Advanced UC-MSCs Therapy for Rheumatoid at a Premier Stem Cell Clinic Thailand
Chronic autoimmune conditions present a significant challenge to global healthcare systems with Rheumatoid arthritis standing as one of the most debilitating inflammatory disorders. This systemic condition is characterized by the body’s immune system mistakenly attacking the synovial tissues within joints, leading to progressive bone erosion, functional disability, and chronic pain. Beyond the physical limitations, the systemic nature of the disease often affects internal organs including the heart and lungs, significantly reducing the quality of life and life expectancy of those afflicted. While pharmacological interventions have evolved over decades, many patients remain non-responsive to existing biological therapies or suffer from severe side effects associated with long-term immunosuppression. This clinical gap has necessitated the exploration of regenerative medicine, specifically the application of UC-MSCs as a transformative therapeutic strategy. Using mesenchymal stem cells derived from the umbilical cord offers a potent immunomodulatory alternative that aims not just to manage symptoms but to reset the underlying immune dysregulation.
Pathophysiological Mechanisms and Clinical Manifestations of Autoimmune Joint Destruction
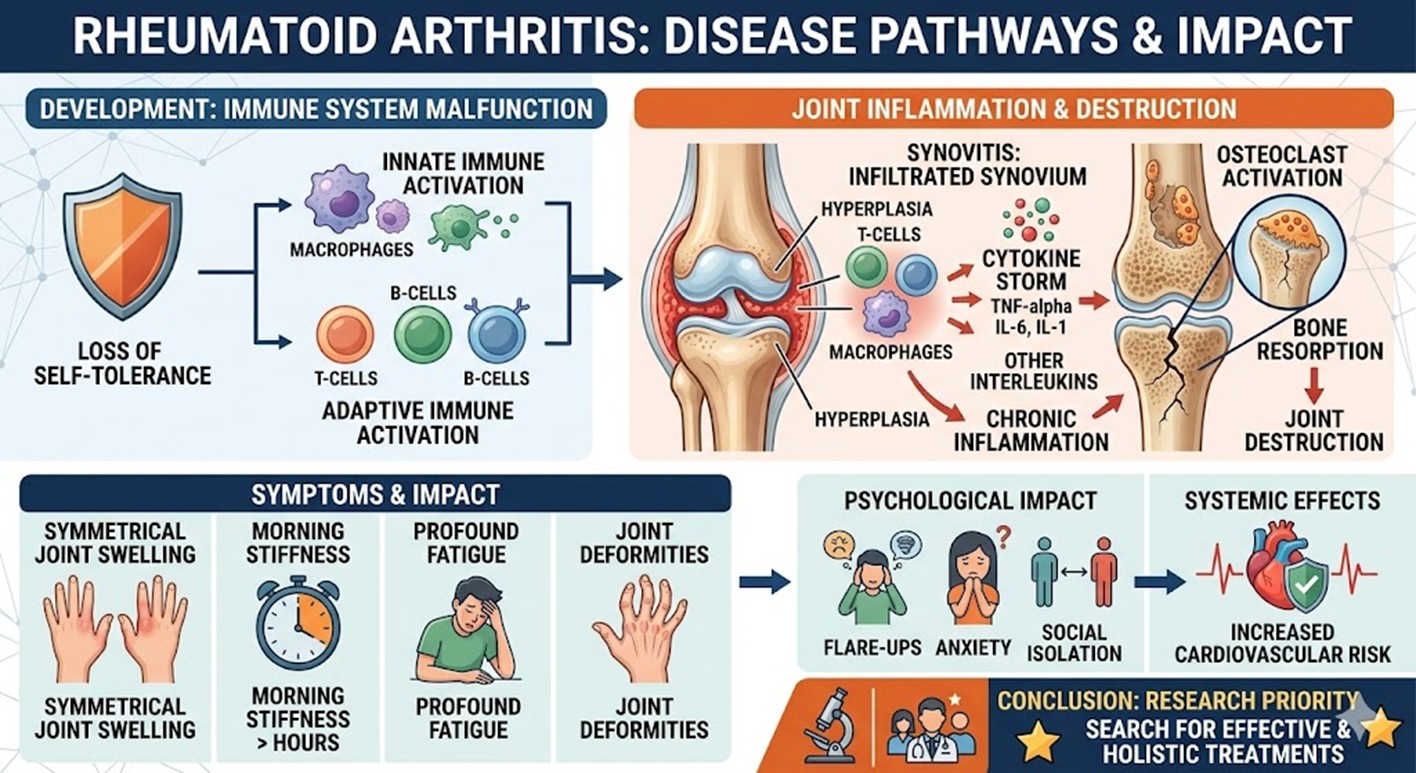
The development of Rheumatoid arthritis is a complex process involving a loss of self-tolerance and the activation of both innate and adaptive immune responses. The primary site of injury is the synovium, which undergoes massive hyperplasia and becomes infiltrated by inflammatory cells such as T-cells, B-cells, and macrophages. These cells secrete a cocktail of pro-inflammatory cytokines, most notably Tumor Necrosis Factor-α and various Interleukins, which sustain a state of chronic inflammation. This environment triggers the activation of osteoclasts, the cells responsible for bone resorption, leading to the irreversible joint destruction seen in advanced stages.
Patients typically experience symmetrical joint swelling, morning stiffness lasting several hours, and profound fatigue. As the disease progresses, the inflammatory process can lead to joint deformities that make simple daily tasks impossible. The psychological impact is equally severe, as the unpredictability of flare-ups often leads to anxiety and social isolation. Furthermore, the systemic inflammatory state increases the risk of cardiovascular disease, making the search for more effective and holistic treatments a high priority for the medical community.
Current Therapeutic Approaches and the Limitations of Conventional Management
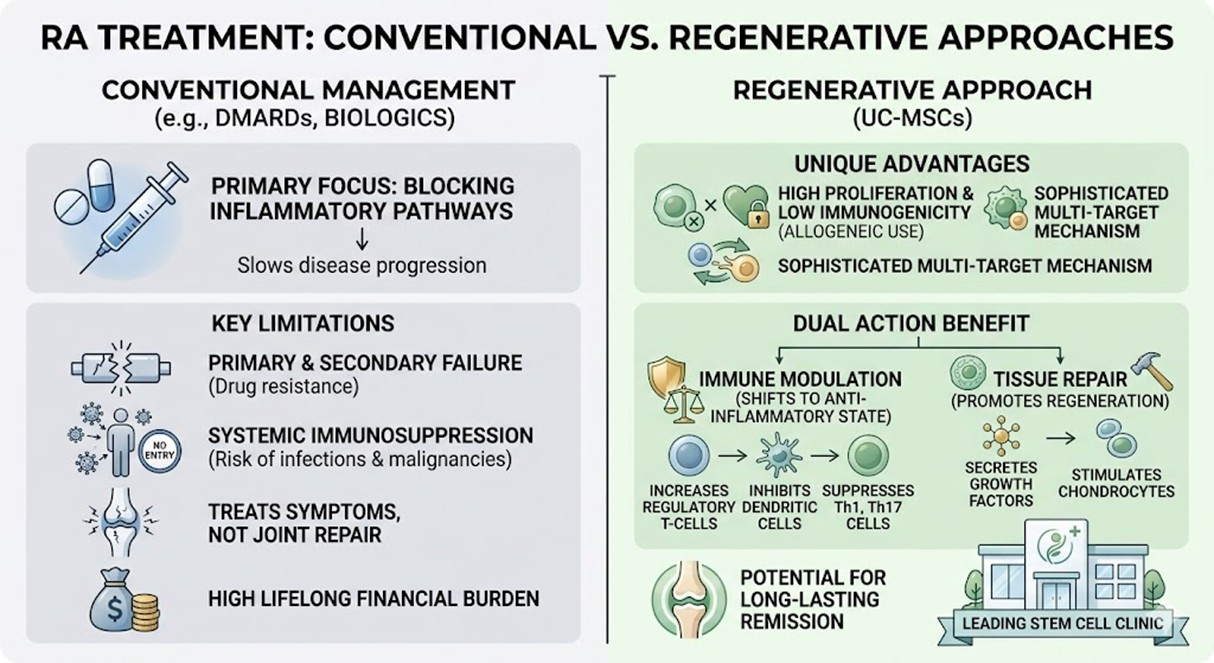
The traditional management of Rheumatoid arthritis relies heavily on Disease-Modifying Anti-rheumatic Drugs and biological agents. While these treatments have revolutionized patient outcomes by slowing disease progression, they are far from perfect. Many patients experience primary or secondary failure, where the drugs either never work or lose their efficacy over time. Additionally, because these medications suppress the entire immune system, they leave patients highly vulnerable to serious infections and certain malignancies.
Furthermore, conventional therapies focus primarily on inhibiting specific inflammatory pathways rather than repairing the damage already sustained by the joint tissues. They do not address the fundamental imbalance of the immune system’s regulatory cells. The financial burden of lifelong biological therapy is also substantial, often creating a barrier to consistent care. These limitations emphasize the urgent need for a more targeted, regenerative approach that can provide long-lasting remission without the systemic toxicity associated with daily pharmacological intervention.
The Regenerative Potential and Immunomodulatory Mechanism of UC-MSCs
Transitioning toward UC-MSCs represents a paradigm shift in treating autoimmune pathologies. Umbilical cord-derived mesenchymal stem cells possess unique biological advantages, including a high proliferative capacity and low immunogenicity, which allows them to be used in allogeneic transplants without the need for strict HLA matching. At a leading Stem Cell Clinic Thailand, these cells are utilized for their sophisticated multi-targeted mechanism of action. Unlike traditional drugs that block a single pathway, these stem cells interact dynamically with the patient’s microenvironment.
The core mechanism involves the secretion of bioactive molecules and direct cell-to-cell contact that shifts the immune profile from a pro-inflammatory state to an anti-inflammatory one. Specifically, they induce the production of Regulatory T-cells, which are essential for maintaining immune tolerance. They also inhibit the maturation of dendritic cells and suppress the overactivity of Th1 and Th17 cells, effectively dampening the cytokine storm within the joints. Beyond immune modulation, these cells promote tissue repair by secreting growth factors that stimulate the resident chondrocytes to regenerate damaged cartilage, offering a dual-action benefit that conventional medicine cannot match.
Future Trajectory of Mesenchymal Stem Cell Applications within the Thai Medical Landscape
The outlook for utilizing UC-MSCs to combat Rheumatoid arthritis in the Southeast Asian region is exceptionally promising, with Thailand positioning itself as a central hub for this innovation. Choosing a Stem Cell Clinic Thailand provides patients with access to world-class laboratory facilities and specialized medical expertise that adheres to rigorous international standards. Thailand has invested heavily in biotechnology infrastructure, ensuring that the processing and cultivation of these cells maintain the highest purity and potency levels.
The future of this therapy in Thailand is moving toward personalized regenerative protocols, where the dosage and delivery methods are tailored to the specific inflammatory markers of the individual. As more clinical data emerges from Thai institutions, the integration of stem cell therapy into standard clinical practice is expected to accelerate. The country’s unique combination of high-tier medical hospitality, advanced research capabilities, and a supportive regulatory framework for cellular therapies makes it a premier destination for patients seeking the next generation of autoimmune treatment.
In summary, the transition from managing symptoms to achieving genuine immune restoration is the hallmark of modern regenerative medicine. The application of UC-MSCs offers a sophisticated solution to the complex challenges posed by Rheumatoid arthritis, addressing both the inflammatory triggers and the need for structural repair. By moving beyond the limitations of traditional immunosuppressants, this therapy provides a pathway toward long-term stability and improved physical function. For those seeking these advanced interventions, a specialized Stem Cell Clinic Thailand stands as a beacon of hope, combining cutting-edge science with a compassionate, patient-centered approach. As research continues to refine these protocols, the potential to significantly alter the disease course for millions of patients becomes increasingly tangible, marking a new era in the fight against autoimmune destruction.

