Toe ulcers due to diabetes mellitus are among the most difficult complications of DM. Wounds like these — which can start small but become serious after healing mechanisms are compromised. If not treated or poorly managed, they can lead to infection and tissue death, even amputation in severe cases. Despite advances in conventional care many diabetic ulcers remain resistant to treatment. This has led to growing interest in regenerative medicine—particularly umbilical cord-derived mesenchymal stem cell (UC-MSC) therapy—as a promising approach to enhance healing and preserve tissue.
The Nature of Diabetic Toe Ulcers
One of the primary contributors is peripheral neuropathy, a condition that reduces sensation in the feet and toes. Because patients may not feel pain or discomfort, minor injuries such as cuts, blisters, or pressure sores often go unnoticed and untreated.
Diabetes can damage blood vessels, limiting the flow of oxygen and nutrients necessary for tissue repair. At the same time, the immune system may be weakened, reducing the body’s ability to fight infection. Elevated blood glucose levels further complicate healing by interfering with normal cellular processes and increasing inflammation.
Together, these factors create an environment where wounds struggle to heal. Even with standard treatments—ulcers may persist or worsen, highlighting the need for more advanced therapeutic options.
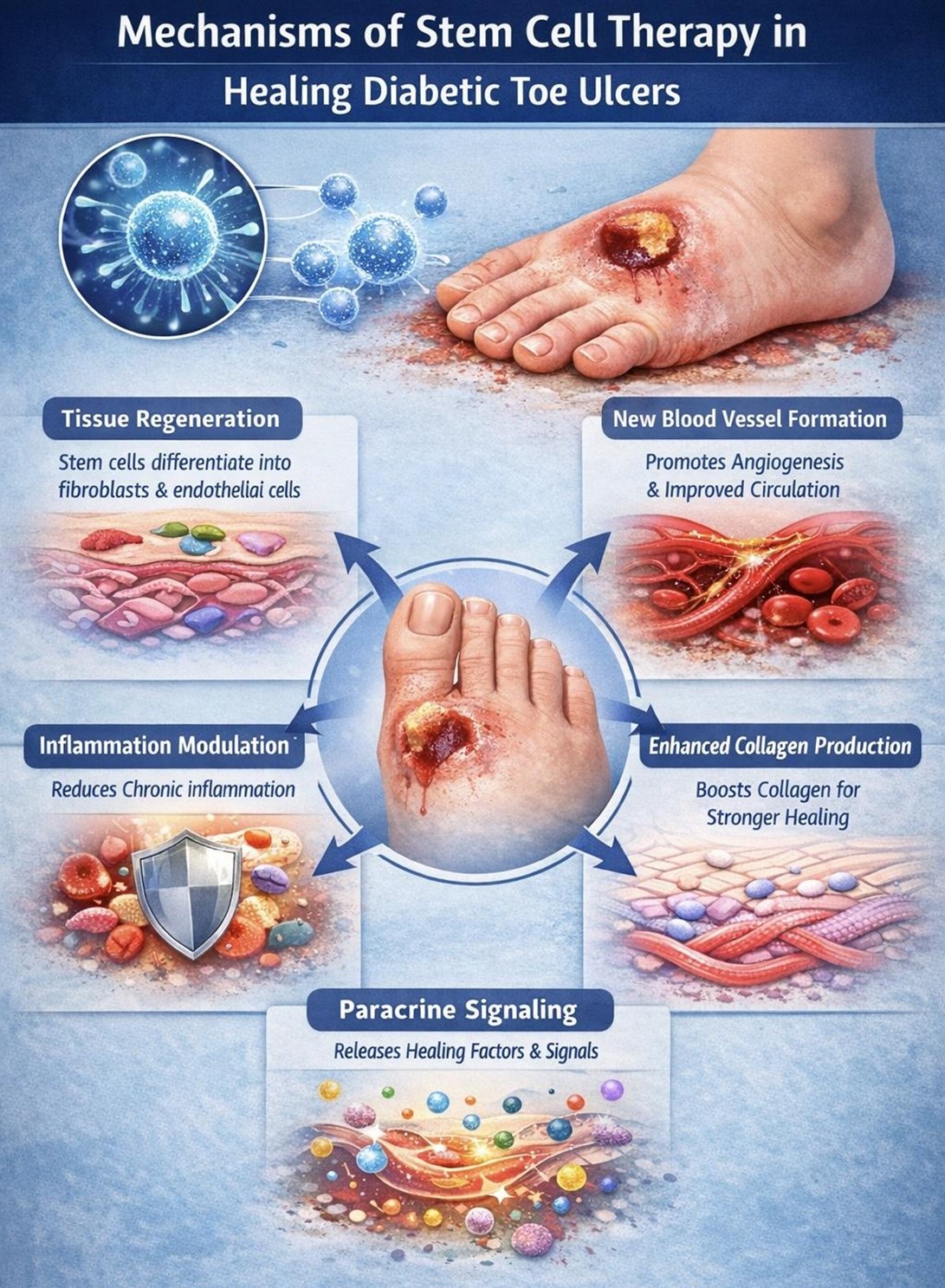
Mechanisms of Stem Cell Therapy Support Diabetic Toe Ulcers Healing
- Regeneration of Damaged Tissue
Stem cells can differentiate into essential cell types involved in skin repair, including fibroblasts and endothelial cells. Fibroblasts are responsible for producing collagen and structural proteins, while endothelial cells contribute to the formation of blood vessels. By replenishing these critical components, stem cells help rebuild damaged tissue and restore skin integrity.
- Formation of New Blood Vessels
One of the major barriers to healing in diabetic ulcers is inadequate blood supply. Stem cells promote angiogenesis, the process of forming new blood vessels, by releasing growth factors such as vascular endothelial growth factor (VEGF). Improved circulation allows oxygen and nutrients to reach the wound more effectively, accelerating tissue repair and reducing the risk of complications.
- Modulation of Inflammation
Chronic inflammation is a hallmark of diabetic wounds and can significantly delay healing. Stem cells help regulate the immune response by reducing excessive inflammatory signals and promoting anti-inflammatory pathways. This creates a more balanced environment that supports tissue regeneration rather than further damage.
- Enhanced Collagen Production
Collagen is essential for wound closure and strength. Stem cells stimulate the production and organization of collagen fibers, leading to stronger and more resilient tissue. This also helps improve the overall quality of healing and reduces the likelihood of wound recurrence.
- Paracrine Effects and Cellular Communication
Beyond direct tissue replacement, stem cells release a wide range of signaling molecules, including growth factors, exosomes, and microRNAs. These substances influence nearby cells, encouraging them to participate in the healing process. This indirect mechanism amplifies the body’s natural repair response and contributes to more efficient recovery.
Methods of Delivering Stem Cell Therapy for Diabetic Toe Ulcers
- Topical application: Stem cells are incorporated into gels or dressings and applied directly to the wound surface, providing localized healing effects.
- Injection therapy: Cells are injected around or into the ulcer to target deeper tissue layers and stimulate regeneration from within.
- Scaffold-based systems: Stem cells are delivered using biocompatible materials that support their survival and prolong their activity at the wound
- Intravenous infusion: Although less targeted, systemic delivery may improve overall circulation and immune function, indirectly supporting wound
Evidence Supporting Stem Cell Therapy
Clinical research has demonstrated encouraging outcomes for stem cell therapy in diabetic wound care. Studies involving mesenchymal stem cells have reported faster wound closure, improved tissue quality, and reduced recurrence rates compared to standard treatments alone. In some trials, patients with chronic ulcers experienced complete healing within weeks after receiving stem cell therapy.
These findings suggest that regenerative medicine can play a significant role in addressing wounds that do not respond to conventional care, offering new hope for patients at risk of severe complications.
Several Benefits of Stem Cell Therapy for Diabetic Toe Ulcers
- Accelerated Healing: By enhancing cellular regeneration and blood flow, wounds can close more quickly.
- Reduced Risk of Amputation: Early and effective treatment may help preserve affected limbs.
- Lower Complication Rates: Improved immune regulation decreases the likelihood of infection.
- Minimal Adverse Effects: Stem cells are generally well-tolerated, with a low risk of immune rejection.
- Improved Quality of Life: Faster recovery leads to reduced pain, better mobility, and greater independence.
Thailand’s Growing Role in Regenerative Medicine
Thailand has become a recognized leader in stem cell therapy, offering advanced treatment options supported by modern medical infrastructure and skilled healthcare professionals. Many clinics specialize in regenerative medicine and provide personalized care plans tailored to each patient’s needs.
In addition to high-quality services, Thailand is known for its accessibility and affordability, attracting patients from around the world. The country’s commitment to innovation and patient-centered care continues to drive progress in the field of regenerative medicine, particularly in the treatment of chronic conditions like diabetic ulcers.
A Promising Future for Diabetic Wound Care
Stem cell therapy represents a significant advancement in the treatment of diabetic toe ulcers. By targeting the underlying causes of poor healing—such as impaired circulation, chronic inflammation, and tissue damage—this approach goes beyond traditional methods that focus solely on symptom management.
As research continues to evolve, stem cell therapy is expected to become an integral part of modern wound care. For patients struggling with persistent diabetic ulcers, especially those at risk of serious complications, this regenerative approach offers a promising pathway toward faster healing, reduced risks, and improved overall health.
In Thailand, where innovation in medical science is rapidly advancing, stem cell therapy is opening new possibilities for restoring tissue health and transforming outcomes for individuals living with diabetes-related wounds.

