Transforming Joint Health: Osteoarthritis Stem Cell Therapy in Thailand and the Future of Regenerative Medicine for Osteoarthritis
The global healthcare landscape is currently grappling with the escalating burden of degenerative joint conditions, with Osteoarthritis emerging as a primary cause of chronic disability. This condition is no longer viewed merely as an inevitable consequence of aging but rather as a complex inflammatory syndrome that leads to the progressive breakdown of articular cartilage. Osteoarthritis patients suffering from this ailment experience a profound decline in quality of life, characterized by persistent pain, restricted mobility, and a gradual loss of independence. The socioeconomic impact is equally staggering, as the costs associated with long term care, loss of productivity, and surgical interventions continue to rise. Because the body possesses a limited capacity to repair hyaline cartilage, the progression of the disease often feels like a slow, irreversible decline that affects millions of individuals across various demographics.
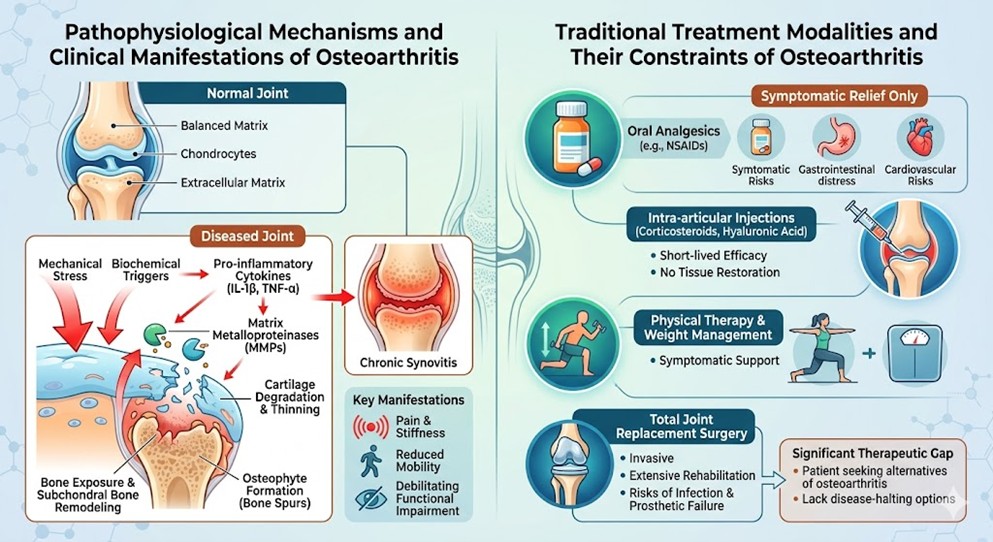
- Pathophysiological Mechanisms and Clinical Manifestations of Osteoarthritis
The underlying mechanism of Osteoarthritis involves a disruption in the delicate balance between the synthesis and degradation of the extracellular matrix within the joint. Under normal physiological conditions, chondrocytes maintain this equilibrium. However, in an osteopathic state, mechanical stress and biochemical triggers activate pro inflammatory cytokines, particularly interleukin 1-β and tumor necrosis factor-α. These molecules stimulate the production of matrix metalloproteinases which actively dismantle the structural framework of the cartilage. As the cartilage thins, the underlying bone becomes exposed, leading to subchondral bone remodeling and the formation of osteophytes. This structural failure is accompanied by chronic synovitis, where the joint lining becomes inflamed, further exacerbating pain and stiffness. The severity of the Osteoarthritis is often measured by the total loss of joint space, resulting in debilitating functional impairment.
- Traditional Treatment Modalities and Their Constraints of Osteoarthritis
Traditional Osteoarthritis management strategies for joint degeneration have focused primarily on symptomatic relief rather than addressing the root cause of the structural damage. Current protocols typically begin with conservative measures such as physical therapy, weight management, and oral analgesics like non-steroidal anti-inflammatory drugs. While these can provide temporary comfort, they do not halt disease progression and are often associated with systemic side effects, including gastrointestinal issues and cardiovascular risks. When pharmacological interventions fail, intra articular injections of corticosteroids or hyaluronic acid are frequently utilized. However, the efficacy of these injections is often short lived and does not facilitate tissue restoration. The final resort is usually total joint replacement surgery, which is invasive, requires extensive rehabilitation, and carries risks of infection or prosthetic failure, leaving a significant Osteoarthritis therapeutic gap for those seeking non-surgical alternatives.
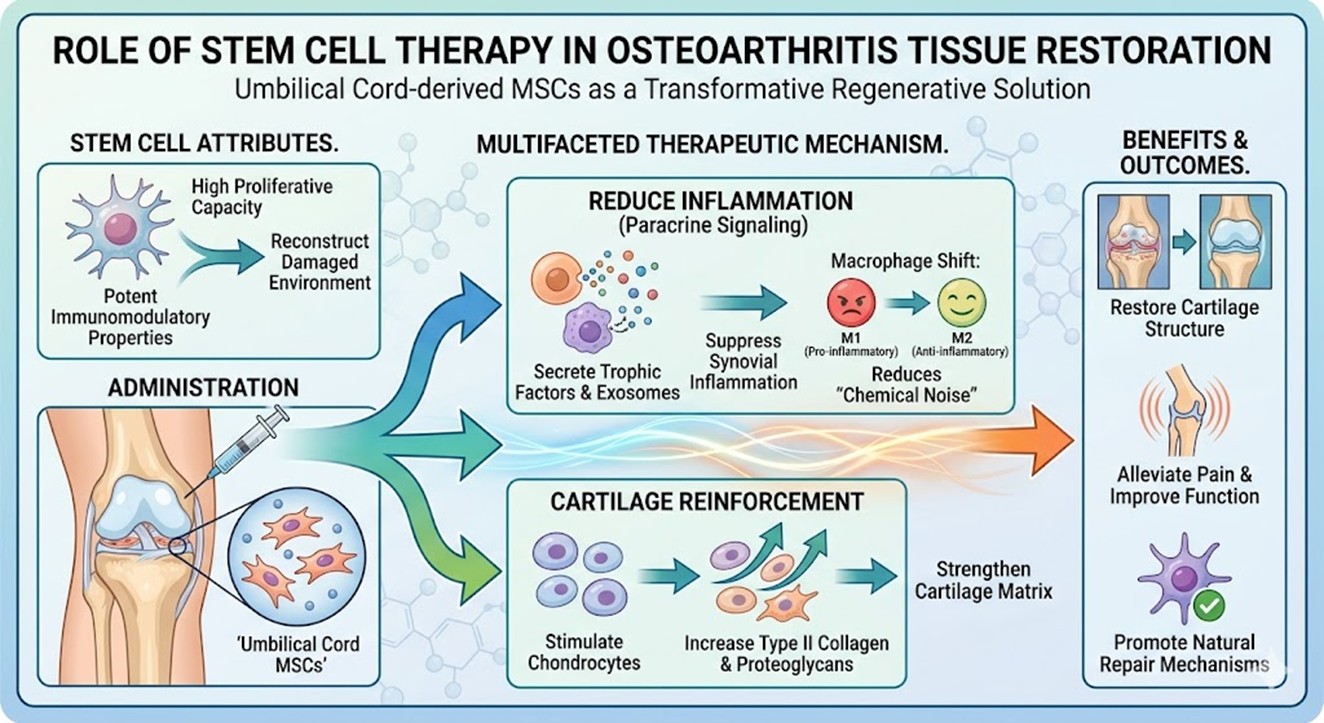
- The Role of Stem Cell Therapy in Tissue Restoration of Osteoarthritis
This is where the application of umbilical cord derived mesenchymal stem cells becomes a transformative solution within the field of Regenerative Medicine. Unlike traditional methods, Stem Cell Therapy aims to reconstruct the damaged biological environment. These specific cells are chosen for their high proliferative capacity and potent immunomodulatory properties. The therapeutic Osteoarthritis mechanism is multifaceted, involving both direct differentiation and paracrine signaling. Once introduced into the joint space, these cells secrete a variety of trophic factors and exosomes that suppress the inflammatory response of the synovium. More importantly, they help modulate the activity of macrophages, shifting them from a pro inflammatory M1 phenotype to an anti-inflammatory M2 phenotype. This shift reduces the chemical noise in the joint, allowing the body’s natural repair mechanisms to function more effectively. Furthermore, these Stem Cells can stimulate local chondrocytes to increase the production of type II collagen and proteoglycans, effectively reinforcing the cartilage matrix.
- Future Prospects of MSCs in Thailand
The potential for utilizing these advanced cellular therapies in Thailand has grown significantly due to the country’s robust medical infrastructure and its emergence as a global hub for biotechnology. Thailand offers a unique combination of world class laboratory facilities and specialized medical expertise, making it an ideal destination for Osteoarthritis patients seeking cutting edge treatments. The regulatory environment in the country is increasingly supportive of clinical research involving cell-based products, ensuring that safety standards are strictly maintained while fostering innovation. Moreover, the integration of Stem Cell Therapy into the broader medical tourism sector allows for a seamless patient experience that combines high quality clinical care with holistic recovery. As research continues to validate the long-term benefits of these treatments, the nation is positioned to lead the region in establishing standardized protocols for regenerative orthopedics.
- Conclusion and Clinical Outlook
The transition from palliative care to restorative science represents a major leap forward in managing musculoskeletal health. By focusing on the biological restoration of the joint through Stem Cell Therapy, medical professionals can offer patients a chance to regain mobility without the trauma of major surgery. The sophisticated interplay between immunomodulation and tissue engineering provided by Regenerative Medicine offers a promising pathway for those who have found little success with conventional treatments. As the medical community in Thailand continues to refine these techniques, the future of Osteoarthritis care looks increasingly focused on biological longevity and the preservation of natural joint function. This shift not only promises better clinical outcomes but also a significant improvement in the overall wellbeing of the global aging population.

