A common misconception is that Parkinson’s disease (PD) primarily affects the older population
Parkinsons disease is much more than just a movement disorder,This means it is a highly variable degeneration in brain neurodegenerative and progressive neurological condition which can impact the bowel, bladder ability to walk, coordinate move balance improve sleep facial expression mood cognition, memory and independence. With the condition many patients will observe tremor, slowness or stiffness but later in the disease process it affects walking, posture, fine motor control and carrying out everyday activities.
The burden of disease is both physical and emotional for many patients. Less mobility can reduce ability to work, travel, exercise and socialize. Then there are those miserable non-motor symptoms, like tiredness, erratic sleep behaviour, depression and anxiety, constipation or cognitive decline; all undoubtedly no less disturbing than tremor or rigidity. The disease has an impact not only on the patient, but also the caregiver and family since personal care needs increase over time.
That’s one reason why, toward the end of October 2023, researchers are still searching for solutions outside of symptom-control medication alone. Standard of care is still indispensable, but there remains an evolving interest as to whether regenerative and immunomodulatory approaches could help selected patients in the future.
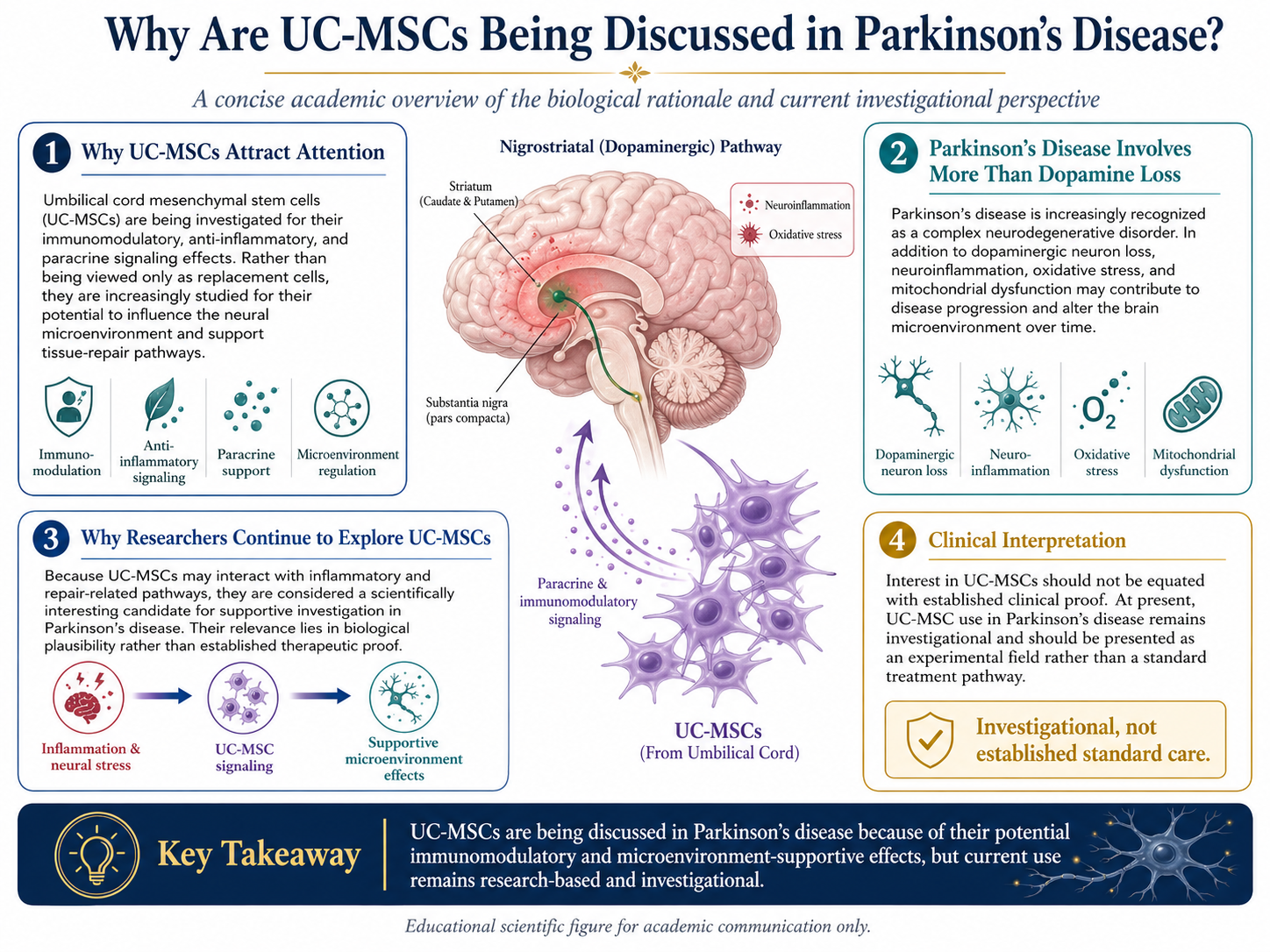
Why is UC-MSCs being discussed in Parkinson’s disease?
Umbilical cord mesenchymal stem cells (UC-MSCs) are being considered as potential treatment options for Parkinson’s disease due to their immunomodulatory, paracrine signaling and anti-inflammatory effects. In contrast to being perceived merely as replacement cells, UC-MSCs are increasingly investigated not just in their capacity to differentiate into neural-like cells but also for the potential roles they might take on influencing the neural microenvironment or mediating immunomodulatory and tissue repair pathways.
Parkinsons is recognized as a disease that extends beyond loss to dopamine alone. In addition to a direct contribution to neurodegenerative disease pathology, neuroinflammation, oxidative stress and mitochondrial dysfunction can further evolve and alter the microenvironment in which the brain exists over time. This makes UC-MSCs an interesting candidate for a potentially supportive therapy in the research cont.
However, interest in UC-MSCs should not be equated with established clinical proof. Currently, this is an experimental field more than a guided standard treatment course.
What Problems Do Parkinson Patients Usually Want to Improve
The majority of patients seeking advanced therapies wish to alleviate the symptoms that have the most immediate impact on function and independence. These can be reduced walking, rigid paralysis in muscles, balance problems, shaking hands and freezing episodes defined as moments of stalled or hurried motion – commonly associated with fatigue and issues performing hand tasks. That said, for some patients the issue of posture, gait confidence and whether they will continue without help to be able to perform basic self-care matters a lot.
Some are, more or less, the quality-of-life people. When motor symptoms are still moderate, however, the impact of poor sleep and decreased energy or mood is more damaging and can lead to mental slowing, pain and a loss of social participation. Practically, patients rarely ask only if a therapy can change a scan or office lab value. They want to learn if they can be less shaky, more mobile, less stiff or more functional in daily life.
That’s why UC-MSCs discussions used to contain both clinical symptoms and general functional aims.
Post-injection of UC-MSC
Early and experimental evidence primarily drives present-day UC-MSC injection debates in Parkinsons disease. The most tempered description of potential benefits is that investigators are considering if UC-MSCs can provide support to the neural environment that would reduce symptoms or perhaps slow functional decline in some instances.
In addition to those potential mechanisms of action, some common benefit areas that are frequently covered in the literature include decreased neuroinflammatory activity, increased tissue-support signaling, a potential contribution from dopaminergic pathways and even an overall healthy local brain microenvironment. Essentially, it is expected that the benefit will not only be in replacing damaged tissue but also assisting the body in creating a more favorable environment for function.
Among patients, this can often mean improved walking confidence or stiffness, smoother movement (less tremor), more balance (and avoid falls), and endurance and a better sense of daily function. Others also anticipate secondary benefits in sleep, energy, and quality of life. But these possible advantages need to come with a caveat. They at this stage are experimental endpoints and should not be considered validated or uniform results.
Clinical Reality: Investigational. Not standard of care or mandate
The scientific rationale is interesting but this, for now and in our opinion, does not advance UC-MSC therapy for Parkinson’s disease from investigational. Standard Parkinson’s Care is still based on the classical principles of medical management (drugs), rehabilitation, exercise, and supportive multidisciplinary care. These pillars have not yet been replaced by stem-cell-based treatment.
Dose and Injection Schedule
The use of UC-MSC for dosing in the context of Parkinson’s disease remains investigational; therefore, protocols are dependent upon the study design, route of administration, treatment goals and patient condition.
The use of repeat treatment intervals has not been standardized for Parkinson’s disease and longterm retreatment strategies remain as experimental rather than standard clinical practice.
Such a Topic Is Trending with the Reason
Nevertheless, Parkinson and UC-MSCs remain an attractive area of study given the need remains unmet. Patients also continue to seek solutions beyond temporary relief of symptoms. The data you collect is limited to the date you began your research and will only be accurate until 10, 2023 at which time all of the researchers continue looking into various methods of helping with the environment around our brains instead if aiming purely for medication replacement strategies. Hence the role of UC-MSCs in the general dialogue on regenerative neurology.
It is a field to follow because it straddles neuroscience, inflammation research, regenerative medicine and quality of life care. Still, it is most scientifically and most conservatively accurate to describe the therapy as promising, plausible, and experimental.
Final Takeaway
Parkinson’s disease is a debilitating condition, presenting with progressive motor and non-motor symptoms leading to functional disability and reduced quality of life. Because UC-MSCs have immunomodulatory, anti-inflammatory and tissue-supporting properties, they are scientifically interesting in Parkinson’s research.

