Why this topic matters more than it sounds
The person looking for Stem cell and stem cells for Chronic Wound usually has not gone in the mode of searching theory. And they want to escape a wound that has begun behaving not like one. This is particularly true in diabetes, where a minor foot ulcer can rapidly develop into major medical complication given the coexistently occurring damage to nerves, blood supply and wound infection risk (and reduced capacity for repair). According to CDC, nerve injury and poor circulation caused by diabetes leave the foot susceptible to chronic non-healing ulcers which maybe infected.
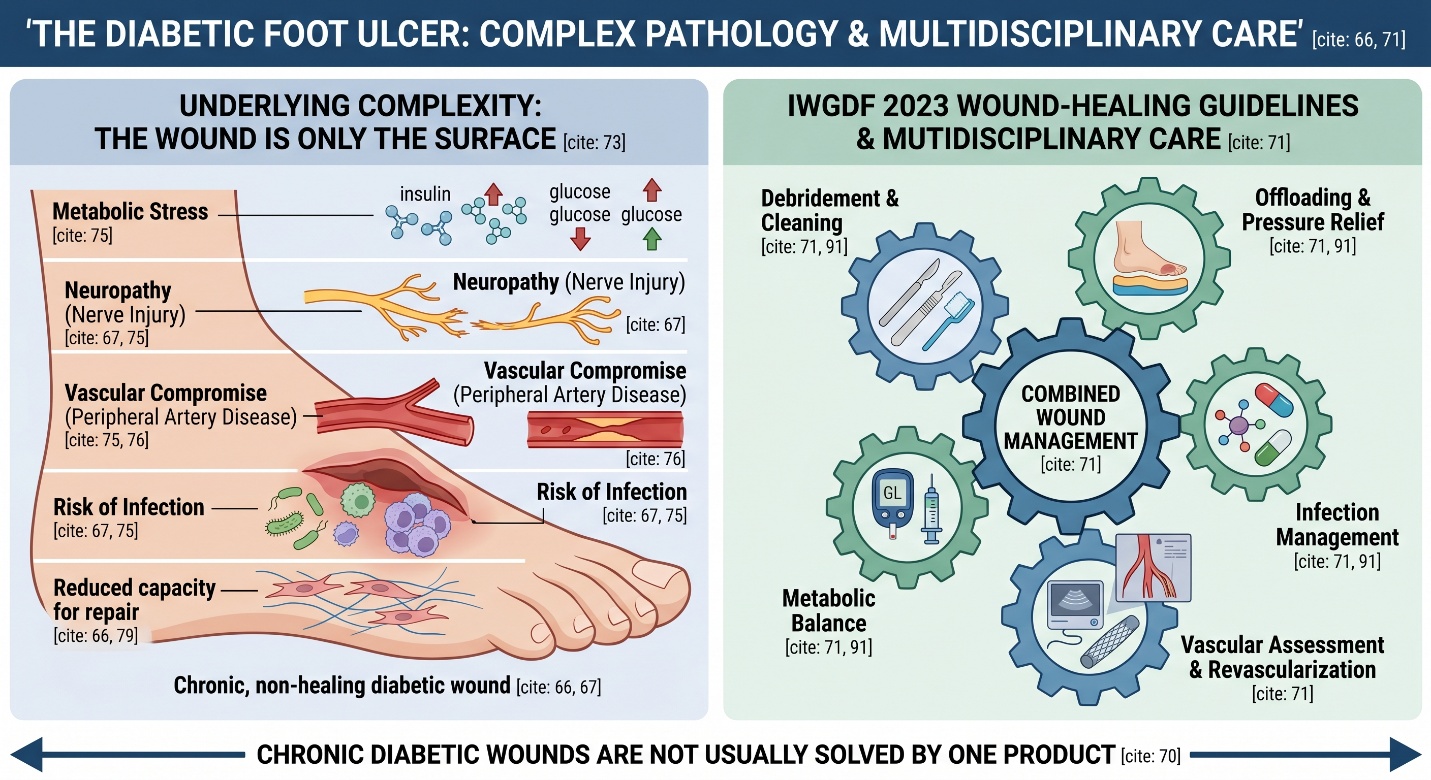
That is also why the phrase diabetes wound curable shows up so often. It reflects a very real fear. But medically, it is not the most useful way to frame the problem. Chronic diabetic wounds are not usually solved by one product or one intervention. The 2023 IWGDF wound-healing guideline emphasizes that wound-healing interventions should be used together with gold-standard multidisciplinary care, while the practical IWGDF guidance continues to center care around debridement, offloading, infection management, vascular assessment, and revascularization when needed.
Why chronic wounds in diabetes are so difficult to heal
The wound is only the surface of the disease
Diabetic foot ulcer has never been just a skin issue. This usually represents a more complex blend of neuropathy, vascular compromise, risk of infection and long-standing metabolic stress. According to the IWGDF peripheral artery disease guideline, up to half of individuals with a foot ulcer have co-existing peripheral artery disease and this has major implications for healing and limb outcomes. Which is why the same wound can appear “tiny” and still act like a life-threatening limb problem.
This is exactly why stem cell research became interesting
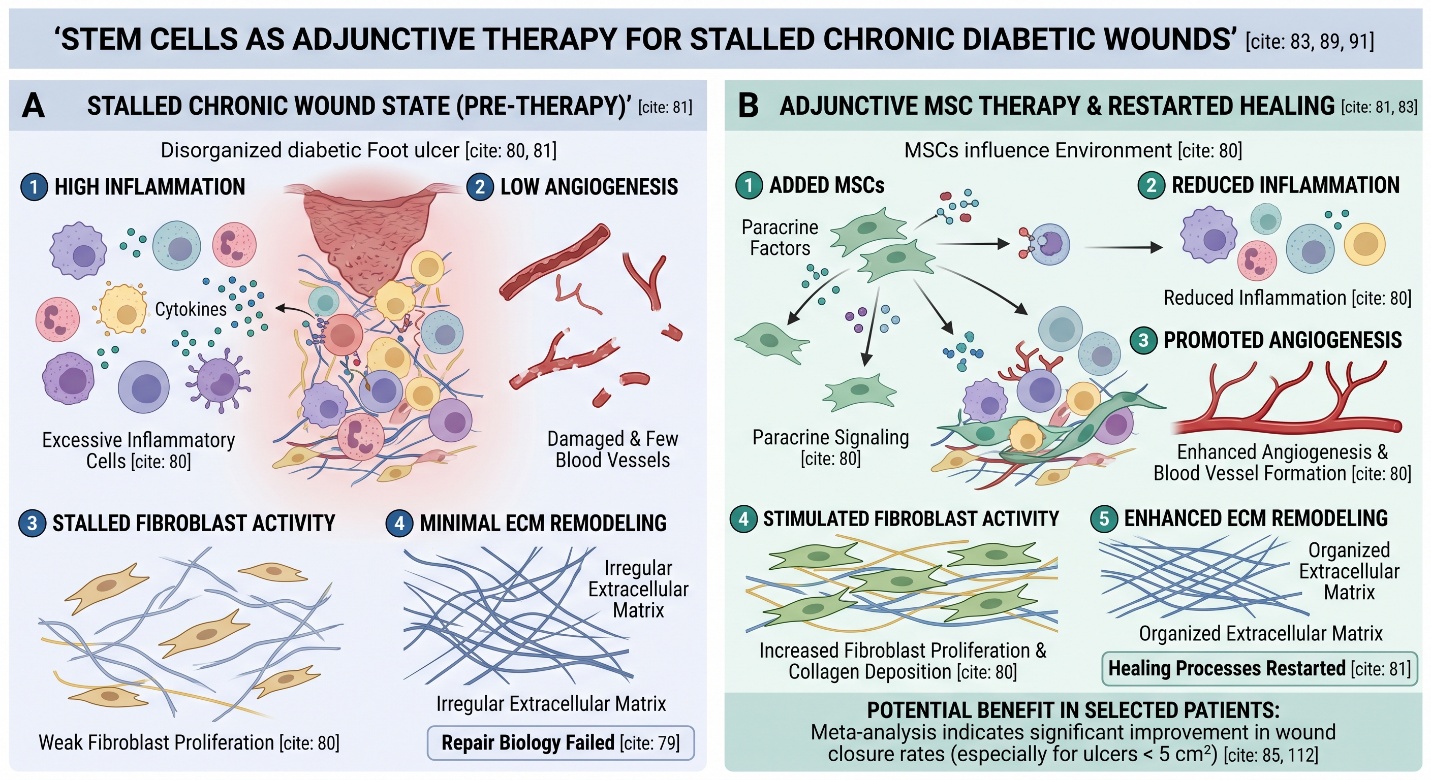
Once wound healing is understood as a failure of repair biology, the interest in Stem Cell therapy makes sense. Reviews published in 2025 describe stem-cell-based strategies for diabetic foot ulcers and limb salvage as promising because they may influence inflammation, angiogenesis, extracellular matrix remodeling, fibroblast activity, and paracrine signaling around the wound. In other words, the appeal is not just that cells sound advanced, but that they may help restart healing processes that have stalled.
Where stem cells for Chronic Wound actually fit
The evidence is real, but it is still adjunctive
This is the part that deserves a plain answer. The evidence is not empty. A 2025 meta-analysis of randomized controlled trials found that mesenchymal stem cell therapy significantly improved wound closure in diabetic foot ulcers overall, with especially strong effects in ulcers smaller than 5 cm². But the same analysis did not show stable benefit for amputation reduction, recurrence, or major safety outcomes, and the authors called for larger phase III multicenter trials with more standardized protocols. That is a meaningful positive signal, but it is still not the same thing as a definitive cure.
The same pattern is evidenced by broader summaries. Favorable effects for regenerative therapies in general were found from a 2025 network meta-analysis on diabetic foot ulcerations, and stem cells as promising adjunctive treatment options were noted from an umbrella-style review of lower-extremity ulcer therapies completed by ref (p). But the operative word here is “promising adjunctive”. They are being researched as adjunctive therapies with robust wound care, not alternatives to it.
The most important word is still “adjunct”
The IWGDF 2023 wound-healing guideline is particularly relevant as it ensures that the field remains (grounded. It says that interventions for the management of chronic wounds should be made in addition to multidisciplinary care, which has been done. Make sure you never miss a story from A-day; they are truly difficult to come by. Which is why stem cells for Chronic Wound are best utilized as part of a larger system of care involving correct debridement, pressure relief, control (when necessary) over infection treatment, vascular workup and metabolic balance. Wounds that are poorly vascularized, infected or repeatedly stressed day in and out cannot be healed just by virtue of the addition antibodies of a regenerative product.
Is “diabetes wound curable” the right question?
It is understandable, but medically too simple
The phrase diabetes wound curable captures the emotion of the problem, but it compresses a complicated reality into a yes-or-no headline. Some diabetic wounds do heal completely. Some heal only after intensive wound care, infection control, and vascular intervention. Some become chronic because the underlying drivers are still active. So the more useful question is not whether diabetes wounds are “curable” in the abstract, but whether the wound is being managed as a whole-limb, whole-patient problem. The CDC and IWGDF both make that broader approach very clear.
Stem cells may improve healing, but they do not erase the basics
This is where realistic writing matters. Stem-cell-based wound therapy may improve healing rates in selected patients, especially in diabetic foot ulcers, but it does not eliminate the need for standard wound care. In practice, the biology of chronic wounds is too layered for that. That is why the strongest current position is not “stem cells cure diabetic wounds,” but rather “stem cells may support wound healing in carefully managed cases.”
Why caution still matters
The science is promising, but regulation still matters
For this reason, the FDA remains concerned about patients who may receive stem cell and exosome products that are marketed without sufficient evidence or regulatory control to demonstrate their safety and effectiveness. The agency goes on to clarify that there are no exosome products approved by the FDA and adds any product marketed as a regenerative therapy may not demonstrate safety or efficacy. What this means is that FDA has generally been warning for some time now against the making of unsupported claims by companies selling exosome- and umbilical-cord-derived products. This is important because wound care falls into one of those categories where desperate need can dress weak claims up to sound convincing.
The most honest conclusion
Not the sales pitch; what is useful here, however, is truth. Stem Cell research for diabetic wounds holds promise and current studies indicate potential benefit in promotion of wound closure when using stem cells for Chronic Wound but only selected foot ulcers seem combinable with these treatment strategies. However, the field is still investigational; protocols are not fully standardized and treatment should stay as part of comprehensive wound care rather than above it. Therefore, if asked whether diabetes wound curable is the correct question to ask for honesty sake you should probably answer it no. The better question is whether the wound receives multidisciplinary treatment of a kind that actually gives healing even minimally realistic hope.