The Habits and Signs That Often Come Before a CKD Diagnosis
- When the kidneys start struggling, the body usually gives hints
Most people do not think about their kidneys until something feels off. The problem is that the early signs of CKD can look ordinary enough to ignore. Years of poorly controlled diabetes, high blood pressure that is never fully managed, too much sodium, too little follow-up, and long periods of assuming “I feel fine, so I must be fine” are some of the patterns most often seen before chronic kidney disease is found. Diabetes and high blood pressure remain the two leading causes of CKD in adults, and the sooner kidney disease is identified, the sooner treatment can begin.
With subtle symptoms initially being the reason behind going for testing, there are many manifestations: foamy urine, swollen ankles, puffiness around the eyes, fatigue, poor appetite, itching, changes in urination, and so on. However, the most important thing is not to just monitor symptoms of kidney failure, but to find a way to treat it! Kidney societies, clinical guidelines, and leaders are urging continued reliance on urine and blood tests. They recommend these tests specifically for people who have diabetes mellitus, high blood pressure, a heart problem, or those with a family history of developing renal failure.
Why CKD Becomes So Difficult to Reverse?
- The damage is not just about filtering less
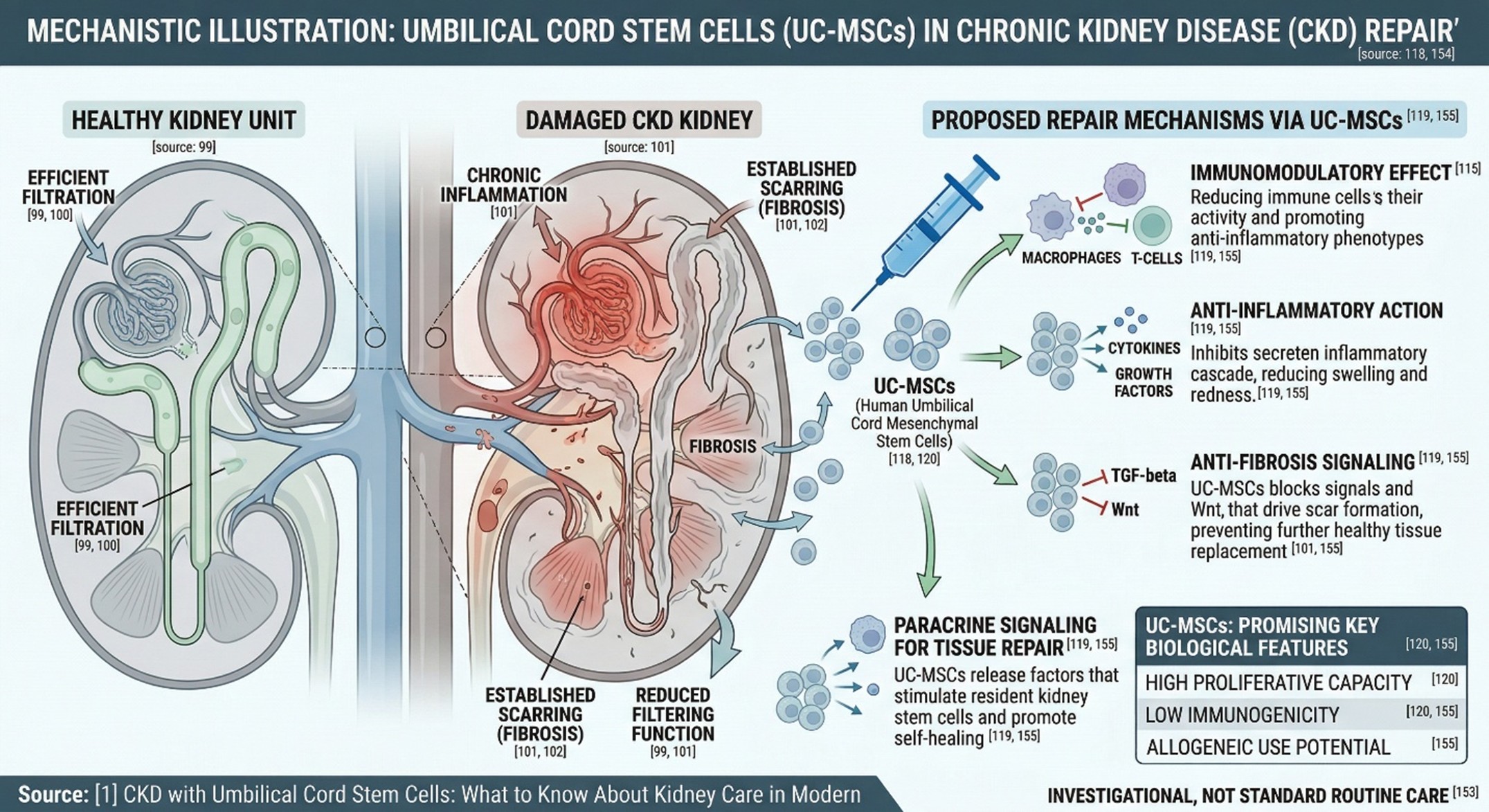
In CKD, the kidney’s filtering units and supporting blood vessels are repeatedly injured over time. High blood glucose can damage the filters. High blood pressure can damage the blood vessels and filtration system even further. Once that process keeps going, inflammation and fibrosis begin to replace healthy kidney tissue, and that is when the disease becomes much harder to reverse. This is why kidney disease is treated as a progressive problem: once scarring becomes established, slowing decline is often more realistic than undoing damage completely.
Where Standard CKD Treatment Comes First
- Before anyone talks about a stem cell clinic
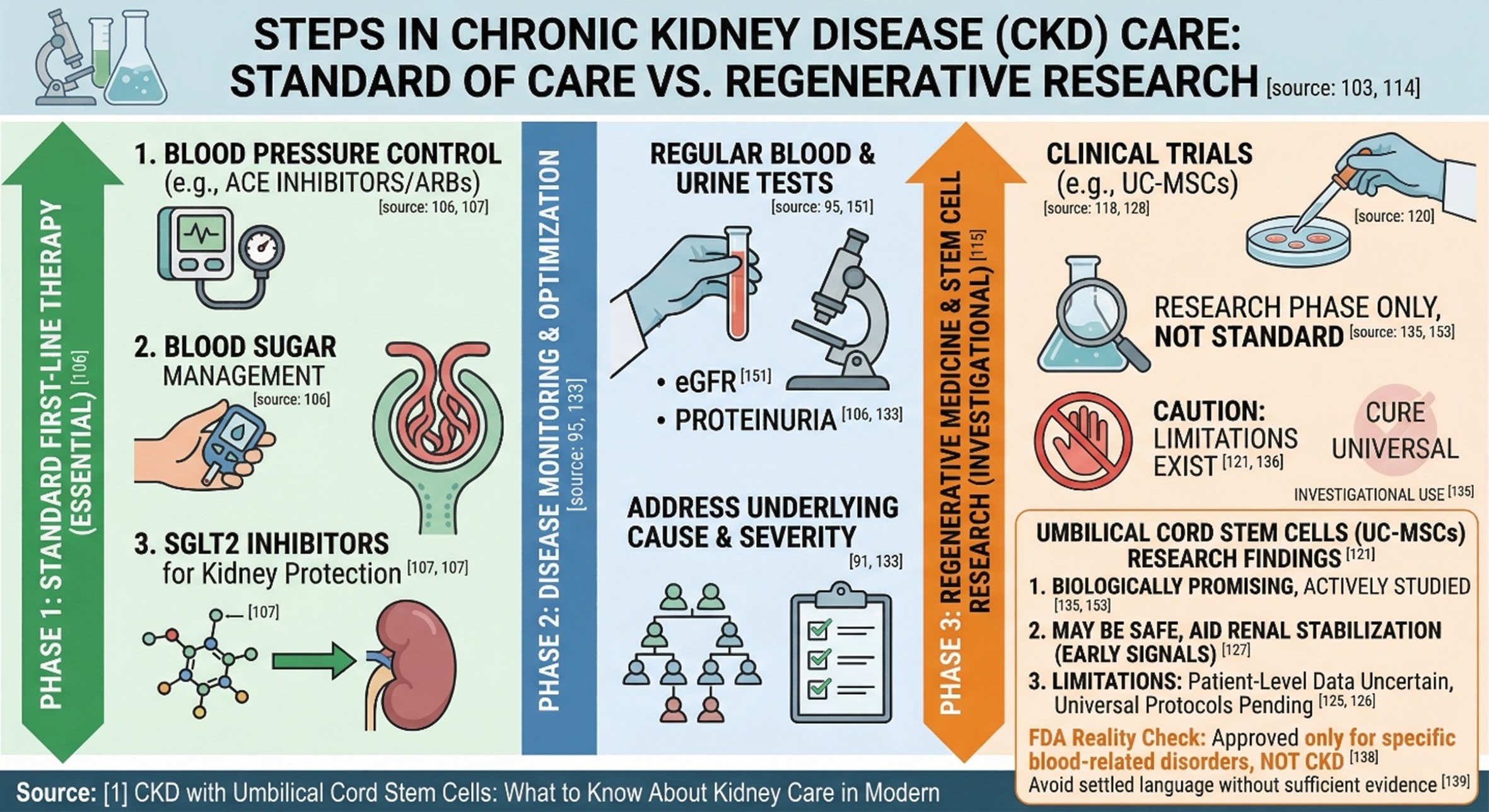
This is the part that should never be skipped. And at present, there are no alternative therapies; it makes sense initially to go for standard treatments. People with CKD today are first of all going to have their blood pressure controlled, then they are going to have their blood sugar tightly controlled, and protein forced out of their urine. Alongside taking medication such as ACE inhibitors or ARBs to protect the kidneys, nowadays SGLT2 inhibitors are increasingly being used as adjunct treatment to delay progression of the disease and minimize cardiovascular complications. When renal function falls far enough, dialysis or kidney transplantation may be needed. Since that is the case, most people do not get started from a stem cell clinic. The vector for them is the protection of the kidneys based on evidence and discovery science.
- Why do people still keep searching for more
Even with better standard care, many patients eventually start looking for something more restorative. That is why searches for stem cell clinics, CKD, and umbilical cord stem cells keep growing. The underlying question is understandable: if modern medicine can slow kidney decline, could regenerative medicine eventually help support repair as well? That is where the research gets interesting.
What Umbilical Cord Stem Cells Actually Are
- Why does this source get so much attention
When scientists discuss using umbilical cord stem cells to get at a cure for kidney disease, they’re usually speaking of those derived from mesenchymal cells, referred to as UC-MSCs. But they do not originate as kidney cells. These cells are appealing because they look to behave more than just simply replacing damaged tissue, immunomodulatory, anti-inflammatory, and carry paracrine signaling effects into the damaged kidney environment, shedding light on how diseases progress. In addition, reviews published recently find that umbilical cord-derived MSCs may have high proliferative capacity and a relatively low immunogenicity, which would help to explain why they are at the forefront of so many research efforts at present.
What the Research Says About Umbilical Cord Stem Cells in CKD
- The strongest message right now is “promising, but not routine.”
The topic where it truly gets interesting is over here. A 2025 update on stem cell use around the world for CKD stated that clinical trials associated with mesenchymal cells keep increasing, causing major overseas interest in some form of MSC treatment for chronic kidney disease. Another separate 2025 report also mentioned that mesenchymal stem cells had a beneficial effect on inflammation and renal function in CKD animal models, though patient-level data remained less certain. This is a key difference. The biological signal is strong enough to sustain this level of activity, but it has not yet reached the certainty needed for a universal protocol.
Monotherapy, there are also early human signals worth heeding. A 2025 paper reportedly showed that transplanting human umbilical cord stem cells into CKD patients with stage 3–4 renal insufficiency was safe and might ease their fall of kidney function as well. Ongoing trials are also assessing discrete intravenous and even meso-renal methods. That does not mean a stem cell clinic can truthfully claim UC-MSC treatment as established routine care for any CKD sufferer. However, it does mean the topic has moved from being merely speculative to reaching a serious phase in clinical trials.
- Good medicine is still about selection and honesty
A responsible stem cell clinic should not begin by giving false hope, but by making an accurate diagnosis, kidney stage, rate of decline, proteinuria, underlying cause, and whether proven discussed, consider which treatment method to choose, and what the current evidence actually shows. To summarize for now: umbilical cord stem cells are biologically promising and actively studied in CKD, but they are still in the research phase before they can be considered a widely accepted treatment method.
Why caution still matters??
That caution is not negativity. It is simply part of reading the field correctly. FDA guidance still makes clear that approved stem cell products are limited to blood-forming stem cells from umbilical cord blood for certain blood-related disorders, not for general conditions like CKD. So anyone exploring a stem cell clinic for kidney disease should separate serious research from language that sounds more settled than the evidence really is.
Final Thoughts
*The reason is quite obvious, which is that this topic just keeps on growing. CKD is common, progressive, and often found only after damage has been certain is a fact. Standard treatment can slow the disease down, but it cannot stop established fibrosis from accumulating further. That is why umbilical cord stem cells have become such a hot research topic and why ordinary treatment begins to feel only half a measure less than perfect. That’s why more people begin looking for a stem cell clinic. Today, the most realistic portrayal of science is optimistic yet cautious: The industry keeps moving, the biological inspiration is intriguing, and experimental data are promising. However, everyday kidney care with consistent evidence-based knowledge that stands the test of history still stands as a rule for first-line therapy.
*FAQ: Stem Cell Clinic, CKD, and Umbilical Cord Stem Cells
- What are the most common warning signs of CKD?
Common warning signs include foamy urine, swelling, fatigue, itching, appetite changes, and changes in urination. But CKD is confirmed with blood and urine testing, not symptoms alone.
- Are umbilical cord stem cells already a standard treatment for CKD?
No. Umbilical cord stem cells are being actively studied, and early findings are encouraging, but the treatment is still investigational rather than standard routine care.
- Why are umbilical cord stem cells so interesting in kidney research?
Researchers are interested in them because they may help influence inflammation, fibrosis, and tissue-repair signaling, and because they have practical biological features that make them attractive for allogeneic use.
- What should a stem cell clinic explain clearly to a CKD patient?
A stem cell clinic should explain disease stage, probable cause, what standard therapies have been used, what type of cells are proposed, and what remains uncertain in the evidence.