Chronic ulcerative wounds typically develop when the body’s natural healing mechanisms become impaired, preventing damaged tissue from repairing itself efficiently. Patients frequently experience prolonged discomfort, recurrent infections, reduced mobility, and in severe cases, the risk of limb amputation.
In recent years, regenerative medicine has introduced new possibilities for treating chronic wounds. Among the most promising developments is stem cell therapy, particularly treatments involving mesenchymal stem cells derived from umbilical cord tissue (UC-MSCs). Rather than simply managing symptoms, regenerative therapies aim to stimulate the body’s natural repair processes and rebuild damaged tissue. This shift from supportive care to biological regeneration is transforming how clinicians approach chronic ulcer treatment.
The Role of Stem Cells in Tissue Repair
In the context of wound healing, stem cells provide benefits through two major mechanisms. The first involves direct tissue regeneration. Stem cells can transform into specialized cells needed to rebuild damaged structures, such as skin cells, connective tissue cells, or cells lining blood vessels. These new cells help restore the integrity of the injured area.
The second mechanism involves paracrine signaling. Stem cells release a variety of bioactive molecules—including growth factors, cytokines, and chemokines—that influence nearby cells. These signaling compounds stimulate surrounding tissues to participate in repair, regulate inflammation, and improve immune responses. Even if stem cells do not permanently integrate into the tissue, the molecules they release can significantly accelerate healing.
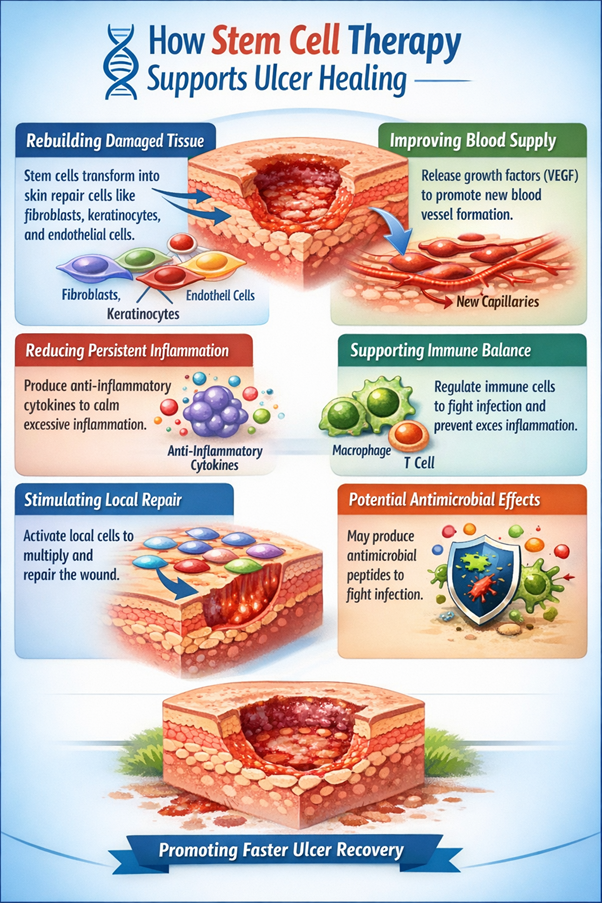
How Stem Cell Therapy Supports Ulcer Healing
- Rebuilding Damaged Tissue: Stem cells have the ability to develop into various types of cells involved in skin repair. These include fibroblasts, which produce connective tissue components such as collagen, keratinocytes that form the outer protective layer of skin, and endothelial cells responsible for creating new blood vessels. By generating these essential cell types, stem cells help rebuild ulcerated tissue from the inside outward.
- Improving Blood Supply: Stem cells release growth factors such as vascular endothelial growth factor (VEGF), which encourages the formation of new capillaries. This process, known as angiogenesis, improves blood supply to the damaged region and supports faster recovery.
- Reducing Persistent Inflammation: Stem cells produce anti-inflammatory molecules, including cytokines such as interleukin-10 and transforming growth factor beta. These substances help calm excessive inflammatory responses and shift the wound environment toward tissue repair rather than ongoing damage.
- Supporting Immune Balance: Stem cells also interact with immune cells such as macrophages and T lymphocytes. Through these interactions, they help regulate immune activity, improving the body’s ability to eliminate infection while preventing excessive inflammation that could delay healing.
- Stimulating Local Repair Mechanisms: The signaling molecules released by stem cells can activate nearby skin and connective tissue cells. These signals encourage local cells to multiply, migrate to the wound site, and participate in rebuilding tissue. In this way, stem cells act as biological coordinators that guide the overall healing process.
- Potential Antimicrobial Effects: Some scientific studies suggest that stem cells may produce antimicrobial peptides capable of inhibiting certain pathogens. These properties could help reduce infection risk and support faster wound recovery.
Advantages of Regenerative Stem Cell Therapy
Stem cell-based treatments offer several important benefits compared with conventional wound care.
One major advantage is the ability to promote full-thickness tissue regeneration. Rather than simply removing damaged tissue, stem cells help reconstruct the layers of skin and underlying structures. This comprehensive repair can improve both function and durability of the healed area.
Another benefit is reduced scarring. Because stem cells help guide the formation of organized tissue, the regenerated skin often appears more natural and flexible, minimizing fibrotic scar formation.
Faster recovery also reduces the risk of infection and other complications. As wounds close more rapidly, they become less vulnerable to microbial invasion. Additionally, regenerated tissue may be stronger and more resilient, lowering the chance of ulcer recurrence.
In severe cases, regenerative therapies may even help prevent limb amputation by restoring circulation and tissue integrity before irreversible damage occurs.
Research and Clinical Evidence
Clinical research examining stem cell therapy for chronic wounds has produced encouraging results. Early-phase clinical trials involving patients with diabetic foot ulcers and venous leg ulcers have demonstrated faster wound closure, improved tissue structure, and reduced ulcer size following stem cell treatment.
Meta-analyses comparing stem cell therapy with conventional care have found higher healing rates among patients receiving regenerative treatments. Importantly, these studies have also reported favorable safety profiles when stem cells are administered under controlled medical conditions.
Research focusing on pressure ulcers has also shown improvements in blood vessel formation and tissue regeneration, highlighting the potential of stem cell therapy across multiple wound types.
Conclusion
Stem cell therapy represents a significant advancement in the treatment of chronic ulcers. Instead of focusing solely on infection control and wound management, regenerative medicine targets the underlying biological problems that prevent healing. By stimulating blood vessel growth, reducing inflammation, restoring tissue structure, and regulating immune responses, stem cells help re-activate the body’s natural repair mechanisms.
As research progresses and clinical techniques continue to improve, stem cell-based therapies are likely to play an increasingly important role in wound care. These treatments hold the potential to accelerate healing, reduce complications, preserve limbs, and ultimately improve the quality of life for patients suffering from chronic ulcerative conditions.

