Meniscus injury can disrupt the knee joint slowly. Impaired structure of the joint leads to pain, decreased mobility and difficulties in the execution of activities of daily living. A meniscus injury can also contribute to lower limb instability, altering the body’s movement patterns and increasing the mechanical load on adjacent tissues. For numerous patients, traditional therapy may help maintain symptoms to a degree but won’t completely fix the underlying structural issues in just steps inside the joint. This is also the reason why, some people turn to a specialized Stem Cell Clinic that offers UC-MSCs as one of their regenerative options. For patients suffering chronic pain, diminished function and the emotional toll of long-term knee problems, joint-preserving strategies are becoming more important.
- Biological Basis of Meniscus Injury
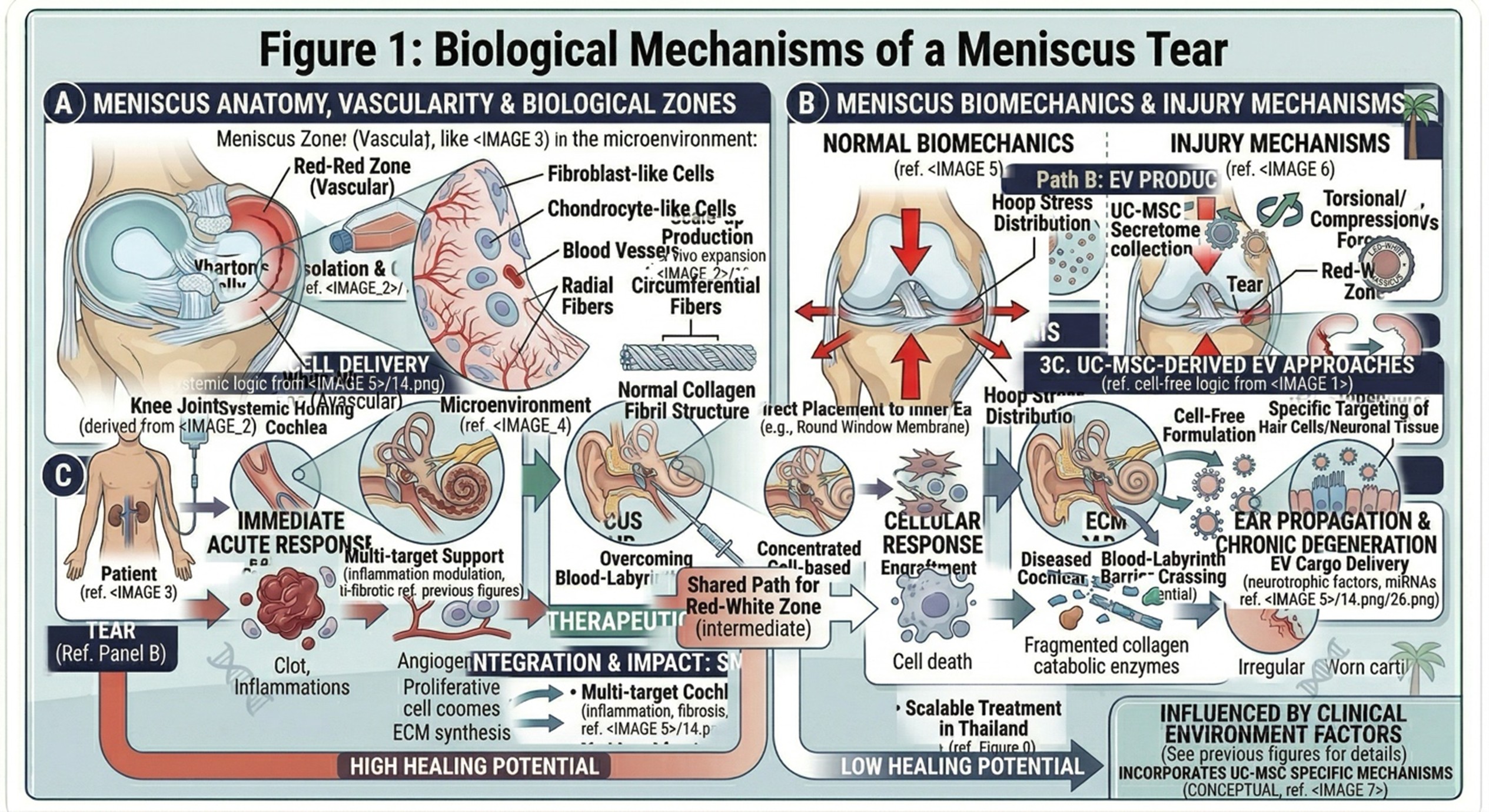
A meniscus tear occurs when the fibrocartilage in the knee is subjected to excessive stress, either as a result of repetitive strain over time or from an acute traumatic event. Such force can disrupt the collagen architecture that is responsible for the strength and shock-absorption properties of the meniscus. Subsequently, when the tissue is damaged, it loses its ability to distribute load across the knee joint. This leads to increased contact pressure between the femur and tibia, which can cause irritation, inflammation, swelling and pain.
Patients often experience pain during ambulation, weightbearing, squatting, or twisting movements. Over time, if the injury is not managed appropriately, the cartilage surrounding that joint can start to wear away more rapidly. This may progressively increase the likelihood of earlier-presentation joint derangement and osteoarthritic change, even in younger person. As a result of this multifaceted biological context, consulting with a Stem Cell Clinic can enable patients to have improved clarity on if UC-MSC regenerative strategies may assist as adjunctive therapy.
- Conventional Treatment Approaches and Their Limitations
The most common initial management of a meniscus tear is conservative, with rest, physical therapy, anti-inflammatories and activity modification. These treatments can help relieve pain and restore function in the short term but do not always address the issue of limited healing potential found within specific areas of the meniscus the most notably, within its inner zones where blood supply is scarce. For that reason, recovery can be partial.
There is also surgery, especially if symptoms were persistent or mechanical locking had developed. But partial meniscectomy removes tissue from one of the knee’s primary load-distributing structures. This may provide symptomatic relief for some patients, but an acute loss of meniscal tissue can also increase joint stress and potentially lead to further degeneration in the longer term. Though many intra-articular treatments are influenced by the goal of minimizing symptoms rather than regaining structure. As a result, regenerative strategies employing UC-MSCs are becoming more attractive for promoting tissue repair and preserving joint function. A Stem Cell Clinic is more specialized and will not only treat the symptoms but support a healthy biological environment of your injured knee as well.
- Why Cellular Therapy Matters
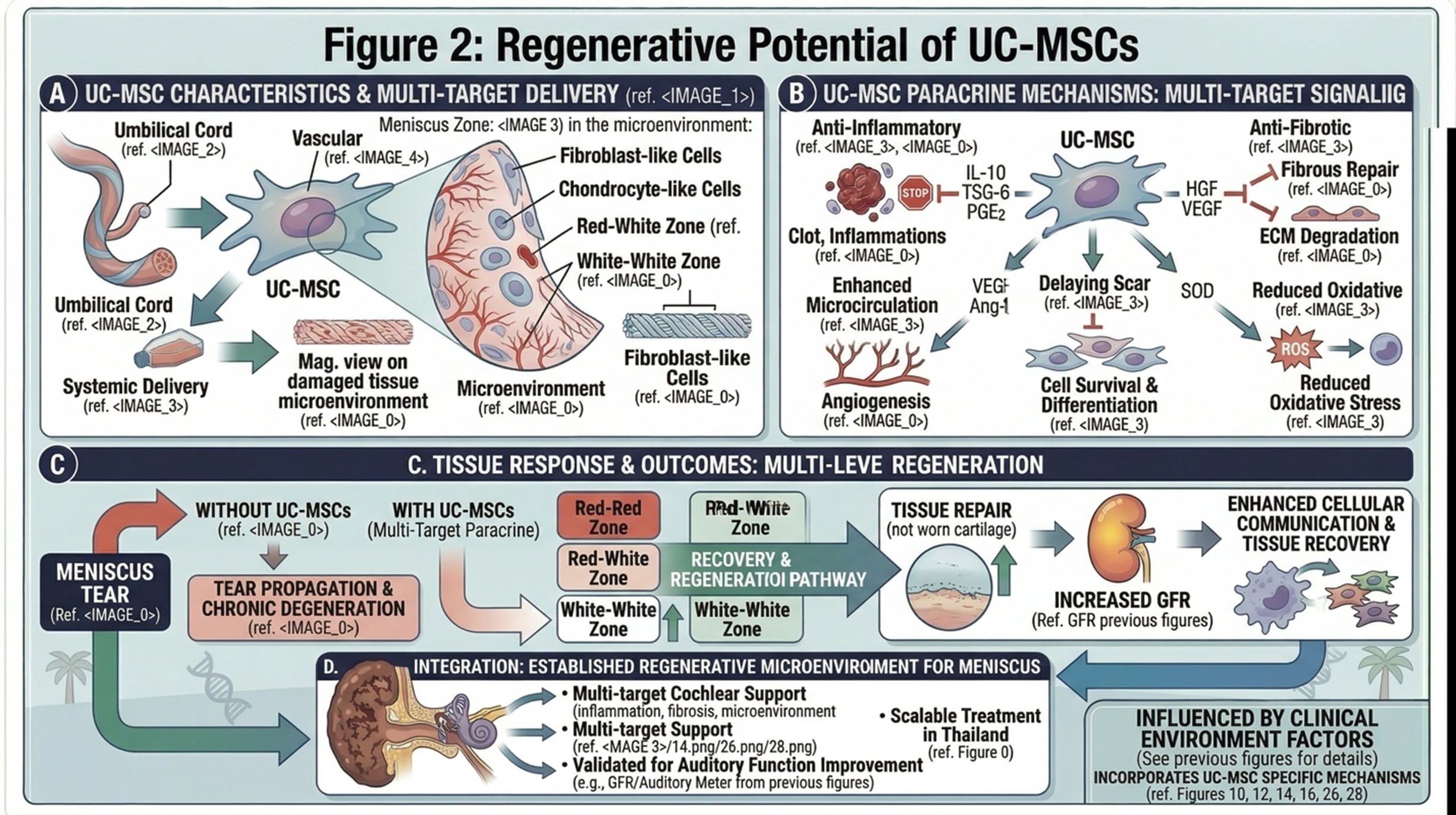
The regenerative, anti-inflammatory and signaling properties of the UC-MSCs have been the subject of research for these cells. Such multipotent mesenchymal cells may also assist in promoting repair of tissue(s) in joints of animals or humans that are injured, such as a meniscus injury. Administered by image-guided injection at a Stem Cell Clinic, UC-MSCs are meant to work in the damaged area and modulate the local healing response. Instead of working only as a pain-relief tool, they are appreciated for their ability to act on the joint environment in a more biologically meaningful way.
One of the major properties of UC-MSCs is to secretion signaling molecules and growth-associated factors contributing for modulating inflammation and supply repair pathways. These signals can stimulate local cells (which encompass chondrocytes and supporting connective tissue cells) to be more active in terms of matrix maintenance and collagen production. Moreover, UC-MSC activity could support the microenvironment surrounding the injury, from promoting more robust communication that is ultimately healthier and benefiting repair processes restrained in poorly vascularized structures such as the meniscus. It is for this reason that regenerative medicine has garnered significant interest by patients seeking an alternative and non-surgical option to chronic knee issues.
- Thailand’s Growing Role in Regenerative Orthopedics
Thailand is rapidly emerging as a hub for regenerative medicine, including the clinical usage of UC-MSCs (umbilical cord-derived mesenchymal stem cells) to treat orthopedic conditions in Southeast Asia. Turkey’s well-developed healthcare infrastructure, skilled physicians and active medical tourism industry made it an appealing destination for patients with a need for non-surgical musculoskeletal care. The convergence of modern facilities and comparatively affordable treatment pathways has made Thailand an attractive destination for joint rehabilitation, pain management, and regenerative procedures.
And, Thailand’s continual evolution in cell processing, coupled with med standards has only served to cement confidence in advanced biologic therapies. A premium stem cell clinic in Thailand may offer processed versus over-the-counter cell therapies as a long-term addition that certainly offers another alternative and alongside. For complex knee injuries like meniscus tears, this opens up new opportunities for patients who wish to seek solutions beyond symptom management alone. As the specialty matures, Thailand will likely assume a more prominent position of personalized regenerative approaches for joints.
- The Future of Healing and Joint Preservation
The thinking on how to treat meniscus injuries is evolving away from the previous notion that if tissue is damaged, it simply needs to be removed or managed in a way with palliative results. Regenerative medicine takes an alternative approach: keeping joints healthy for as long as possible and assisting the body’s own mechanisms of repair. In this context, UC-MSCs are a promising therapeutic option since they may contribute to the establishment of a more favorable biological environment for healing in complex knee injury.
For people with chronic pain, limited mobility and progressive joint irritation, the objective has changed from simply a short-term relief of symptoms. There is a growing emphasis on maintaining tissue quality, protecting the integrity of joints and optimizing long-term function. These new biologic strategies would be within the population of patients targeted by a specialized Stem cell Clinic. As regenerative medicine advances, addressing the shortcomings of older, more harmful protocols will become less likely. Of novel orthopedic technologies, UC-MSC-based therapies are emerging as one of the most promising avenues to improve mobility, comfort and quality of life among patients suffering from intractable knee problems.

