracellular vesicles
This multi-layered strategy distinguishes stem cell therapy from traditional treatments and positions it as a potentially transformative option.
Looking Ahead
As research continues to advance, stem cell therapy is emerging as a promising direction in the fight against Alzheimer’s disease. Its ability to promote repair, protect neurons, and address underlying disease mechanisms offers hope for more effective and long-lasting treatments.
In Thailand, ongoing developments in regenerative medicine are making such therapies increasingly accessible. With continued scientific progress and carefully conducted clinical studies, stem cell-based treatments may one day move beyond experimental stages to become part of standard care.
The potential of stem cell therapy to not only manage symptoms but also repair damage and restore function represents a significant step forward in addressing one of the most complex neurological disorders of our time.

