Ulcerative Colitis (UC) is a type of chronic inflammatory bowel disease and is associated with immune-mediated injury to the colonic mucosa. It can be a debilitating illness, one that carves out an inordinate chunk of daily life of patients endure abdominal pain, fecal urgency, rectal bleeding, fatigue and weight loss, plus emotional distress from having chronic symptoms. Although helpful in inducing andmaintaining remission for many patients, moderate-to-severe disease remains challenging to manage in terms of persisting mucosal injury as well as therapy response that declines over time.
This has drawn growing interest in regenerative medicine and cell-based adjuvant therapies. Sputtering of inflammation suppression beyond this, whether biologic therapies bias up tissue repair in that, as well as restoring barrier and intestinal environment is an area — form exploring. Against this background, the investigators decided to explore mesenchymal stem cell–based approaches in ulcerative colitis.
- Pathophysiological Basis of Ulcerative Colitis
Ulcerative colitis, in very general terms, is a disease where the immune system reacts abnormally to the lining of the intestines and creates chronic inflammation of colon. The inflammatory process mainly involves the mucosa, resulting in ulceration, bleeding, edema and progressive loss of the epithelial barrier. Over the disease course, however, the colon is less able to maintain a stable and health surface ecologic environment promoting continued symptoms and periods of flare.
The clinical consequences can be profound. Diarrhea, abdominal cramping, rectal bleeding, anemia and fatigue and nutritional decline can occur frequently in patients. In chronic disease, lingering inflammation might also increase the risk for structural complications and colorectal neoplasia in the event that whatever underlying condition has resulted continues to be so irretrievably mismanaged over time. According to this perspective, preservation and restoration of mucosal integrity had become one of the major therapeutic targets for UC treatment.
The main antagonistic goal from a regenerative point of view, is to suppress not only immunity but also promote peroneal migration while remitting the cha injustice al barrier. That is the crux at which biochemical creativity has bloomed: investigators are now testing whether biologic therapeutics can facilitate a more homeostatic milieu for mucosal healing and epithelial restitution.
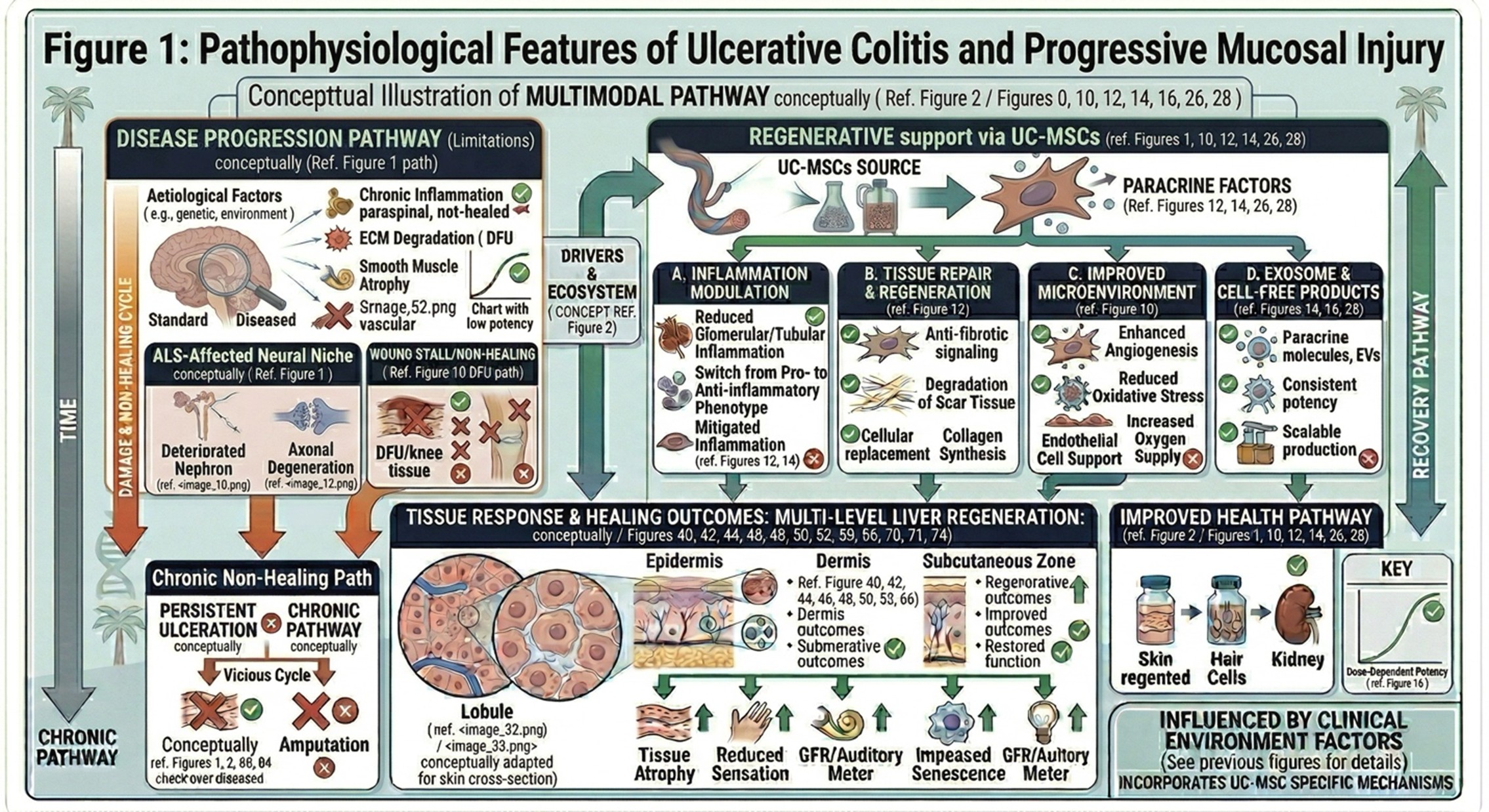
- Limitations of Conventional Therapy
S1 Progression of Ulcerative Colitis (UC) in Adults There are evidence-based guidelines defining the appropriate therapies for UC based on disease severity and treatment history, which include aminosalicylates, corticosteroids, immunomodulators and biologics. Such treatments can be absolutely critical and form the basis of standard-of-care. Their primary function is to decrease inflammation, manage symptoms and maintain remission.
However, important limitations remain. Corticosteroids have huge side effects when used long term, including bone loss, metabolic complication and risk of infection. Biologic and targeted therapies are effective but not all patients respond, some lose response over time or develop treatment limiting side effects. And even if inflammation is lessened, any damage to tissue may struggle to heal fully or swiftly.
That has created interest in treatment models that don’t only aim to suppress immune activity. So the question now is more than just how to quiet inflammation, but how best to support repair of the intestinal barrier and prepare a local milieu that is optimal for the types of repair that must follow. The broader therapeutic goal is also why regenerative approaches continue to garner attention.
- Biological Rationale for Stem Cell–Based Support in Ulcerative Colitis
Due to their immunomodulatory and tissue-supportive effects, stem cell–derived therapy is of interest in ulcerative colitis. The current interest primarily relates to mesenchymal stem cells (MSCs), of which studies are not directed solely toward their role as direct structural replacements, rather they have been investigated as biologically active features signaling cells that can regulate inflammation, the immune response, and repair pathways.
Following administration, MSCs are believed to exert a majority of their action through paracrine signaling. That is, they release cytokines, growth-related factors and extracellular vesicles that may help nudge inflammatory cells into a less harmful state. Within a setting of ulcerative colitis, such signaling may relieve the inflammatory load present in colon tissue and promote a normalized tissue environment.
An additional focus of interest is the capacity for these cells to facilitate mucosal healing via promotion of epithelial restitution and local regenerative responses. Instead of being framed as a panacea that guarantees reversal of disease, the almost contemporaneous and more sound science suggests that stem cell–based therapy may improve the conditions necessary to heal the intestinal barrier. To date, regenerative medicine has been discussed at the support strategy in selected cases of inflammatory bowel disease.
Figure 2: Proposed Immunomodulatory and Regenerative Mechanisms of Stem Cell–Based Therapy in Ulcerative Colitis
- Thailand and the Development of Regenerative Medicine
Thailand has long been notable in the realm of medical tourism and regenerative medicine as a result of its well-developed private healthcare system, infrastructure for international patients, and investment in research in areas such as biopharmaceuticals. The nation has continued to advance specialist wards integrating cutting-edge evaluation, encouraging treatment preparation and organized medical follow-up in GI and regenerative therapy.
Thailand is very much a lawyer in the world of overseas patients as it has access to hospital care, well-trained clinical personnel and reasonably low prices. Concurrently, continued investment in laboratory development and translational medicine has sustained interest in cell-based therapies as part of a broader innovation arc within healthcare.
Reiterating the biological significance of UC without mentioning regenerative strategies is lame. Severity of disease, response to previous therapy (where relevant), safety and the quality of the treatment program proposed are criteria used in clinical decision-making. Yet for patients with complex supportive mechanisms, oversight by a physician of medicine and appropriate expectations and integration into usual gastroenterology care should still prevail.
As regenerative medicine matures, cell-based supportive strategies may become more central to the ulcerative colitis dialogue — particularly as patients pursue biologically relevant approaches capable of longer disease management.

