The clinical management of chronic knee disorders is gradually shifting away from the pursuit of short-term symptom relief toward options that strive to facilitate structural recovery within the joint. During this transition, umbilical cord-derived mesenchymal stem cells (UC-MSCs) have been highlighted as a biologically active agent in regenerative orthopedics. Instead of just targeting immediate pain relief, this has been studied for its possible action on inflammation, cartilage support, synovial homeostasis and signaling in tissue repair. In specialized regenerative medicine clinics in Thailand, UC-MSC-based protocols are being integrated into advanced knee care programs aimed at addressing underlying joint deterioration in a more holistic fashion.
- Biological Basis of Knee Degeneration
Knee pain that stably lasts, by contrast, is often only the clinical expression of a more important degenerative process rather than merely an effect of age or exertion. With time, the articular cartilage may undergo structural breakdown, the synovial environment may be less protective and the joint can enter a cycle of mechanical load and low-grade inflammation. This process continues until you find it harder and harder to move and then normal day-to-day function slowly deteriorates.
In many patients, the degenerative cascade extends beyond cartilage thinning alone. The surrounding tissue milieu may likewise become metabolically detrimental, through reduced lubrication, inflammatory signaling molecules and altered local repair responses. This is a reason that chronic knee disease can be increasingly limiting. In regenerative medicine, UC-MSCs are being studied to potentially improve joint biological homeostasis prior to the point at which structural alterations reach a level where major surgical reconstruction may be an only or most viable treatment option.
This knee degeneration has significant impact on walking tolerance/exercise capacity, balance and quality of life. For decades, standard treatment guidance was largely based on short-term symptom-relief interventions. More recently, biologically targeted knee programs were developed in Thailand, that have fostered interest in whether regenerative strategies might aid load bearing by the joint over time.
- Chondrogenic Signaling and Synovial Environment Modulation
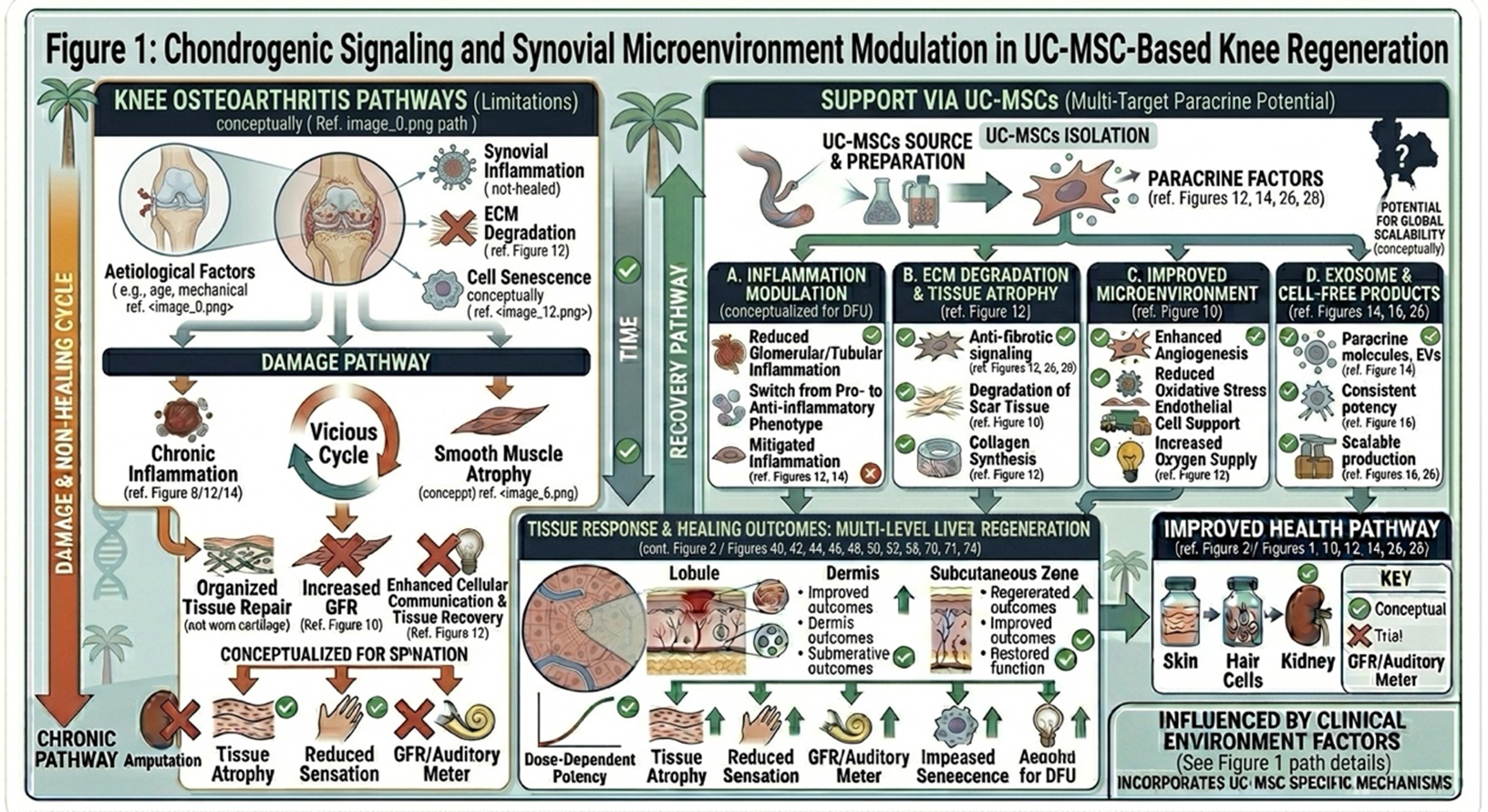
UC-MSCs are known to have greater chondrogenic potential than other MSC types and the ability to alter local joint atmosphere via paracrine signalling, and these properties make them candidate for use in regenerative knee treatments. The synovial space in a degenerative knee often becomes defined by inflammatory mediators, biochemical imbalance, and diminished support for normal tissue homeostasis. In those circumstances, the joint’s own ability to repair itself may become compromised.
UC-MSCs, when introduced into the intra-articular setting, are believed to function less as simple replacement cells and more as biological signaling mediators. They have been observed to secrete growth factors, trophic molecules and antiinflammatory mediators that promote synovial stability, dampen inordinate inflammatory responses and provide a more favorable environment for cartilage preservation. This is partly why regenerative clinicians speak of these cells working through a sort of “biological reset” in the diseased joint.
Their therapeutic mechanism is thus not linear only. Instead, for UC-MSCs a synergistic role is being explored through the modulation of endotype populations that control inflammation as well as positive support in matrix repair systems and overall biochemical environments required for better functional recovery of the joint.
- Evolving Beyond Conventional Orthopedic Symptom Management
The traditional management of chronic knee degeneration has provided some measure of pain relief for many patients, but its limitations are well known. Corticosteroids or viscosupplementation are injectable in nature and may alleviate pain or improve lubrication in the joint for varying length of time, but these modalities do nothing to address deeper tissue-level degeneration. They tend to play a supportive and temporary role instead of reconstructive.
At the other end of the treatment spectrum, total knee replacement might provide substantial benefit for patients with advanced disease; however, it is a major surgical intervention with demands imposed by recovery, rehabilitation efforts and the risk associated with any form of operative care. The gap that exists between conservative management through physical therapy versus major surgical intervention allows regenerative orthopedics to provide an intermediate treatment pathway.
In this regard, UC-MSC-based therapy is being evaluated as a potential minimally invasive treatment that may fill the gap between rehabilitation-based management and surgical reconstruction. The broader goal is to facilitate function, lower inflammatory burden, and possibly improve tissue quality in select people before irreversible decline takes over the joint.
- Regenerative Advantages of UC-MSCs in Knee Support
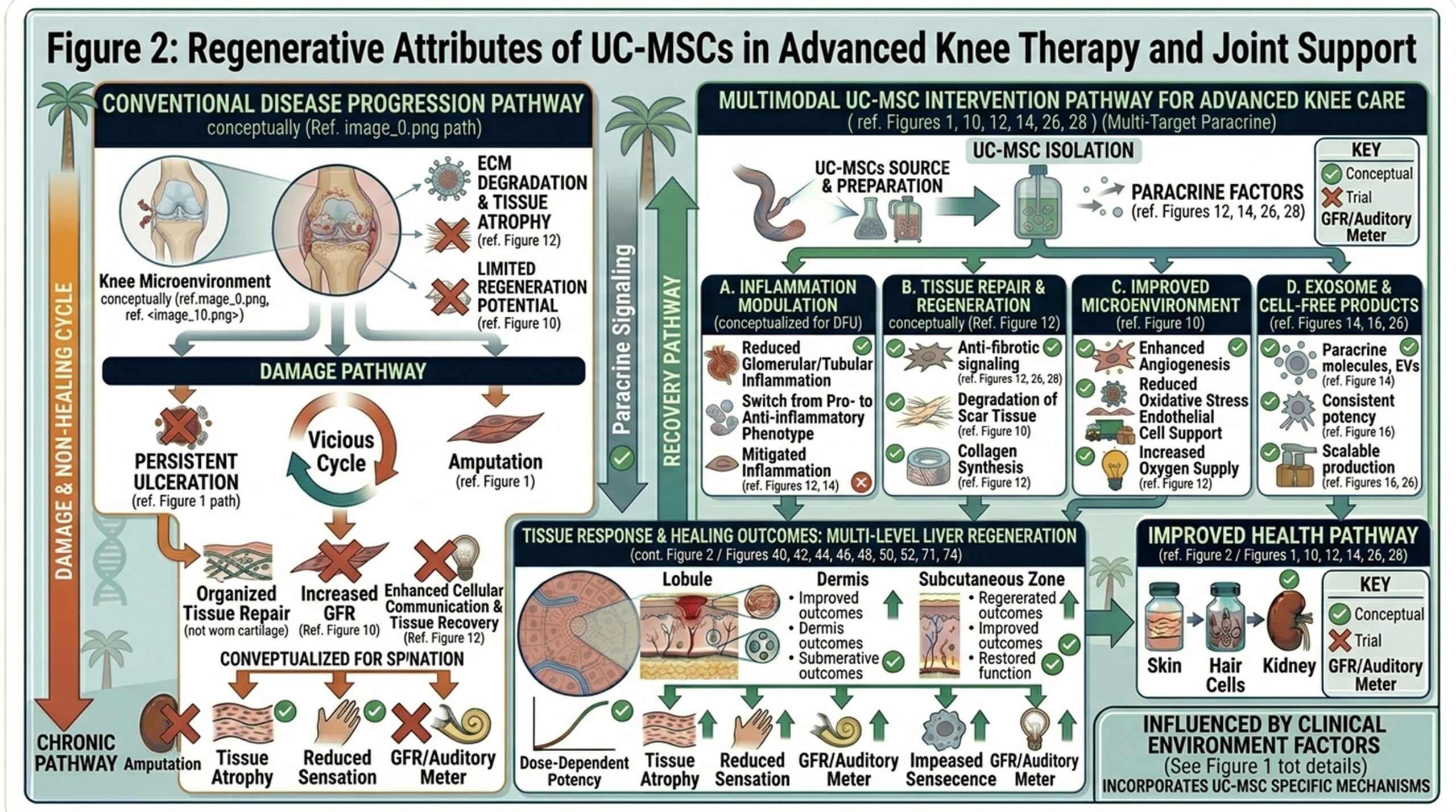
Due to the biological youth and high activity of data for various signalings, UC-MSCs are usually giving priority in regenerative programs. In comparison to many cell populations derived from adults, these cells are reported as having strong proliferative potential and a vigorous secretary profile that may be pertinent in tissues suffering from chronic use and degeneration.
As such, there are a few potential regenerative contributions usually discussed for knee-directed care. One group is support for cartilage matrix maintenance, including pathways related to collagen production and chondrocyte-related signaling. A second is the modulation of the synovial lining and inflammatory environment that may help reduce ongoing biochemical stress on joint pain and stiffness. Alongside their ability to interact with meniscal and connective tissue healing settings, UC-MSCs have established an interest in joint environments having structural strain beyond just cartilage.
Instead of a promise for full reversal of advanced degeneration, the more credible regenerative perspective is that these cells may help reinforce the biological milieu necessary for better joint support. In the clinic, this might lead to them taking goals like pain relief, increased mobility, better function, and slowed progression in select patients.
- Thailand’s Role in Advanced Regenerative Orthopedic Care
Expanding in this field, Thailand is getting the attention due to clinical expertise, laboratory capability and international patient care infrastructure. In the field of orthopedic applications, this has provided impetus for expansion of specialized programs that are incorporated into biologic treatment pathways, through imaging guidance, rehabilitative planning and tailored procedural strategy.
One of the main practical contributions for advanced knee treatment is the implementation of image-based injections, notably ultrasound-guided injection placement. This provides a more specific methods for joint space or surrounding structure targeting, which can be especially advantageous in regenerative techniques where the outcome quality may depend on the location of delivery. Precise placements are most often considered a cornerstone of contemporary orthobiologic care.
Factors like cell handling standards, viability, sterility and consistency of protocol are another determining reason why regenerative centers in Thailand excel. These operational factors are important considerations as the quality of a cell-based intervention is dependent not only on the cell source, but also on the means of how the product is prepared, delivered and incorporated into an overall treatment plan.
- Concluding Perspective
The introduction of UC-MSC-based therapy into the clinical management of chronic knee disease also mirrors a broader paradigm shift in musculoskeletal medicine. Instead of concentrating solely on pain suppression or surgical replacement at the latest stages, regenerative orthopedics is increasingly looking at how to support the biological bedrock of joint health itself. UC-MSCs are of particular interest in this regard, with mechanisms involving the modulation of inflammation, support for synoviocytes (the cells lining the joint), tissue signaling and matrix preservation.
These strategies are underway and a fundamental part of a more precise and biology driven model of knee therapy in advanced clinical settings in Thailand. At the same time, responsible interpretation is key. UC-MSC-based treatment should be considered as an adjunctive regenerative treatment still under clinical development rather than a definitive solution for all type of knee degeneration. Used as described in selective conditions and in structured medical protocols, however, this strategy may provide a science-based approach to enhance mobility, alleviate pain and more prolonged joint support over time.

