Healthy brain function depends on coordinated activity across multiple systems including immune balance, inflammation control, the gut–brain axis, metabolic signaling, blood flow, and neural connectivity. When these systems are well-regulated, the brain is better able to support attention, learning, communication, sleep, and emotional regulation.
In recent years, regenerative medicine has begun exploring new ways to support neurological and neuroimmune health at a cellular level. One area of growing interest involves umbilical cord–derived mesenchymal stem cells (UC-MSCs). UC-MSCs are studied because they release bioactive molecules, help regulate immune responses, and can support tissue repair processes. For autism spectrum disorder (ASD), stem cell therapy is being investigated as a supportive approachthat may help improve the internal environment that influences brain and nervous system function. Outcomes vary widely, and research is still evolving.
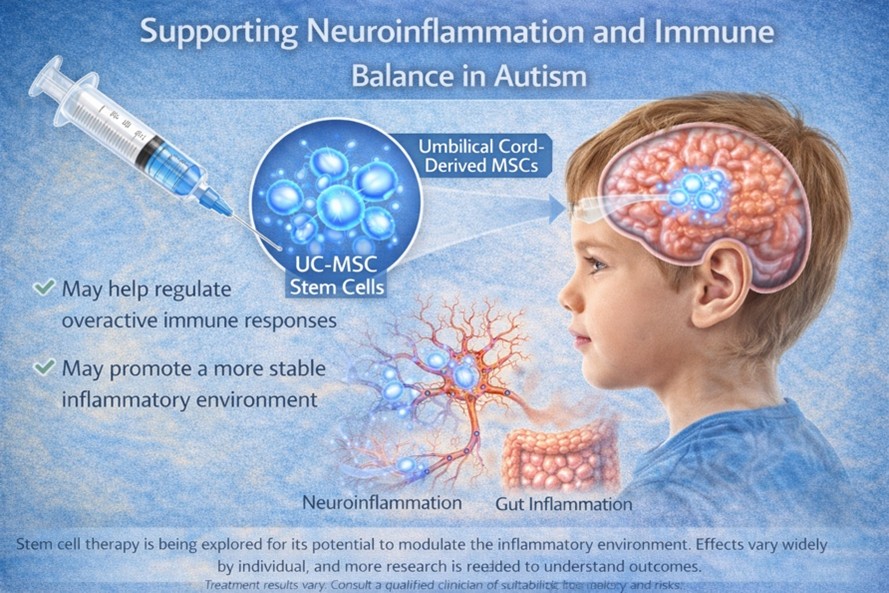
Supporting Neuroinflammation and Immune Balance
Many researchers have explored the role of immune dysregulation and chronic low-grade inflammation in some individuals with ASD. When inflammatory signaling is elevated, it may affect brain function, sleep quality, sensory processing, and behavior.
UC-MSCs are being studied for their immunomodulatory effects, meaning they may help calm excessive immune activity and support a more balanced inflammatory response. By reducing inflammatory signaling, stem cell therapy may support a more stable neuroimmune environment, which could potentially translate into improvements in daily functioning for some individuals. However, responses differ and are not guaranteed.
Promoting Healthier Communication Between Brain Cells
Brain function relies on efficient communication between neurons and supportive brain cells (such as glial cells). When inflammation or oxidative stress disrupts this environment, neural signaling may become less efficient.
UC-MSCs release a range of growth factors and signaling molecules that may help support neural protection and recovery processes. Rather than directly “changing” the brain, this approach is studied for how it may support the conditions needed for healthier signaling, including reduced inflammatory stress and improved cellular support.
Supporting the Gut–Brain Axis and Systemic Metabolic Health
The gut–brain axis plays an important role in neurodevelopment. Many individuals with ASD experience gastrointestinal issues, food sensitivities, or altered gut microbiome patterns. Ongoing gut inflammation can influence immune activity and may affect mood, sleep, and behavior.
Because UC-MSCs may help regulate inflammation systemically, they are being explored for their potential to support gut-related inflammation and overall metabolic balance. A healthier internal inflammatory environment may also help improve how the body processes nutrients, responds to stress, and maintains energy stability—factors that can influence day-to-day functioning.
Encouraging Healthier Tissue Repair and Oxidative Stress Control
Oxidative stress (an imbalance between free radicals and antioxidant defenses) has been studied in relation to neurodevelopmental conditions. Excess oxidative stress can strain cellular health and disrupt normal signaling.
UC-MSC therapy is being investigated for its potential to support tissue repair pathways and reduce damaging inflammatory cascades that contribute to oxidative stress. By supporting cellular resilience and repair mechanisms, the therapy may help improve overall physiological stability, which can be meaningful for individuals with complex neurodevelopmental needs.
Supporting Sleep, Attention, and Behavior Through Better Physiological Regulation
Many autism-related challenges—such as sleep disruption, irritability, attention difficulties, and sensory sensitivity—can be influenced by underlying inflammation, immune imbalance, gut discomfort, or metabolic instability.
By supporting immune regulation and reducing inflammatory signaling, UC-MSC–based therapy may help improve physiological balance. In some cases, this may contribute to better sleep quality, improved comfort, and enhanced participation in therapy, learning, and daily routines. These effects are highly individual and should be viewed as potential supportive benefits rather than guaranteed outcomes.
Figure 2: Supporting Sleep, Attention, and Behavior Through Better Physiological Regulation.
Supporting Long-Term Development Alongside Behavioral Therapies
Autism care is often most effective when it is comprehensive, including behavioral therapy, speech and occupational therapy, nutritional support, and individualized medical care. If stem cell therapy is considered, it is best viewed as an adjunct approach—aiming to support the body’s internal environment so the individual can better engage with ongoing therapies.
This broader concept focuses on improving “readiness for learning and development” through better regulation of inflammation, immune balance, sleep, and general well-being.
Conclusion
Umbilical cord–derived mesenchymal stem cells represent an emerging area of research in autism and neurodevelopmental support. Through immune modulation, inflammation reduction, and the release of beneficial signaling molecules, UC-MSC–based approaches are being investigated for their potential to support neurological and systemic balance.
While early research is still developing and outcomes vary, stem cell therapy may offer a supportive strategy for selected individuals—particularly when combined with structured therapies and personalized medical oversight. A thorough consultation with a qualified practitioner is essential to assess suitability, safety, and realistic expectations.

