Stem Cell Therapy Thailand UC-MSCs Innovations Cerebral Palsy
- Introduction, Origins, and Impact
Cerebral Palsy is a major neurodevelopmental disorder affecting children. It is caused by permanent malformations or devastating injuries to the developing brain while in utero or in the early postnatal period. The injuries lead to permanent brain damage which entails deficits in motor, postural and balance control along with frequent deficits in cognition. It is a condition emotionally and financially traumatizing for affected families. It is so severe that the affected individual will need to remain dependent for the rest of their life, and will never achieve any degree of independence. For years, the medical community has focused on symptomatic relief via the use of medications and physical therapy. These approaches are seen as a failure since they do not and cannot address and modify the structural deficits of the central nervous system. Because of the pressing need for alternatives, there has been a renewed interest in the field of the regenerative medicine. In this regard, UC-MSCs have shown promise in repairing the central nervous system. Stem Cell Therapy Thailand offers the prospect of moving beyond traditional therapies, and instead, offer true neurological repair.
- Pathogenesis, Mechanism of, and Life-Long Consequences
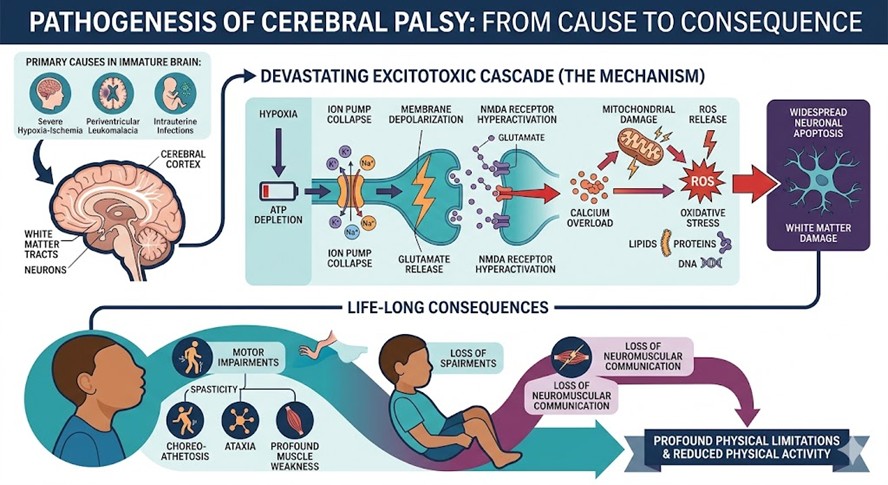
The main causes of this Cerebral Palsy condition are immature brain from severe hypoxic-ischemic encephalopathy, periventricular leukomalacia, and intrauterine infections. If the developing brain suffers from severe hypoxia, there is a devastating and unrepairable chain reaction. Hypoxia causes the rapid depletion of cellular ATP, and leads to the instantaneous collapse of energy dependent ion transport systems. Every failure initiates a profound amount of membrane depolarization that releases large amounts of the excitatory neurotransmitter, glutamate, into the extracellular space. Glutamate releases N-methyl-D-aspartate receptors (NMDA) which lead to uncontrolled calcium (Ca2+) influx into fragile neurons. Intracellular calcium overload acts as the cell’s primary executor dismantling the cell’s mitochondria which releases highly reactive oxygen species (ROS). Oxidative stress causes the destruction of the cell’s lipids, nucleic acids, and structural proteins. The excitotoxic cascade results widespread neuronal apoptosis and significant damage to the brain’s white matter tracts. The cellular damage results in the loss of the brain’s spasticity, choreoathetosis, and ataxia, as well as profound muscle weakness. The significant brain damage results in the loss of impact of neuromuscular communication. This results in a life of little to no physical activity and profound physical limitations.
- Traditional Treatment Modalities and Inherent Limitations
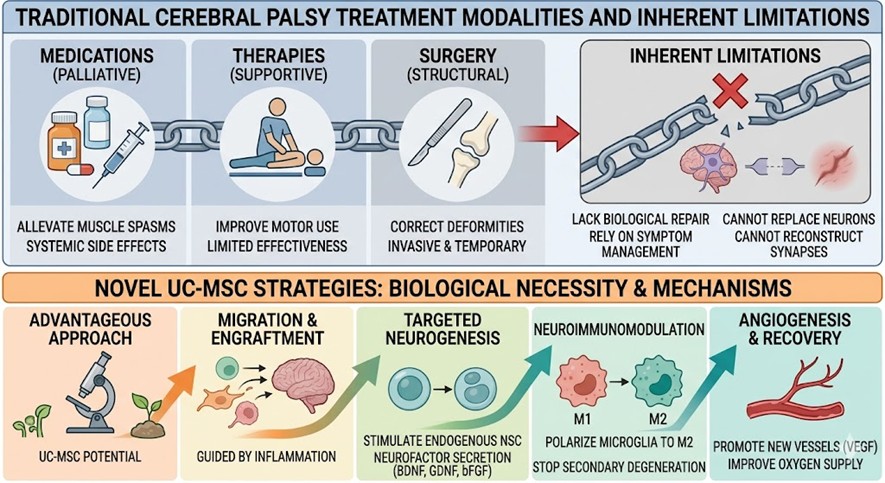
Treatment for Cerebral Palsy has predominantly been based on a series of limitations until now. Most of the time, physicians use medications such as oral baclofen, tizanidine, or benzodiazepines to alleviate severe muscle spasms. Botulinum toxin injections paralyze certain muscle groups and also reduce focal dystonia. Extensive physical, occupational, and speech therapy remains the most important factor in the preservation of effective motor use and in the prevention of the formation of serious joint contractures. In the event of serious injuries, orthopedic surgery also becomes necessary to lengthen tendons, realign bones, and to correct serious spinal curvature. Before surgery, most of the time, these methods have limited scope of development. The most serious and problematic of these is that they have to rely on palliative means. They completely lack the biological mechanisms necessary to process and replace lost neuronal populations, reconstruct broken synaptic connections, or qualitatively transform the underlying neuropathological landscape.
- Biological Necessity and Mechanisms of Novel Strategies
The scientific community is more certain that to address the primary cellular injuries involved, exceedingly sophisticated regenerative mechanisms will be required. In this regard, the use of UC-MSCs has begun to be viewed as a more advantageous Cerebral Palsy approach because of their unmatched immunomodulatory and strong neurotrophic effects. When clinicians inject these multipotent cells, they migrate towards certain zones of the ischemic brain injury, guided by complex inflammatory chemokine gradients. After engraftment, UC-MSCs take on their therapeutic role mainly by paracrine signaling. They produce and release large quantities of important neurotrophic factors, such as brain-derived neurotrophic factor, glial cell line-derived neurotrophic factor, and basic fibroblast growth factor, which profoundly stimulate the proliferation and differentiation of the resident neural stem cells to transform them into mature and functional neurons to replace the apoptotic cell populations. In addition, UC-MSCs markedly influence the hostile neuroinflammatory milieu. They release anti-inflammatory cytokines that change resident microglia from the severely damaging M1 phenotype to the highly neuroprotective M2 phenotype. Macrophage polarization of this type effectively stops ongoing secondary neurodegeneration. Additionally, they produce and release strong angiogenic factors, such as vascular endothelial growth factor, which promote the development of new capillary networks. This sustained and robust neovascularization also restores, and very importantly, improves the supply of oxygen and other nutrients to the brain tissue that is previously ischemic. Because of its particular combination of targeted neurogenesis, powerful immunomodulation, and robust angiogenesis, this Stem Cell Therapy approach is markedly superior to previous methods.
- Upcoming trends and competitive benefits of home-grown therapies
The future trajectory of utilizing UC-MSCs in complex neurodevelopmental disorders like Cerebral Palsy is gaining an important foothold in Southeast Asia and is highly encouraged by the changing paradigm of regenerative protocols in the international medical community. Patients around the world traveling for Stem Cell Therapy Thailand are changing south east Asian bioethics. Thailand’s biomedical engineering centers are the best in the world in the world for cell culturing and practicing bioengineering with some of the best laboratory management. The country attracts an elite international medical researcher community and collaborates in the best cell therapy and cell intervention and best neurorehabilitation rehabilitation medical science and best patient surgical and best physiotherapy medical science. This remarkable blend of advanced technology with qualitative and regulatory protection and the best of science and the best humanitarian patient care establish Southeast Asia as a leading area of specialized care to treat challenging conditions of the nervous system.

