Advances in regenerative medicine are transforming many areas of healthcare, including reproductive medicine. One emerging area of research involves the use of stem cells to help restore ovarian function in women experiencing fertility challenges. Ovarian rejuvenation through stem cell therapy is an experimental yet promising approach designed to support women who face infertility due to aging, premature ovarian insufficiency (POI), or the natural transition into menopause. By utilizing the regenerative abilities of stem cells, scientists and clinicians hope to repair or revitalize ovarian tissue and improve the reproductive environment.
For many women, declining fertility can be emotionally and physically challenging. Traditional fertility treatments such as hormone therapy or in vitro fertilization (IVF) may help in some cases, but their effectiveness can be limited when ovarian reserve is significantly reduced. Regenerative therapies using umbilical cord–derived mesenchymal stem cells (UC-MSCs) are now being explored as a potential way to enhance ovarian function and create new possibilities for women seeking to conceive.
Understanding Ovarian Aging and Fertility Decline
Female fertility naturally decreases with age. Females are born with a limited number of eggs, and this reserve naturally decreases as they age. As women reach their mid-30s and beyond, both the number and quality of eggs typically decrease. This reduction in ovarian reserve can make conception more difficult and increase the likelihood of reproductive complications.
Hormonal changes also play a significant role in fertility decline. Hormones such as estrogen and anti-Müllerian hormone (AMH) are closely associated with ovarian function. As ovarian reserve diminishes, levels of these hormones often decrease as well, which can affect ovulation and menstrual regularity.
For some women, ovarian decline occurs earlier than expected due to a condition known as premature ovarian insufficiency. Premature ovarian insufficiency (POI) happens when the ovaries stop functioning normally before a woman reaches 40 years of age. This condition may be linked to genetic abnormalities, autoimmune disorders, or medical treatments such as chemotherapy or radiation therapy. Women with POI often experience irregular or absent menstrual cycles and may face significant challenges when attempting to conceive.
In situations where ovarian function is severely reduced, conventional fertility treatments may not provide sufficient results. This has led researchers to explore regenerative strategies, including stem cell therapy, as a potential way to restore ovarian activity.
How Stem Cells Contribute to Regenerative Medicine
Stem cells are unique biological cells with the remarkable ability to develop into various specialized cell types. Unlike mature cells, stem cells remain unspecialized until they are activated to perform specific functions. They can also replicate themselves, providing a continuous source of regenerative cells.
In regenerative medicine, stem cells are widely studied because of their capacity to repair damaged tissues and support healing processes. Mesenchymal stem cells (MSCs), including those derived from umbilical cord tissue, are particularly valuable due to their anti-inflammatory and regenerative properties.
In addition to their ability to differentiate into various cell types, stem cells release signaling molecules known as growth factors and cytokines. These substances help regulate inflammation, stimulate tissue repair, and encourage the growth of new blood vessels. Through these mechanisms, stem cells can create a more supportive environment for healing and regeneration.
How Stem Cell Therapy May Support Ovarian Function
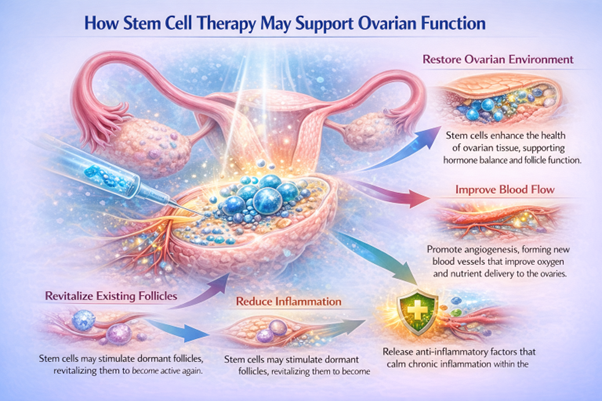
The purpose of stem cell therapy for ovarian rejuvenation is not always to generate entirely new eggs. Instead, the therapy often focuses on improving the ovarian environment so that any remaining follicles can function more effectively. By enhancing the health of ovarian tissue, stem cells may help restore hormonal balance and promote normal reproductive activity.
Once prepared, the stem cells are introduced into the ovaries through minimally invasive procedures. Techniques such as laparoscopic injection or ultrasound-guided transvaginal injection are commonly used to deliver the cells into the ovarian cortex, the outer layer of the ovary where follicles are located.
After being administered, stem cells begin interacting with the surrounding tissue. Rather than directly producing eggs, they release bioactive molecules that support several important regenerative processes.
One of these processes is angiogenesis, or the formation of new blood vessels. Improved blood circulation allows oxygen and nutrients to reach ovarian tissues more effectively, which may help revitalize existing follicles.
Stem cells may also reduce inflammation within the ovaries. Chronic inflammation can disrupt normal ovarian function, so reducing this inflammatory environment may allow healthier tissue activity.
In addition, stem cells can help support the survival and function of existing ovarian cells. Some researchers believe that stem cells may even stimulate dormant follicles—follicles that remain inactive within the ovary—to become active again. If this occurs, it could potentially restore ovulation and improve fertility.
Conclusion
Stem cell–based ovarian rejuvenation represents an exciting and innovative direction in reproductive medicine. By harnessing the regenerative potential of stem cells, this approach aims to restore ovarian function and improve fertility in women facing challenges related to aging, premature ovarian insufficiency, or other medical conditions.
Early research suggests that stem cell therapy may help revive ovarian activity, improve hormone levels, and in some cases even enable natural conception. The main types of stem cells being studied—mesenchymal stem cells and induced pluripotent stem cells—offer unique regenerative mechanisms that may support tissue repair and reproductive function.
As scientific knowledge and technology continue to evolve, stem cell therapy may eventually become an important option for women seeking to restore fertility and hormonal balance.
For many individuals facing limited fertility options, regenerative medicine offers renewed hope. With continued advancements, stem cell therapy could play a transformative role in helping women achieve their reproductive goals and improve overall reproductive health.

