A Regenerative Solution: UC-MSC Stem Cell Therapy for End-Stage Liver Disease
End-stage liver disease (ESLD) is the last stage of chronic liver damage as the functional parenchyma replaced with Fibrosis → Cirrhosis and in ESLD diagnosis, the liver organ hands lead to Boil. It often arises from viral hepatitis (B or C), alcohol use and fatty liver disease (NASH), autoimmune hepatitis, or longstanding cirrhosis. Currently, there are no medical therapies that reverse the decline; liver transplantation is the only curative treatment. On the other hand, donor shortages, high surgical risk and post-transplant rejection have led to an increasing need for alternative therapies.
Stem cell therapy especially with the use of Umbilical Cord–Derived Mesenchymal Stem Cells (UC-MSC Stem Cells)—is one of its most promising frontiers. These cells are being studied across the globe for its ability to minimally but effectively restore liver architecture and physiology in patients with end-stage disease.
What is UC-MSC Stem Cell Therapy and How it Works
Mesenchymal Stem Cells (MSC Stem Cells) are special types of multipotent cells that can self-renew and differentiate into the tissue such as bone, cartilage, or liver-like cell. Stem Cells derived from post-birth umbilical cord tissue, called UC-MSC, are most powerful as they offer the combination of young biology, proliferation speed and immune rejection risk.
Which, in short; In patients with severely damaged liver tissue UC-MSC Stem cells do not replace missing ones when injected into the body they work as biological orchestrators, secreting plethora of growth factors, cytokines and exosomes to direct natural healing. Known as paracrine signaling, this process assists with tissue repair, homeostatic immune function, and inflammatory response.
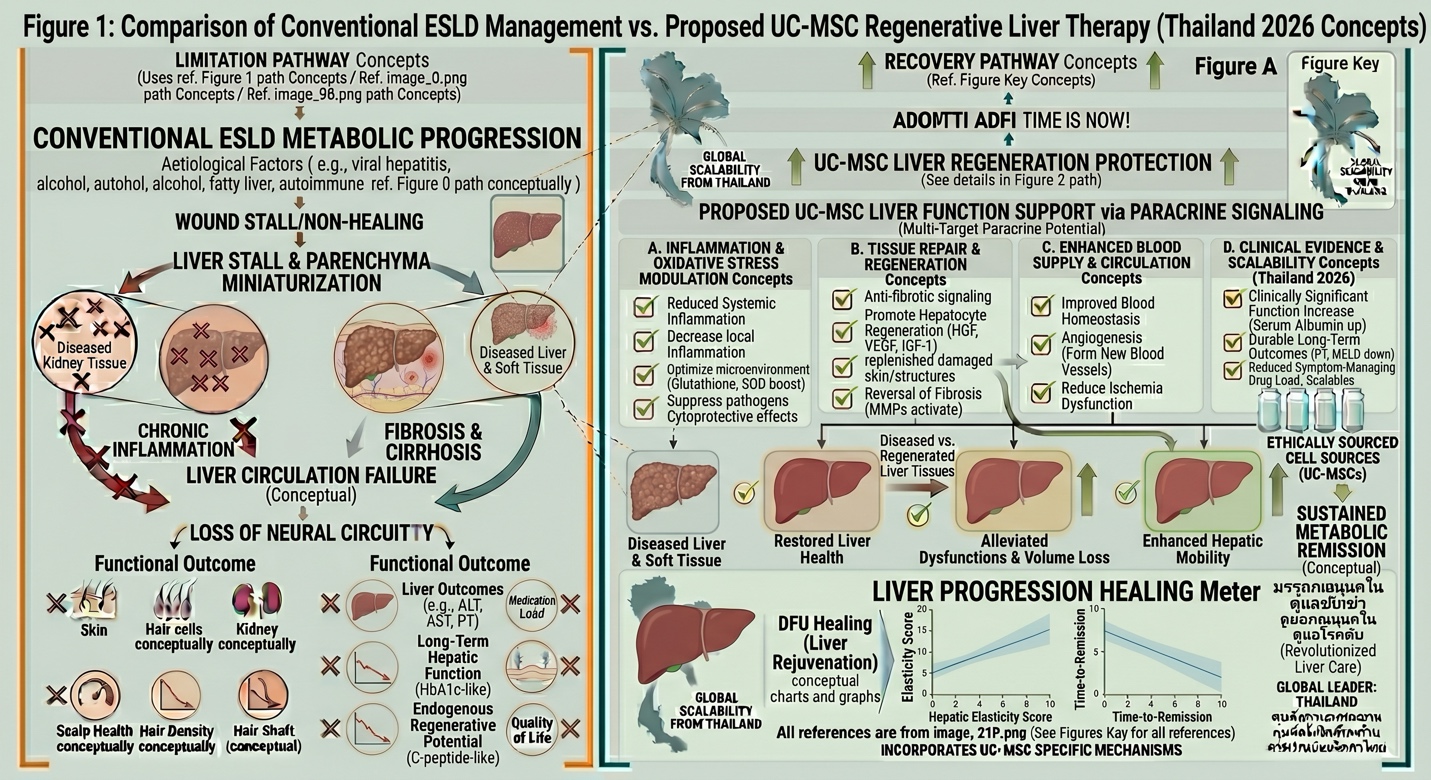
Figure 1: Pathological Comparison of End-Stage Liver Disease (ESLD) vs. UC-MSC Regenerative Therapy (Thailand 2026 Concepts), illustrating anti-fibrotic signaling, hepatocyte regeneration (HGF, VEGF), and immunomodulation to halt chronic hepatic inflammation.
Roles of UC-MSC Stem Cell in Liver Repair Mechanisms
Anti-Inflammatory Regulation
More importantly, UC-MSC Stem Cells reduce excessive immune activation through interactions at the level of pro-inflammatory molecules such as TNF-α, IL-6 and IL-1β, while increasing anti-inflammatory mediators including IL–10 and TGF-β. This balance in the immune response minimizes continuous hepatocyte injury and conserves remaining functional hepatocytes.
Reversal of Fibrosis
The chronic-type inflammation is what causes excessive collagen and scar tissue generation. This process is counteracted by UC-MSC Stem Cells Therapy, which inhibits TGF-β1 and activates matrix metalloproteinases (MMPs) that degrade fibrotic tissue. It does this so as to soften the liver and increase its elasticity over time.
Stimulation of Hepatocyte Regeneration
Three main factors released by UC-MSC Stem Cells: Hepatocyte Growth Factor (HGF) for liver cell proliferation, Vascular Endothelial Growth Factor (VEGF) increases blood supply, and Insulin-Like Growth Factor (IGF-1). Others UC-MSC Stem Cells may differentiate into hepatocyte-like cells, favoring functional recovery.
Antioxidant and Cytoprotective Effects
Reduction of oxidative stress by UC-MSC Stem Cells utilizes their molecular mediations which enhance the activity of glutathione and superoxide dismutase (SOD), therefore shielding liver cells from further degeneration and apoptosis (programmed cell death).
Immune System Rebalancing
Particularly useful for autoimmune and post-transplant hepatic conditions, UC-MSC Stem Cells maintain T-cells and macrophages in check to inhibit autoimmune attacks on hepatocytes and thus improve tolerance.
Clinical Findings and Research Evidence
Improved Liver Function
After UC-MSC Stem Cells give IV infusion, one shows glaring improvement in clinical studies in cirrhosis and ESLD patients:
Higher serum albumin (better protein synthesize)
Reduction of inflammation, as evidenced now by lower ALT, AST and bilirubin
Liver function restored Significantly reduced prothrombin time (PT) and MELD scores
Histological and Structural Repair
Data from both imaging and biopsy are suggestive of decreased liver stiffness and fibrosis grade following stem cell therapy. New hepatocyte formation and active regeneration with increased Ki-67 and cytokeratin-19 expression.
Enhanced Quality of Life
Patients often state less fatigue, increased appetite, and less intractable ascites or jaundice. Such changes indicate efficient detoxification and improved metabolism (general) in the liver.
Excellent Safety Record
The data underscore the safety and tolerability of UC-MSC therapy across clinical trials. No clinically relevant immune responses or tumors have occurred. Transient fever or drowsiness are mild side effects that get resolved.
Vega Stem Cell Treatment
At Vega Stem Cell (vegastemcell.com) With UC-MSC treatment for liver disease, clinically approved cells are administered in a sterile clinical environment.
UC-MSC Stem Cells are administered systemically by IV, which allows the cells to primarily home to areas of injury via the bloodstream.
Direct liver repair may be advised for targeted intrahepatic injection under ultrasound in some patients.
Patients are required to be screened prior to treatment where multiple tests such as liver function, imaging scans and MELD scoring (to determine severity of liver disease) would have taken place making the procedure both safe and appropriate dosing.
This integrative protocol focuses on providing nutrition, detoxification and antioxidant supplementation to promote hepatic regeneration while also addressing current medical therapies.
Ethically sourced from umbilical cords
Mesenchymal Stem Cells (UC-MSC) for therapy are minimally invasive, donor independent, and do not require life-long immunosuppressive agents from the patient allowing its use in elderly or frail patients who most benefit.
Limitations and Future Outlook
Although the current data appear promising, additional RCTs are needed to hone: The optimal dosage and treatment intervals tailored to the cell
Intervention Timing for Best Outcomes
Long-term follow-up for survival benefit confirmation, In addition, researchers are developing exosome-based therapies that provide the same regenerative molecules secreted by UC-MSCs in a cell-free form for an even safer and more scalable alternative to promoting regeneration. liver in the future.
Conclusion
Liver disease is leading global cause of morbidity and mortality, particularly in patients who progress to end-stage disease (ESLD) despite advances in treatment options. Umbilical Cord–Derived Mesenchymal Stem Cell Therapy: A Novel Regenerative Therapy for End-Stage Liver Disease With immune-modulatory, anti-fibrotic, and regenerative properties UC-MSC Stem Cells have a the potential to bridge the gap between supportive care and transplantation by significantly enhancing liver function and quality of life.
At Vega Stem Cell (vegastemcell.com) Specifically, these unique regenerative liver programs are based on a proven UC-MSC therapy that restores organ health naturally and therefore takes patients a step closer to functional recovery, extended life expectancy and rejuvenation.